Sun safety: Rays awareness
In Clinical
Follow this topic
Bookmark
Record learning outcomes
In theory the public should all know by now what steps to take when the sun comes out, but on warm sunny days the matter of sun protection often falls by the wayside €“ and melanoma skin cancer rates are increasing fast as a result. Pharmacy teams need to hammer home the sun safety message.

Learning objectives
After reading this feature you should be able to:
- Help customers get to know their skin type and risk of skin cancer
- Advise them on how to choose and apply a sunscreen in addition to using other sun protection measures
- Refer patients with skin changes that may indicate skin cancer.
Figures from Cancer Research UK show that today's melanoma skin cancer incidence rates in the UK are four times higher than they were in the 1970s, having increased by 45 per cent in the past decade alone. During this period, incidences in men have been higher than in women (56 and 35 per cent respectively). According to the charity, 86 per cent of malignant melanoma cases are preventable.1
Last year, as part of its annual Shunburn awareness campaign, the Teenage Cancer Trust claimed that more than two-thirds of young people aged 13-24 years routinely went without sun cream to achieve a deeper tan.2
With no shortage of sun protection products available, much of the problem appears to stem from a lack of awareness about the damage prolonged exposure to the sun can cause, says Clare O'Connor, sun care expert at Boots UK.
€People in the UK often don't think about applying sunscreen when going about their daily activities such as gardening, walking the dog or washing the car, underestimating both the strength of the UV and the amount of time they will be exposed,€ she says. €But UV damage is cumulative and as we live longer and holiday more often, our total exposure can be much higher than for previous generations.€
Experts freely admit that it can be tricky to strike a balance between the recommended advice and the practicalities of applying a sunscreen every time you nip outside €“ but they still insist there needs to be a step change in awareness in order to tackle the continuing increase in skin cancer cases in the UK.
Debunking some myths...
People are definitely more 'sun aware' these days, especially as more products such as make-up and moisturisers now include SPFs, says Dr Anjali Mahto, a consultant dermatologist and spokesperson for the British Skin Foundation. €However, there is still the concern that people think they only need sunscreen when on hot beach holidays abroad,€ she says. €Obviously we know that the UK sun can burn skin, too.€
It is hugely important for pharmacists to be armed with the correct information that can be easily conveyed to the public, she says, but the number one rule is to make sure people understand there is no such thing as a safe tan €“ and that the only safe way to achieve one is from a bottle. Other misconceptions include:
My skin just goes brown: Sun exposure prompts the body to produce increased levels of melanin in skin cells, which is essentially a defence mechanism against damaging UV rays
Sun exposure helps to build up a base tan: Any browning of the skin is evidence the body is trying to protect itself from sun exposure
I have darker skin, so never burn anyway: People with darker skin can still burn or they can have a genetic disposition to skin cancer
I need the sun for vitamin D: Many experts now point to diet or supplements as a safer means of topping up vitamin D levels arising from limited direct sun exposure on the skin
I don't need sun cream before/after the peak times: While it is advisable to stay out of the sun between 11am and 3pm, you are still absorbing UVA/UVB rays at other times
Sun cream isn't necessary on cloudy days: It is thought that clouds may only reduce UV rays by about 20 per cent
Sunscreens don't really work anyway: Research shows that people routinely underuse sun creams, reducing their effectiveness.
One size does not fit all
Most people assume that buying a sun cream is all about how much time you want to spend in the sun, but individual requirements make it important to select the right level of protection. €I'd really like to see pharmacists helping their customers understand both their particular skin type and the importance of choosing high protection and UVA protection,€ says Clare O'Connor.
As a general rule of thumb, the following applies:
Skin types 1 & 2 and children: should use a minimum SPF 30 in the UK (but preferably SPF 50+), and SPF 50+ in southern Europe and more exotic far-flung destinations
Skin types 3 & 4: should use a minimum of SPF 15 in the UK; SPF 30 in Southern Europe and SPF 50+ further afield
Skin types 5 & 6: should use SPF 15 or even SPF 30 in equatorial regions.
Role of UV rays
Ultraviolet irradiation penetrates the earth in two forms:
€¢ UVB is typically responsible for sunburn and is linked to both malignant melanoma and basal cell carcinoma risk. SPFs aim to block UVB rays and prevent the skin from burning.
€¢ UVA affects the elastin in the skin and leads to wrinkles, sun-induced skin ageing and, potentially, skin cancer. UVA can penetrate window glass and penetrates more deeply than UVB.
Wherever possible, customers should be looking for both UVB protection (denoted by an SPF) and UVA protection (usually indicated by the star rating system).
Current EU recommendations require sunscreen manufacturers to label their products with both SPF numbers and low to very high protection labels.3 The UVA protection for each sunscreen should be at least a third of the labelled SPF. This adherence is denoted by the letters UVA in a circle. For example, a three-star product will protect against 60 per cent of UVA in relation to UVB, while a five-star product will protect against more than 90 per cent of UVA in relation to UVB.
The latest sunscreens also aim to offer protection against a much wider range of wavelengths €“ covering visible light and infrared radiation, which have been linked to skin pigmentation and premature skin ageing, respectively.
Get it covered
To ensure optimal protection, sunscreen should be applied 15 to 30 minutes before going out in the sun €“ and then re-applied every two hours and straight after swimming and towel drying.
The average-sized adult should apply more than half a teaspoon of sunscreen (about 3ml) to each arm and the face/neck, and just over one teaspoon (6ml) to each leg, the front of the body and the back of the body.
