Ticked off
In Clinical
Follow this topic
Bookmark
Record learning outcomes
How can pharmacists help to tame ‘one of the most dangerous animals in Europe’?
Key facts
- Tick-borne diseases are on the rise in the UK
- Ticks contribute to drug sensitivities and food allergies
- During 2017, there were 1,579 laboratory confirmed reports of Lyme disease in England and Wales
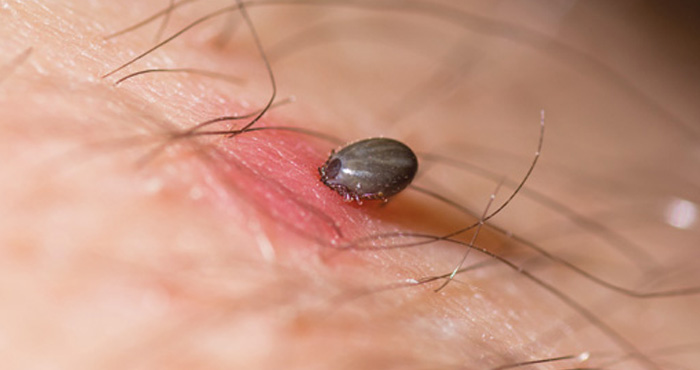
As my mug of tea cooled, I watched the tiny spider-like tick, which hitched a lift during a walk in the woods, crawl over my wrist. Thankfully, it hadn’t yet stuck its barded proboscis through my flesh to gorge itself to 100 times its body weight on my blood. I squashed the tiny vampire before it had the chance to potentially make me one of the thousands of people who develop tick-borne diseases in the UK each year. Indeed, some experts regard the tick Ixodes ricinus, which is common across the UK, as “one of the most dangerous animals in Europe”.1
Meanwhile, ecological changes are driving a rise in tick numbers and there are the first signs that once exotic infections are becoming endemic. More surprisingly, some ticks increase the likelihood of drug-related hypersensitivity, explain mysterious anaphylaxes and force immunologists to rethink some basic ideas about allergies. So, this feature looks at how pharmacists can help patients and pets prevent this growing threat to human and animal health.
Introducing ticks
The Acari, the group of parasites that includes mites and ticks, first emerged some 400 million years ago.2 Most mites are less than 1mm long.3 Some are tiny: Demodex folliculorum and D. brevis live in human hair follicles and sebaceous glands respectively.4 Ticks are larger: a female cattle mite engorged on blood can reach 3cm long.3
Broadly, there are two families of tick. As their name suggests, the approximately 700 species of hard ticks (Ixodidae) are covered by a shield called a scutum. The 200 or so species of soft ticks (Argasidae) don’t have a scutum. Another family (Nuttalliellidae) has a single member.3,5
The location of the mouth parts differs between hard and soft ticks, but both families, unlike mites, have a harpoon-like hypostome, with teeth that curve backwards. The teeth pierce the skin allowing hard ticks to feed for several days or weeks and make them notoriously difficult to dislodge.3,5 During this time, hard ticks drink more than 100 times their body weight in blood, secreting 60-70 per cent of the water back into the host. Soft ticks, in contrast, can gorge themselves in minutes to hours.5
Twenty tick species are native to the UK. The sheep, deer or castor bean tick (I. ricinus), for instance, is the vector for the spiral-shaped bacterium (spirochete) Borrelia burgdorferi that causes Lyme disease. During 2017, there were 1,579 laboratory confirmed reports of Lyme disease in England and Wales. However, Lyme disease is not notifiable by medics so this is probably an under-estimate. The true figure is probably closer to 3,000 cases in England and Wales each year.6,7
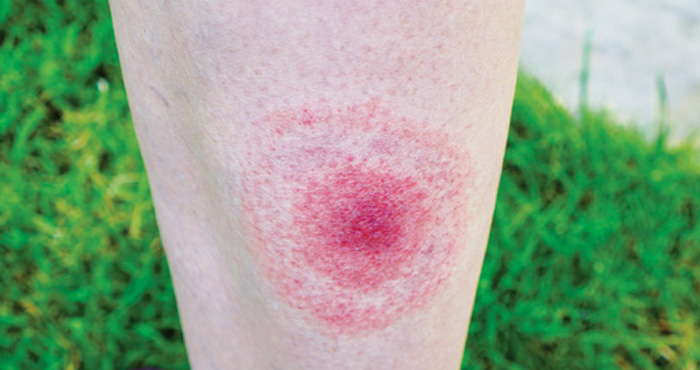
Lyme disease, which is especially common in southern England and the Scottish Highlands, causes a characteristic circular red rash and flu-like symptoms.7 Pharmacists should refer suspected cases urgently. Patients usually recover with two to four weeks of antibiotics but, if not treated quickly, Lyme disease can cause serious neurological and cardiac complications.7
In Europe, up to 3 per cent of immature nymphs and up to 5 per cent of adult ticks carry the tick-borne encephalitis virus (TBEV),1 which is endemic in 27 European countries, including Austria, southern Germany, the Baltic states, Switzerland, Belgium and the Netherlands.1,7,8
If not treated quickly, Lyme disease can cause serious neurological and cardiac complications
Ticks, drug sensitivities and food allergies
Perhaps more surprisingly, ticks contribute to drug sensitivities and food allergies. About 1-2 per cent of patients in clinical studies of cetuximab (a monoclonal antibody that treats some colorectal, and head and neck cancers) developed hypersensitivity reactions, some of which were severe. All the patients who developed a hypersensitivity reaction were already sensitive to a sugar called galactose-alpha-1,3-galactose (alpha-gal).9
Aside from humans and other primates, most mammals express alpha-gal in their cell membranes – which is why transplanting organs from animals to humans is difficult because the immune system reacts against alpha-gal.9 The genetically engineered mouse cells that produce cetuximab add alpha-gal residues to the protein backbone during post-transcriptional modification.9,10 But why were people already sensitive?
