Eye problems and their management
In Clinical
Follow this topic
Bookmark
Record learning outcomes
Routine eye examinations were suspended during the Covid-19 lockdown. With high street opticians now struggling with a backlog of cancelled appointments, pharmacy’s role in the detection and management of common eye conditions has never been more essential
Learning objectives
After reading this feature you should be able to:
• Describe why Covid-19 protection measures could lead to preventable loss of sight in some people
• Understand how pharmacists can diagnose and manage various common eye problems with OTC treatment options
• Look out for warning signs that might indicate more serious eye disease.
With the pandemic continuing to affect the way eye care services are provided, the College of Optometrists is forthright in its assessment of the situation: “The current measures in place to protect people from acquiring Covid-19 will undoubtedly lead to vision loss that in normal circumstances would have been preventable as additional safety measures will further reduce capacity.”1
Community pharmacy teams can help both in the identification of warning signs indicating potentially serious underlying eye conditions, as well as in the everyday management of common eye ailments.
Macular degeneration
Age-related macular degeneration (AMD) is a serious eye condition that currently ranks among the leading causes of sight loss in the over-50s.2 With dry AMD, which accounts for 90 per cent of cases, symptoms develop slowly and insidiously, often going undetected for years. In contrast, wet AMD usually has a sudden onset with significant changes to the central vision occurring over days or weeks.
The macula is the middle part of the retina responsible for visual acuity, so degeneration manifests as a blurred area in the central line of vision which grows bigger over time, causing objects to appear dimmer and out of focus. Key signs of potential AMD that pharmacy staff should be vigilant for include difficulty reading small print despite reading glasses, a blurred area in the centre of the visual field and straight lines appearing distorted or wavy.
Currently there is no treatment for AMD but OTC supplements available specifically for the condition contain high doses of vitamins A, C, E, the minerals zinc and copper, and the micronutrient lutein, which may slow disease progression. Regular eye examinations, smoking cessation, exercise and a healthy diet are also important parts of early AMD management.
For wet AMD, treatment options include injections of antivascular endothelial growth factor (anti-VEGF), photodynamic therapy and photocoagulation therapy.

Key facts
• Measures to protect against Covid-19 could actually lead to preventable vision loss
• Studies are looking at a potential link between eye disease and Covid-19
• Pharmacy teams have a vital role in managing common eye conditions
• Age-related macular degeneration is the leading cause of sight loss in the over-50s
• Old age is a key risk factor for glaucoma
Diabetic retinopathy
There are several different variants of diabetic retinopathy, all of which stem from glucose- induced damage to the network of small vessels that supply blood to the retina. The most important advice for any customer with diabetes is to keep blood glucose levels well controlled.
Good glycaemic control is key to safeguarding eye health, as well as preventing development of a host of other serious disease-related complications. Blood pressure and cholesterol should also be kept in tight check, along with regular exercise, maintenance of a healthy weight and smoking cessation. Attending annual retinal screening appointments is vitally important as early detection and treatment of retinopathy can help prevent sight loss.
Any customer with type 1 or type 2 diabetes can potentially develop retinopathy but pharmacy teams should also be aware of key risk factors, which include long-standing diabetes, persistent hyperglycaemia, high blood pressure or cholesterol, or being of Asian or Afro-Caribbean descent.
Symptoms are not usually noticeable until retinopathy is in the advanced stages but when they do develop can include a gradual worsening of vision, sudden sight loss, floaters, blurred/ patchy vision and eye pain or redness. Any diabetic customer presenting with these symptoms should be encouraged to visit an optician.
Diabetic retinopathy that is threatening or already affecting a patient’s vision can be treated with laser therapy or injection of anti-VEGF agents directly into the eye. In advanced cases, surgical intervention may be carried out to remove blood or scar tissue from the eye.
Dry eye
Dry eye results from an imbalance in the triple-layered tear film that bathes and lubricates the eye. Potential signs and symptoms include dryness, the sensation of a foreign body in the eye, burning, itching, grittiness, sensitivity to light, frequent blinking, redness and – somewhat paradoxically – excessive eye watering as the tear glands attempt to overcome dryness by producing large volumes of tears.
Artificial tears are the cornerstone of dry eye treatment and work by lubricating the eyes and boosting moisture levels.
A number of different products are available OTC, of which hypromellose is the most frequently used preparation. Drops may need to be instilled hourly until symptoms improve, after which frequency can be tapered off.
Other treatment options include:
- Hyaluronic acid-based drops, which combat tear deficiency
- Carbomer gels, which cling to the eye surface
- Polyvinyl alcohol preparations, which improve ‘wetability’
- Ointments containing paraffin or wool fat.