According to Anjali Mahto, common parts of the body that get missed when applying sunscreen include:
Eyelids: The skin of the upper and lower eyelids is thin and fragile. The best defence is to wear sunglasses that offer adequate protection against UVA and UVB, and which cover as much skin as possible
Legs: The commonest anatomical site for melanoma in females
Ears: The ears are a high-risk area, particularly for non-melanoma skin cancers such as basal cell and squamous cell carcinoma
Heads: Men with reduced hair or thinning scalp hair are vulnerable to scalp cancer, but women should also ensure that sunscreen is applied adequately to the hairline
Lips: Often an overlooked site for non-melanoma skin cancer, a photo-protective lip block or lip balm should be used to block UV rays
Everywhere besides: the same principles apply to the tops of feet, side of face, hands and underarms.
Additional advice
€¢ Always keep babies and young children out of direct sunlight
€¢ Don't forget to protect the skin with clothing
€¢ Wear a hat that protects the face, neck and ears
€¢ Spend time in the shade at peak sunny times (between 11am and 3pm)
Treating sunburn
Customers should receive the following advice if sunburnt:
Act quickly and get out of the sun: Cover up the affected areas and stay in the shade until the sunburn has healed
Wear loose cotton clothing: Allow the skin to 'breathe' over any sunburnt areas
Take OTC pain relief: Painkillers can help relieve the pain and reduce inflammation caused by sunburn (e.g. ibuprofen)
Cool the skin: Apply a cool compress to the skin (e.g. a towel dampened with cool water for 15 minutes), or take a lukewarm bath or shower. Make sure the shower is running at a gentle flow, but if blisters are starting to develop, then a bath is preferable. Do not rub the skin with a towel, but gently pat it dry
Moisturise: Use an unperfumed cream or lotion to soothe the skin after bathing. Repeat applications may be needed for several weeks to reduce the appearance of peeling. Aloe vera or soy-containing gels or lotions can be soothing, with aloe vera also acting as an anti-inflammatory. However, creams or lotions that contain petroleum, benzocaine or lidocaine can trap heat in the skin or cause local irritation
Stay hydrated: Drink water (and limit alcohol) to offset any dehydration
Use a mild steroid cream: Applying hydrocortisone 0.5-1% cream for 48 hours may decrease pain, swelling and inflammation caused by sunburn and speed up the healing process. Avoid in small children
Leave blisters alone: Popping blisters can lead to infection and scarring. Blisters will settle by themselves after a few days.
Checking moles
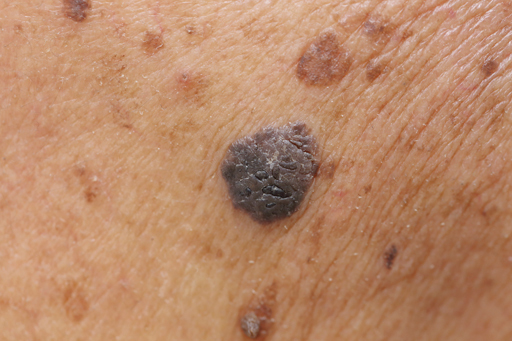
Dermatologists recommend people examine their skin on a monthly basis in order to detect unusual growths or changes.
According to Cancer Research UK, people with just one unusually shaped or very large mole (atypical naevi) have an increased risk of melanoma. The risk increases with the number of atypical naevi.4
Any self-check should be carried out in a well-lit room with the aid of a full-length mirror. It is important to look closely at the entire body including the scalp, buttocks and genitalia, palms and soles, including the spaces between the fingers and toes. Customers with lots of moles should ask someone else help them with their check.
The acronym 'ABCDE' is a useful guide to follow for warning signs:
Asymmetry: one half of the mole is different to the other
Border: an irregular, scalloped or poorly defined edge
Colour: uneven colour or variable colours within a mole
Diameter: the mole is bigger than 6mm in size
Evolving: the mole is changing in its size, shape or colour.
€When it comes to managing the risk of skin cancer, having a lot of moles can be significant €“ simply because it is more likely that one might change,€ says Dr Susan Mayou, consultant dermatologist at Cadogan Clinic, whose mole mapping service is the only one validated by the British Skin Foundation.
€What people are really looking for [could be described as] a member of the orchestra playing out of tune. If they have any specific concerns about a suspicious-looking mole, or one that has changed or is causing them discomfort, then they should visit their GP or a dermatologist without delay for a more thorough investigation.€
The clinic, she says, has seen a significant increase in the number of people visiting for mole checks. €I'd like to think it is a sign that more people are coming to realise that their skin needs to be monitored just like any other part of the body and are adding a mole check to their calendar. I would love to see people doing this, because skin cancer is highly curable if caught in its early stages. Although the skin is the body's biggest organ, it is easy to have it checked €“ and any worries can be ticked off in 10 or 15 minutes.
€It would be enormously valuable if community pharmacists could carry promotional material about moles on the counter and more easily direct customers to read it €“ bundling it with sun cream purchases, for example. Simply raising the topic on a sunny day could really help make a difference.€
References
1. cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/skin-cancer#heading-Zero
2. teenagecancertrust.org/about-us/news/nearly-23-teens-shun-sunscreen-deeper-tan
3. bad.org.uk/for-the-public/skin-cancer/sunscreen-fact-sheet#spf-in-moisturisers
4. cancerresearchuk.org/about-cancer/melanoma/risks-causes
