Clinical

Sight for sore eyes
In Clinical
Let’s get clinical. Follow the links below to find out more about the latest clinical insight in community pharmacy.Bookmark
Record learning outcomes
A recent news story about a child who lost their sight due to poor nutrition has raised awareness of how fragile eyesight can be. Experts are also concerned about the effects excessive screen time can have on the eyes… but what do they mean by excessive?

Learning objectives
After reading this feature you should be able to:
- Discuss the impact screen habits can have on the eyes
- Understand the role regular eye tests can play in detecting illness
- Provide guidance on the treatment of common eye conditions.
According to the latest Sounds Insight report 2019 from Scrivens Opticians, the number of teenagers aged 13 to 16 years needing glasses has risen from 20 to 35 per cent over the past seven years – and “too much” screen time could be to blame, the authors believe.
Of the 13 to 16-year-olds requiring glasses, 66 per cent are short-sighted. Typically this age group spends 26 hours a week looking at their mobile phones and/or tablets, watching TV and playing video games. The research found that half of parents have attempted to curb their teenager’s screen time amid fears that too much has a negative impact on their child’s eyes.
There is no real consensus among eye experts about whether screen time has a direct impact on children’s vision in the long-term, but looking at screens for prolonged periods of time (as well as reading or any close work) can lead to short-term eye strain.
“Most experts agree that children can have similar symptoms from excessive screen time as adults, such as dry eyes, and blurry and tired vision,” says Max Halford, clinical lead for the Association of British Dispensing Opticians.
“There is some really interesting research around the huge increase in myopia (short-sightedness) linked to excessive time spent looking at a screen, possibly linked to lack of time spent outdoors and exposure to UV. With regard to screen time, most agree that toddlers aged two to five years should not exceed one hour per day and above this age screen time should not exceed two hours per day.”
Testing times
This year’s National Eye Health Week (September 23-26) promoted the need for regular eye tests at all ages. Adults and children should have eye tests every two years (unless advised otherwise by an optometrist). Eye tests for children can pick up squint, amblyopia (lazy eye), long-sightedness and short-sightedness, as well as other issues such as colour blindness.
In the Scrivens report, 26 per cent of the parents said they had never taken their children for an eye test, even though they are free on the NHS for children under 16 years of age or those under 19 years in full-time education. “Parents always have a long back-to-school check list, but getting children’s eyes tested should be a priority,” says Scrivens.
“Many children don’t understand what is ‘normal’ when it comes to their vision, so probably won’t know if they are having problems. An eye test will reveal any issues that in most cases can be corrected through prescription glasses or contact lenses. Not only will seeing clearly make reading and writing easier but it will help levels of concentration so children can remember what is being taught in class. Being able to detect any issues with sight at this crucial stage of development and education can help to ensure a child doesn’t fall behind.”
Pharmacy teams are ideally placed to promote the importance of regular eye tests for children when parents come in for health advice. Signs that an older child may need an eye test include headaches or eye pain, dry eyes, rubbing the eyes excessively, sitting too close to the television, squinting, tilting their head or covering one eye.
Younger children may show clumsiness, poor hand-to-eye co-ordination or bump into things, says Poonam Patel, eye health information officer at the Royal National Institute of Blind People (RNIB). “Pharmacies should build links with local optician practices so that staff can provide customers with information on where they can go for an eye examination,” she says.
Early diagnosis crucial
It is not just children who are missing out on eye tests – many adults also don’t visit an optometrist regularly. “We know from many studies that people value their eyesight,” says Cathy Yelf of the Macular Society, “so it is a paradox that people take so little care of their eyesight and often don’t know how to care for their eyes.”
“Many people only have a sight test if they notice obvious changes to their vision. They may not realise that an eye examination can detect the early signs of conditions that are potentially sight-threatening, such as glaucoma or age-related macular degeneration. Eye examinations can also reveal other health conditions such as diabetes, high blood pressure or cancers.”