NICE specifically recommends preservative-free formulations for customers with known sensitivity to tear supplements, more severe dry eyes that require drops more than four times per day, those using multiple preserved topical medications or wearers of soft or hybrid contact lenses.3
It is also important to be aware of common culprit medications that can cause dry eye such as diuretics, beta blockers, antihistamines, sleeping drugs and some analgesics. Other potential environmental triggers include wearing contact lenses, central heating, air conditioning, smoky environments and excessive screen time.

Conjunctivitis
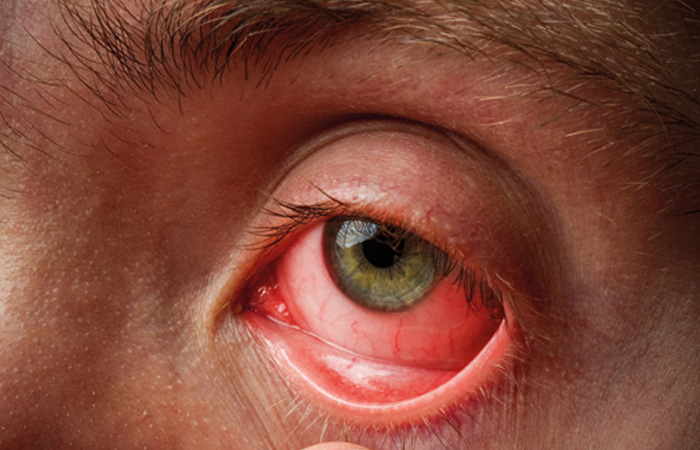
Conjunctivitis is one of the most common eye complaints encountered in pharmacy and describes inflammation of the thin membrane (the conjunctiva) that covers the whites of the eyes and inside of the eyelids. There are two key types of conjunctivitis: infective, which is highly contagious, and allergic, which is not.
Infective conjunctivitis causes the whites of the eyes to become pink and the eyelids red and swollen. It usually starts in one eye and quickly spreads to the other. A sticky discharge is produced that results in the eyelashes sticking together on waking and the eyes may feel gritty and irritated.
Allergic conjunctivitis, often associated with hay fever, also makes the eyes pink/reddish in colour but develops in both eyes at the same time and is typically accompanied by other symptoms such as sneezing and runny nose. Eyes may be watery and feel itchy.
Self-care measures can help ease both types of conjunctivitis. Customers should be advised to clean the eyelids with cotton wool soaked in sterile saline or cooled boiled water to remove any discharge.
A cool compress such as a cold flannel held against the eyes for a few minutes can also help ease discomfort, and lubricating drops or artificial tears can be recommended. Contact lenses should not be worn during a bout of conjunctivitis. For cases of infective conjunctivitis, sufferers should be encouraged to wash hands regularly, avoid rubbing their eyes, and keep towels and flannels separate. Most cases of viral and bacterial conjunctivitis are self-limiting and will resolve within around seven days without treatment.3 Customers should therefore be encouraged to pursue self-care steps in the first instance but if the problem is severe or circumstances require rapid resolution, then a topical antibiotic can be recommended.3
Options include chloramphenicol 0.5 per cent drops, 1 per cent ointment or fusidic acid 1 per cent drops.3 Eye drops containing sodium cromoglicate or antihistamine as active ingredients are the recommended treatments for allergic conjunctivitis. Any treatment for conjunctivitis in a child under two years will require a prescription from a GP.
Glaucoma
There are several different types of glaucoma but all result in increased fluid pressure within the eye, which damages the optic nerve. Regular routine eye examinations are key to detecting glaucoma as the condition typically develops very slowly over many years without obvious symptoms, leading to it being christened ‘the silent thief of sight’.
Pharmacy teams should be aware that advanced age (over 70 years) is a key risk factor for glaucoma development. The condition is also more common in people with a family history of glaucoma, of African, Caribbean or Asian origin, with short/ long-sightedness or suffering from diabetes. When they do occur, possible symptoms of glaucoma include changes to peripheral vision, blurred vision or seeing rainbow-coloured rings around bright lights.
The first step in treatment is eye drops to lower pressure in the eye. For most patients, this is all the treatment that is required, but it must be continued long-term – usually for life. For cases that do not respond to drops alone, other treatment options include laser therapy to unblock drainage tubes in the eye or reduce fluid production, and surgery (trabeculectomy) to boost the drainage of fluid out of the eye.
Uveitis
Uveitis is associated with inflammation in the middle part of the eye, known as the uvea, which includes the iris. It can cause pain, sensitivity to bright lights and vision impairment. Uveitis is relatively rare, affecting only around two to five people per 10,000 every year in the UK, and can be triggered by an underlying autoimmune condition, an infection or injury to the eye.4
Anterior uveitis is the most common type of uveitis and usually affects only one eye. It typically onsets quickly and is associated with aching eye pain where the eyeball feels tender, eye redness and photophobia. Prompt treatment of uveitis is important to reduce the risk of potential complications such as glaucoma and cataracts. Steroids are the mainstay of treatment, instilled as drops if the front of the eye is affected or as injections or oral therapy if the middle or back of the eye is inflamed.