When American researchers mapped hypersensitivity reactions, they clustered in Arkansas, North Carolina and Tennessee, but not in either northern California or Boston. Meanwhile, patients stated presenting with allergic reactions – including generalised urticaria, angioedema and anaphylaxis – to mammalian meat and products such as dairy, wool and gelatine.9,10 When researchers asked, 94.6 per cent of those with a meat allergy recalled a tick bite. The rest said they spent a lot of time outdoors.9
The distribution of Rocky Mountain spotted fever almost exactly overlapped with the clusters of cetuximab reactions and the red meat allergies.9,10 The Lone Star tick (Amblyomma americanum), which is common across the south-eastern US, transmits the bacteria that causes Rocky Mountain spotted fever.9 It seems the Lone Star tick sensitises people to alpha-gal, perhaps from the remnants of a previous meal or an unidentified chemical in the saliva.9 Indeed, almost one in five of the general Tennessean population were alpha-gal sensitive.9
Usually proteins trigger allergic reactions, which are characterised by increased levels of immunoglobulin E (IgE), but people with meat allergies show raised IgE to alpha-gal. This tick-borne sensitivity is leading immunologists to rethink some basic ideas about allergies.9
A tick-borne allergy in Tennessee might not seem relevant in Telford but, in 2007, researchers reported meat allergy in people sensitised to alpha-gal by the Australian paralysis tick (Ixodes holocyclus). Since then, researchers have reported alpha-gal allergy associated with ticks from South America, Africa, Asia and Europe including the UK.9
No-one knows how many people have alpha-gal allergy: one American study found that the reaction might account for 9 per cent of otherwise unexplained anaphylaxes.9 All this matters because heparin, pancreatic enzymes, thyroid supplements, some vaccines, intravenous fluids containing gelatine and the filler magnesium stearate all contain alpha-gal.9

Ticks and pets
Pharmacies offering animal health services need to watch out for ticks. Increasingly, owners walk dogs in the countryside, which raises the risk of tick-borne diseases that were traditionally unusual outside of rural communities. In the UK, I. ricinus can, for example, transmit the louping-ill virus and the bacterium Anaplasma phagocytophilum, which causes tick-borne fever.11 Pharmacy teams should therefore reinforce the importance of checking for ticks as part of routine pet care, regardless of whether their location is rural or urban.8
Louping-ill virus, which causes similar neurological problems to TBEV, is common among red grouse, sheep and other ruminants, but may infect people and dogs.11,12 The public health risk posed by louping-ill virus is unclear.12 A. phagocytophilum is also common in ruminants and can infect dogs and cats. While often asymptomatic, A. phagocytophilum can cause immuno-suppression, which can exacerbate or contribute to other diseases.11 It is important to refer to a vet if there is any doubt about an animal’s health.
Hard ticks can transmit other parasites, such as the protozoa Babesia canis; a potentially fatal infection in dogs, which is common across mainland Europe. The mite vector (Dermacentor reticulatus) is endemic in several parts of the UK but until recently, vets thought the UK was free from endemic B. canis, although some cases arrived by pet travel and imports. In 2015 and 2016, however, several untravelled dogs in Essex developed babesiosis and researchers collected the tick from fields in which the dogs walked.13 It seems canine babesiosis now has a foothold in the UK.