If a customer complains of regular headaches or has recently had a fall, the pharmacy team could ask them when they last had a sight test. Some adults may not have regular eye tests because they worry about the cost. Yet free eye examinations are available on the NHS for certain groups (e.g. the over-60s and people with diabetes or glaucoma). Some people may qualify for an optical voucher, which can be used as full or partial payment towards the cost of glasses or contact lenses of their choice. If customers are housebound, they may be entitled to a NHS-funded sight test at home (domiciliary sight test).
Many chronic eye conditions, such as age-related macular degeneration (AMD), glaucoma and cataracts, don’t cause symptoms in the early stages, but changes in the eye can be picked up during a routine examination. If a customer has early AMD, an eye examination may show pigment changes in the retina and/or the presence of large ‘drusen’ (yellowish, fatty deposits). Pharmacy customers who mention any changes to their vision should be referred to an optometrist straightaway.

“Customers who describe any sudden changes in vision, such as blurriness or distortion, or vision loss, could be showing signs of AMD or glaucoma,” says Meena Ralhan, optical compliance manager at Vision Express. “AMD would cause distortion to straight lines making them appear wavy. Glaucoma is a more gradual visual loss and patients may say they can’t see the periphery well, known as tunnel vision. Advice must be to see
an optometrist as soon as possible for investigation.”
According to the International Glaucoma Association, glaucoma (raised intraocular pressure) affects 2 per cent of people over 40 years, with around half of all cases remaining undiagnosed. The commonest type, primary open angle glaucoma, tends to develop slowly over several years with no early warning symptoms.
Acute closed angle glaucoma, which is much less common, is a medical emergency. “This can present with sudden onset red and very painful eye, with blurred vision and a cloudy cornea,” says Poonam Patel. “These symptoms should always be referred to the nearest A&E or eye casualty service so that the patient receives prompt treatment to reduce eye pressure quickly and prevent permanent damage to sight.”
The International Glaucoma Association and UK Opthalmology Alliance recently produced a Patient Standards for Glaucoma document. Recommendations include ensuring that patients are able to self-administer their glaucoma medication – for example, patients with arthritis of the fingers may have physical problems applying eye drops, so may need compliance aids or other treatment strategies such as laser or surgery.
“Pharmacy staff can support patients with glaucoma by educating them on the importance of administering their eye drops correctly and advising them of compliance aids if they are having difficulties,” says Poonam Patel. “Compliance to treatment is very important in the management of glaucoma and in preventing sight loss.”
Joining the dots...
Don’t place medicine labels over on-pack Braille, David Clarke, services director at the Royal National Institute of Blind People, tells pharmacists
As a blind person with congenital glaucoma I have benefited hugely from numerous innovations during my lifetime that have enabled me to live independently.
One such example is the innovations contained within smartphones which, through the power of synthetic speech, enable me to buy goods, participate in social media, navigate, do my banking and find out which platform my train is leaving from.
One of the most important changes I have noticed is the introduction of Braille labels on medication packaging. For some time now it has been a legal requirement under European law for pharmaceutical companies to display the name and strength of medicines in Braille on their packaging. What does this mean for someone like myself? If the labelling is undertaken correctly, I can discern from the packaging the name of the product I have picked up, its strength and how I can safely use it. This is great – but further improvements could be made.
There for a reason
Notwithstanding the difference that this innovation has made to the daily lives of the over 20,000 Braille readers in the UK, it is still possible for the process to be unintentionally sabotaged. This is where anyone working in a pharmacy or in a pharmaceutical packaging operation can help.
I recently had cause to pick up a prescription from a pharmacy in the north west of England on behalf of my mother. On presenting myself at the counter along with the correct credentials, the package was placed in a paper bag and handed over to me – a very efficient process. But in this case there was one major failing.
The sticker denoting who the prescription was for had been placed over the Braille instructions, thereby rendering it useless. This is, of course, just one example of where the process can be interrupted.
Anecdotally, the defacing of Braille instructions can occur at any point from when the packaging is produced right up until the product is picked up by the end user. So what can pharmacists do to ensure that the Braille can be read?
Keep in mind that the Braille included on packaging is there for a reason, backed up by law, and provides vital information to the people reading it. Never place labels over the top of the Braille and seek to ensure that the packaging is carefully handled to avoid unnecessary damage that will make the Braille more difficult or impossible to read.
