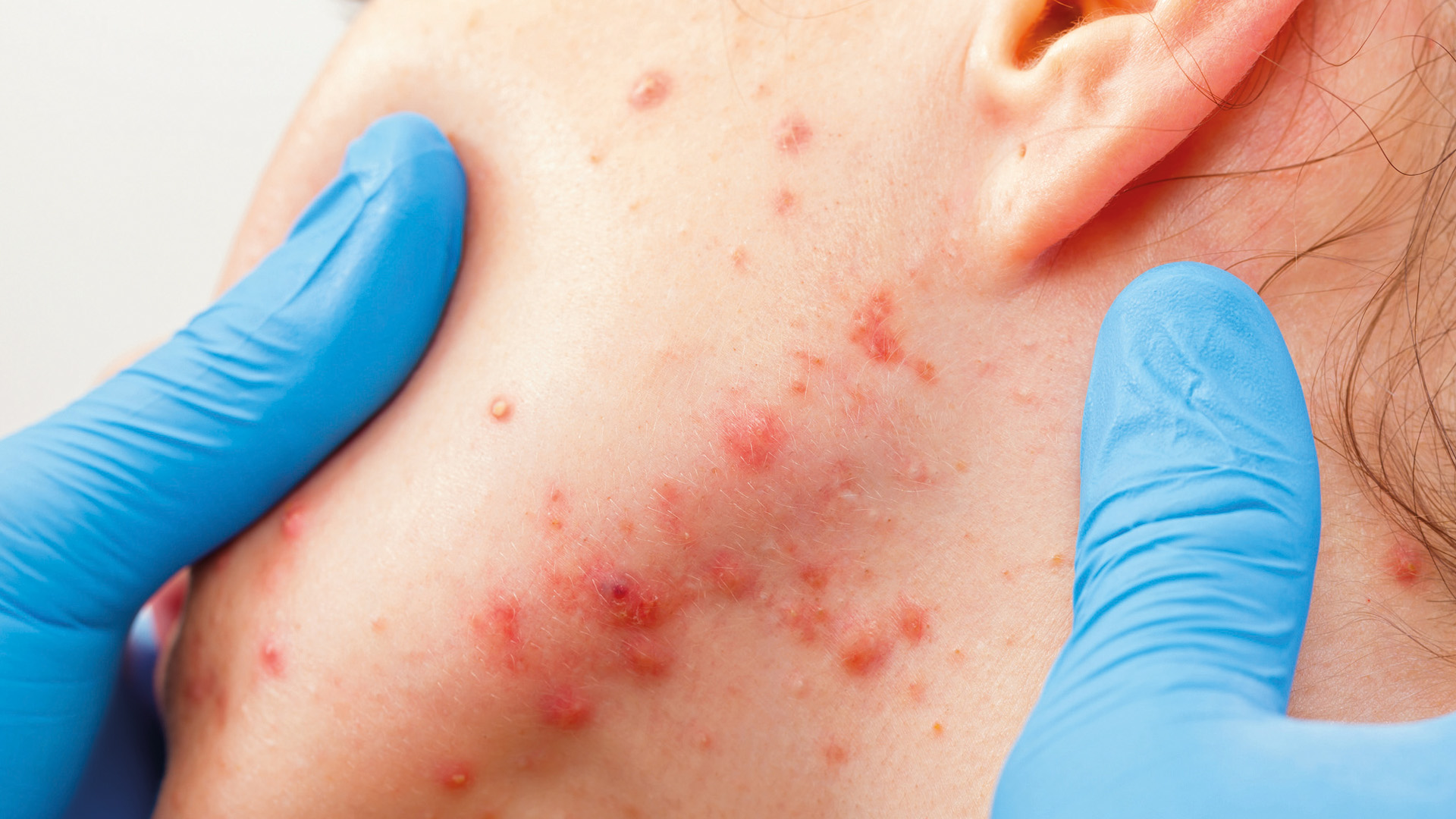
In OTC
Follow this topic
Bookmark
Record learning outcomes
A new NICE guideline on the management of acne brings together many key points for effective management. Consider some of the main elements of the guidance and suggests some action points for community pharmacy
The new NICE guideline aims to make sure acne treatment becomes less of a ‘hit and miss’ affair and follows a logical pathway.