Eye strain
Eye strain arises when the eyes become tired from prolonged activities such as reading, driving or – by far the most common culprit – computer use. Symptoms include blurred or double vision, sore/itching eyes, watering eyes, increased light sensitivity and headaches.
Such is the impact of technology that computer vision syndrome (CVS) has now been recognised as a specific collection of eye and vision problems stemming directly from computer use. Screens require the eyes to subtly but continuously refocus and also blunt the natural blinking reflex, both of which increase the risk of eye strain. The College of Optometrists recommends three key tips to help alleviate eye strain:5
- Follow the 20/20/20 rule – take a break every 20 minutes and focus on something 20 feet away for 20 seconds. Looking into the distance relaxes the focusing muscle, helping to reduce fatigue
- Make a conscious effort to blink regularly
- Wear glasses if they have been prescribed for you.

Eye floaters
Floaters appear as small black or translucent spots or strands that look like something ‘floating’ across the field of vision. Customers may also describe them as squiggly lines, rings or cobwebs. They are most obvious when looking at a bright background and may appear fleetingly before moving out of sight. Floaters are generally harmless, particularly
if they are long-standing, unchanging and not associated with any vision changes. However, on rare occasions, floaters can be harbingers of a more serious eye condition such as retinal detachment. A sudden appearance or increase in the number of floaters, eye pain, blurred vision or a dark ‘curtain’ or shadow moving across the visual field are all red flag signs that require immediate medical advice.
Floaters themselves are tiny pieces of debris in the vitreous humour that cast shadows onto the retina. They are most common among older people and usually result from the benign process of posterior vitreous detachment where the eye’s natural ‘jelly’ becomes more watery. There is no treatment for eye floaters but their presence is generally recorded and monitored during routine eye examinations.
Cataracts
Cataracts result from an age-related change which causes cloudy patches to develop on the lens of the eye. Symptoms include misty/cloudy vision, increased sensitivity to light and objects appearing ‘washed out’. Many people describe the vision through cataracts as akin to having dirty spectacles that need cleaning.
There is no pharmacological therapy for cataracts and the only effective treatment involves eye surgery to replace the cloudy lens with an artificial lens made of plastic or silicone. The timing of cataracts surgery is dictated by the severity of the vision impairment and its impact on a person’s life.
Customers should be made aware that there is a one in 10 chance of developing a complication known as posterior capsule opacification (PCA) after cataract surgery, which causes vision to become cloudy again.4 In most cases, this is easily treatable with a quick and painless outpatient laser procedure.
For the many patients awaiting cataract surgery who have experienced delays due to the coronavirus pandemic, pharmacy staff can provide reassurance that postponement should not increase their risk of permanent sight loss or complications, or make the procedure less likely to succeed. The RNIB provides some useful tips for maximising vision while awaiting treatment for cataracts.
Study to investigate link between retinopathy and Covid-19
Eye research charity Fight for Sight and Diabetes UK are joining forces to investigate if people with diabetic retinopathy are at greater risk of developing complications from Covid-19.
Research being carried out at the University of Edinburgh will investigate whether people previously diagnosed with diabetic retinopathy experience worse Covid-19 outcomes. The study will determine whether this is because the virus can reach tissues outside the lungs (in this case the eye) due to damaged blood vessel walls.
If successful, the results of the study will allow researchers to propose new ways of predicting Covid-19 risk based on non-invasive imaging of the eye. This could assist doctors in identifying the people at greatest risk of complications at the time of diagnosis and plan their treatment pathways accordingly.
Dr Miguel Bernabeu, who is co-ordinating the study, says that, if the results support the hypothesis, “we will be in a position to design a prospective study to validate these findings and advance towards clinical adoption within one year”.
“There is never an easy time to have diabetes, but the Covid-19 pandemic is a particularly difficult time for people living with the condition,” says Anna Morris, assistant director of research at Diabetes UK. “That is why it is crucial that we identify who is at higher risk of more severe outcomes from infection.”

Are people with diabetic retinopathy at greater risk of developing complications of Covid-19?
REFERENCES
- The College of Optometrists. Ophthalmology and Optometry: our vision for safe and sustainable patient eye care services in England during and beyond Covid-19. August 2020
- Specsavers. Macular Degeneration
- NICE Clinical Knowledge Summaries (CKS)
- Royal National Institute of Blind People (RNIB). Eye conditions
- The College of Optometrists. College of Optometrists issues advice on lockdown eye care to mark 6/6. June 2020.