And finally, a plea to manufacturers. Think carefully about what Braille text you are putting on your packaging. Is it essential information that is needed to use the product correctly and safely or does it merely reiterate the brand and the benefits? It is usually a small space – so please use it wisely!
The Braille included on packaging provides vital information to people reading it
Lifestyle habits
Many chronic eye conditions become more common with age or are related to family history. However, according to National Eye Health Week, 50 per cent of sight loss is avoidable and making certain lifestyle changes may help to prevent some chronic eye conditions. Smoking has been linked to a higher risk of cataracts and AMD, while heavy alcohol consumption has also been linked to AMD development. There is some evidence that regular exercise can help to preserve vision in older people, especially those with narrowing or hardening of the arteries, high blood pressure or diabetes.
“Lifestyle can have huge benefits for patients’ vision,” says Max Halford. “Smoking is often quoted as the highest modifiable risk for blindness and certainly in diabetes the annual retinal screening appointment is vital. A good diet, regular breaks from the screen and a routine eye test every two years – or more often if recommended by an optometrist – are the best ways of ensuring good long-term eye health.
“Eyes age like the rest of our bodies and UV damage early on in life can cause early cataracts, so a good pair of UV-protecting sunglasses will help. Dispensing opticians are there to advise on the most appropriate protective eye wear.”

Certain nutrients are particularly important for healthy eyes. According to information issued during this year’s National Eye Health Week, carotenoids may help to prevent AMD and cataracts, while deficiency in complex B vitamins may increase the risk of cataracts and retinopathy.
Omega-3 fatty acids may be beneficial for dry eyes and general eye health. Research shows that eating one portion of oily fish a week can help to lower the risk of developing AMD by up to 40 per cent. Maintaining a healthy weight is also essential for good eye health, as obesity is associated with a higher risk of diabetic eye problems and other eye conditions associated with stroke.
Poonam Patel says various dietary supplements on the market claim to be beneficial for eye health, but there is no good evidence that the general population should be taking them. “For people with AMD, it has been shown that a certain formula (AREDS2) of the antioxidant vitamins A, C, and E, as well as the trace element zinc and the micronutrients lutein and zeaxanthin, can help to slow down the progression of the condition in some people.
“An optometrist would be able to advise a patient with AMD whether nutritional supplements would be beneficial for them. Pharmacists and pharmacy staff can support these people by advising them of the particular formulations of nutritional supplements and products that have shown to be beneficial in large-scale trials.”
If pharmacy customers have an underlying chronic condition that can cause eye damage, such as diabetes, a healthy lifestyle is particularly important. According to Diabetes UK, 1,600 people lose their sight every year to diabetes (high blood glucose levels can damage the back of the eye, causing diabetic retinopathy). Annual screening is offered to everyone with diabetes aged 12 years and over to pick up and treat any problems early on.
Acute eye problems
Infective conjunctivitis
Conjunctivitis can cause red, bloodshot watery eyes, inflamed inner eyelids, blurred vision, a scratchy feeling and discharge. “Bacterial conjunctivitis often resolves in about a week without treatment,” says Poonam Patel. “Treatment with topical antibiotics may help to speed up resolution and render the patient less infectious to others. Viral conjunctivitis is also self-limiting, resolving within a couple of weeks. Cold compresses, artificial tears or lubricating ointments may help to relieve symptoms.”
Styes
A stye is caused by an infection of the eyelid glands. It causes a small, red, painful lump on an eyelid, usually on just one eye. The eye may look red and seem watery but vision won’t be affected. A stye is rarely serious and will usually get better on its own without any treatment. Holding a warm compress against the eye for five to 10 minutes at a time, three or four times a day, will encourage the stye to release pus and heal more quickly. Customers should avoid wearing contact lenses and eye makeup until the stye has healed. If the stye is very painful or swollen and isn’t getting better, customers should see their GP. Customers should never try to burst a stye themselves.