Emphasis is placed on the importance of providing treatment of suitable duration, monitoring response and changing treatment if necessary. In addition, it provides the option for maintenance treatment where appropriate.
NHS England has advised that prescriptions for treating mild acne should not routinely be offered in primary care as the condition is appropriate for self-care.1 Pharmacists can help to support and guide patients with general measures and in the effective use of OTC and prescribed medication.
Acne (acne vulgaris), which affects up to 95 per cent of people aged 12-24 years, is characterised by inflammation of the pilosebaceous units and lesions, mainly on the face, back and chest. Typical lesions include open comedones (blackheads) and closed comedones (whiteheads), inflammatory papules, pustules, nodules and cysts.
Untreated acne can lead to scarring – often atrophic, so-called ‘ice-pick’ scars – and hyperpigmentation, especially on dark skin. Although acne usually resolves after a few years, it can have a serious impact on quality of life at a critical time in a person’s development. The severity of acne can vary considerably.
First-line treatment options
First-line treatment should be selected from the options in Table 1 according to the severity of acne and individual preferences. Whichever treatment is chosen, a 12-week course should be prescribed.
Benzoyl peroxide monotherapy should only be considered if the combination treatments in the table are contraindicated or if the patient wishes to avoid using a topical retinoid, or a topical or oral antibiotic.
The use of antibiotic treatments is associated with a risk of antimicrobial resistance – so topical or oral antibiotic preparations should not be prescribed for longer than six months, while the following should not be used at all:
- Monotherapy with a topical antibiotic
- Monotherapy with an oral antibiotic
- A combination of a topical and oral antibiotic.
First-line treatment should be reviewed after 12 weeks to assess whether the acne has improved and if there are any side-effects. In people whose treatment includes an oral antibiotic, if their acne has completely cleared prescribers should consider stopping it but continuing the topical treatment. If the acne has not cleared completely, the treatment may be continued for up to 12 more weeks. If acne fails to respond to the selected treatment, a different combination may be tried.
People who experience incomplete clearance or frequent relapses may be offered maintenance treatment initially with a fixed combination of adapalene and benzoyl peroxide. This should be reviewed after 12 weeks to decide whether it should continue.
Action points
- Give people with acne clear information tailored to their needs. This includes explaining the different treatment options and the importance of adherence for a minimum of six to eight weeks to see the effects of treatment
- Provide skincare advice including guidance on washing with a mild detergent, using oil-free moisturisers and sun creams, and avoiding picking or scratching as this can increase the risk of scarring
- There is insufficient evidence to identify dietary factors that might be implicated in acne, so normal, healthy eating should be recommended
- To reduce the risk of skin irritation (red, sore, dry skin) associated with topical treatments such as benzoyl peroxide or retinoids, start with alternate-day or short-contact application (e.g. washing off after an hour). If tolerated, progress to using a standard application
- Be aware that topical retinoids and oral tetracyclines are contraindicated during pregnancy and when planning a pregnancy. Explain to women of childbearing potential that they will need to use effective contraception. Women who become pregnant while using a topical retinoid can be reassured that the foetus is unlikely to be harmed, according to a systematic review and meta-analysis that examined pregnancy outcomes following first trimester exposure to topical retinoids2
- Don’t forget that some drug treatments can cause acne and/or might be aggravating a patient’s acne. These include topical and oral corticosteroids, anabolic steroids, lithium, ciclosporin and iodides taken orally (which may be part of some homeopathic therapies)3
- Patients with severe acne, high risk of scarring or severe mental health problems (e.g. severe depression, suicidal ideation) should be referred for (or advised to seek) specialist treatment
- Oral retinoid treatment should only be used after adequate courses of standard therapy with systemic antibiotics and topical therapy have been tried. Oral retinoids are highly teratogenic and are only prescribed for women of childbearing potential in conjunction with a rigorous pregnancy prevention programme.4
References
- NHS England. Conditions for which over-the-counter items should not routinely be prescribed in primary care: Guidance for CCGs
- Kaplan YC et al. Pregnancy outcomes following first-trimester exposure to topical retinoids: a systematic review and meta-analysis. Br J Dermatol 2015; 173: 1132-1141. doi.org/10.1111/bjd.14053
- Primary Care Dermatology Society. Acne vulgaris guideline
- European Medicines Agency. Updated measures for pregnancy prevention during retinoid use. March 2018 EMA/165360/2018.