Growing problem
Ecological changes could encourage further outbreaks of tick-borne diseases. Crimean-Congo haemorrhagic fever virus (CCHFV), for instance, kills 10-40 per cent of infected patients. Since being found in Crimea in 1944 and in the Congo in 1969, thousands of people worldwide have contracted CCHFV from the bite of Hyalomma marginatum, dead infected ticks, contaminated human blood and other body fluids, and animal tissues. Migratory birds dispersing H. marginatum seem responsible for CCHFV outbreaks in Turkey.14
The Parliamentary Office of Science and Technology (POST) suggests that CCHFV currently poses “a low risk to the UK”.7 Each spring migrating birds carry H. marginatum into the UK but, currently, our climate is too cold for the tick to survive.12 Climate change may mean the ticks become established. Moreover, several ticks (including species of Ixodes) can transmit CCHFV.14 In one case, a tick on a dog from Portugal had the potential to carry CCHFV,8 so in certain circumstances the endemic areas could expand rapidly.14
Tick-borne diseases that were once viewed as exotic (as we saw with B. canis) can get a foothold in the UK. In 2005, Public Health England launched the Tick Surveillance Scheme (TSS) and by 2018 this had identified 339 different ticks belonging to 10 species arriving from 15 countries, most of which entered on dogs.7,8 Not all imported ticks were submitted to the TSS so this is certainly an underestimate.8 One submitted tick – Rhipicephalus sanguineus – can transmit canine babesiosis, ehrlichiosis (caused by species of the Ehrlichia bacteria) and the human infection Mediterranean spotted fever, caused by the bacterium Rickettsia conorii.8
Climate change may allow invasive non-native ticks to establish populations in the UK7 and allow native ticks to expand their range: I. ricinus seems to be increasing its distribution across Europe, for instance.12 One estimate suggested that a 2ºC rise in annual average temperature could increase the number of Lyme disease cases in the US by more than 20 per cent in the next few decades.6
Changes to land use also influence tick distribution. Tick populations are highest in wooded areas and where there are high numbers of deer, sheep and other hosts.7 Increasing deer populations, their expanding territories, which now include towns and cities, green-belt developments, urban greenspace and wildlife corridors, are driving the spread of ticks in lowland UK. And the TSS reports increasing tick numbers in urban areas.12
Climate change may allow invasive non-native ticks to establish populations in the UK
Advising the public
Warmer climate also changes our behaviour. We are more likely to spend time outdoors wearing less clothing, leaving us vulnerable to tick bites.12 Fortunately some simple tips can help to reduce the risk. People visiting high-risk areas in the UK or abroad should be advised to wear light-coloured protective clothing, such as long-sleeved shirts and long trousers tucked into boots or socks. As far as possible, advise them to avoid brushing against vegetation that may harbour the tick, so staying in the middle of a paths.1
After returning, pharmacists should suggest walkers take a shower and look for ticks, especially on the backs of knees, armpits and groin. Removing a tick quickly minimises the risk of infection.1 A tick probably needs to feed for at least 24-48 hours before transmitting a pathogen.8 Pharmacists should suggest people grasp the tick as close as possible to the skin, ideally using fine-tipped tweezers or forceps. Gently twist to loosen the tick and pull out slowly. Any remaining parts will fall out as the skin sheds.1
Secondary infections are rare in healthy people, but they should wash the area with soap and water and, if they want to be on the safe side, apply an antiseptic. Put the tick into folded paper (to reduce the risk of infection) and crush or kill with boiling water. Washing or drying clothing at 60°C for 20 minutes should also kill any ticks.1
Many mosquito repellents sold in pharmacies – especially those containing N,N-Diethyl-m-toluamide (DEET), picaridin or ethyl butylacetylaminopropionate (EBAAP) – also protect against ticks, but it is worth mentioning to customers that these protect for a shorter time against mites than for mosquitoes.1
The emergence of new endemic diseases, the link with allergies, as well as climate and other ecological changes mean that the impact and clinical importance of tick-borne infections will almost certainly grow in the UK over the next few years.
Further information
- Babesia canis information
- Bristol University Tick ID
- Centers for Disease Control and Prevention
- European Centre for Disease Prevention and Control
- National Biodiversity Network Atlas (search for ticks for UK reports)
- Lyme Disease Action
- Lyme disease information
- Public Health England’s Tick awareness and the TSS.
References
- British Journal of General Practice 2016; 66:492-494
- Available here
- Matthews BE. An Introduction to Parasitology. Cambridge University Press. 1998
- Proceedings of the National Academy of Sciences 2015; 112:15958-15963
- PloS One 2011; 6:e23675-e23675
- Canadian Journal of Infectious Diseases and Medical Microbiology 2018; 2018:10
- Available here
- Veterinary Record 2018; 182:511-513
- The Biologist 2018; 66:18-21
- Journal of Allergy and Clinical Immunology 2015; 135:589-596
- Veterinary Record 2018; 182:609-609
- The Lancet Infectious Diseases 2015;1 5:721-730
- Parasites & Vectors 2018; 11:132
- Viruses 2019; 11:529; DOI: 10.3390/v11060529