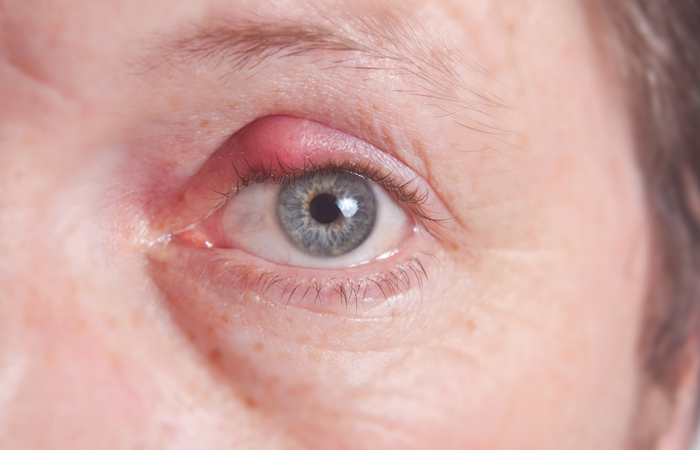
Blepharitis
Blepharitis (inflammation of the eyelids) can cause redness, crusty or greasy eyelashes and itchy/sore eyes. Good eye hygiene can prevent and manage the condition, and specific products are available over the counter. “Blepharitis can normally be treated by washing eyelids every day,” say Vision Direct’s in-house optometrists Brendan O’Brien and Benjamin Dumaine. “Lid cleaning often needs to be continued indefinitely to prevent recurrence. More severe cases of blepharitis may require treatment with antibiotic ointment applied to the eyelids or antibiotic drops used in the eyes and, in a few cases, steroid eye drops.”
Dry eyes
People with dry eyes either don’t produce enough tears or their tears evaporate too quickly. Their eyes may be itchy, inflamed and irritated. In severe cases, if left untreated, dry eyes can damage the cornea, leading to scarring. Dry eyes tend to affect the over-65s, menopausal women and those with certain chronic conditions, such as arthritis or diabetes. However, modern lifestyles are increasing symptom prevalence due to increased screen time, dusty environments, air conditioning and certain medications, says Meena Ralhan. “Pharmacies should recommend customers see an optometrist to determine the type of dry eye and ascertain the most effective course of treatment.”
Brendan O’Brien and Benjamin Dumaine recommend that mild to moderate cases of dry eye can usually be successfully treated using OTC artificial teardrops. “If a patient has severe symptoms and needs to use eye drops more than six times a day, or if they wear contact lenses, advise them to use preservative-free eye drops,” they suggest.
“Certain eye ointments can also be used to help lubricate the eyes, but can often cause blurred vision, so are probably best used only at night. More severe cases may require specialist medication or lacrimal punctal plugs.”
Charity stresses the need for a balanced diet
A YouGov poll for the eye research charity, Fight for Sight, has found that many people are unaware that certain unhealthy habits have possible links to sight loss.
The charity is raising awareness of the need to consume a balanced diet after research into the rare case of a child losing his sight through poor nutrition was published in Annals of Internal Medicine. The child’s diet, which resulted in serious vitamin deficiencies, led him to develop a condition called nutritional optic neuropathy (NON), causing irreversible blindness. NON is more commonly seen in malnourished children in developing countries and purely dietary causes of this condition are rare in the western world.
In the YouGov poll, only 30 per cent of adults knew that an unhealthy diet has a possible link to sight loss and just 40 per cent knew the same about smoking. According to research, smokers double their risk of developing macular degeneration, for which limited treatments are available. Of greater concern is the finding that 28 per cent of British adults get their eyes tested less than the recommended once every two years, with nearly one in 10 (9 per cent) never getting their eyes tested.
“The results from this poll sadly are not surprising,” says Dr Rubina Ahmed, head of research at Fight for Sight. “There are currently 2 million people living with sight loss in the UK, but it is estimated that half of these cases are preventable through the right lifestyle and by accessing the right treatments. There needs to be more awareness of the need for regular eye tests, a balanced diet and of the links between smoking and sight loss.”
The charity advises people to make sure they have a balanced diet that includes nutrients such as omega-3 fatty acids, zinc and vitamins B, C and E. Recommended foods for general good health include green leafy vegetables, citrus fruits and oily fish such as salmon.
The number of people with sight loss in the UK is expected to double to 4 million by 2050.
More information can be found here.
