Clinical

Making eye contact
In Clinical
Let’s get clinical. Follow the links below to find out more about the latest clinical insight in community pharmacy.Bookmark
Record learning outcomes
Many eye problems can be treated with OTC products but it is important to be able to differentiate between common eye complaints and more serious medical conditions that need referring.

Learning objectives
After reading this feature you should be able to:
- Explain the importance of a healthy lifestyle and regular sight tests for the preservation of healthy vision
- Recommend self-care measures to manage minor eye problems
- Signpost those needing more information on specific conditions.
Eye health experts have warned that one million people in the UK are living with avoidable sight loss severe enough to have a significant impact on their daily lives – a number that is forecast to rise by a third by 2030.
Speaking at the launch of National Eye Health Week in September, chair David Cartwright said that, while some cases of sight loss are sadly unavoidable, “for many, simply going for regular eye tests and adopting a healthier lifestyle could prevent sight loss having a significant impact on lives and help people to live well for longer”.
Being physically active, he said, has been shown to reduce the risk of visual impairment by 58 per cent compared to somebody with a sedentary lifestyle, while cutting back on a diet high in meat – defined as more than 3.5oz daily (the equivalent of two small sausages) – could help cut the risk of cataracts. Meanwhile, research published in the British Medical Journal reveals as many as one in five cases (120,000) of age-related macular degeneration (AMD), the UK’s leading cause of blindness, are caused by tobacco consumption.
There is also growing evidence to suggest that diet can play a role in triggering the onset and progression of AMD, says Cartwright. One research study has shown that eating just one portion of fish a week could reduce the risk of developing AMD by as much as 40 per cent, while heavy drinking (three or more standard drinks per day) has been associated with the development of early AMD.
Poor uptake of regular eye tests (once every two years unless advised otherwise by an optometrist) is also a big risk factor for unnecessary sight loss. Almost 14 million people fail to have regular eye tests, yet an optometrist can spot signs of glaucoma years before a change in vision becomes apparent. As a result, there are an estimated 300,000 people living in the UK with undiagnosed glaucoma because they have not had a recent eye test.
Pharmacy staff may be the only people working in health many of these people see, so it is important to be on the look-out for those customers who would benefit from having their sight checked or need help to manage minor eye problems.
Let us now consider some common eye conditions.
Conjunctivitis
Conjunctivitis is inflammation of the conjunctiva (the lining of the eyelids and eyeball), which is most commonly caused by viral or bacterial infection but can also be caused by allergy, mechanical irritation or medicines.
Allergic conjunctivitis is always bilateral and is associated with itching and watery discharge. In 90 per cent of cases, allergic conjunctivitis is seasonal (hay fever) but it also commonly occurs in people with other allergic conditions, such as atopic dermatitis of the eyelids or asthma.
Bacterial conjunctivitis is more likely to be bilateral than unilateral. Eyes may be red and there may be a burning or foreign body sensation accompanied by mild itching (if at all). There is usually a purulent discharge and it may be associated with otitis media (inflammation of the middle ear; see CPD module).
Viral conjunctivitis usually starts in one eye, then spreads to the other a few days later. It is frequently associated with a recent upper respiratory tract infection or contact with an infected person. Signs and symptoms include red eye, mild to moderate itching, burning and a foreign body sensation with watery mucous discharge.
Of the two, bacterial conjunctivitis is commoner in children and viral conjunctivitis more frequent in adults.
Treatment
Pharmacy treatments for allergic conjunctivitis include artificial tears (hypromellose), mast cell stabiliser drops (sodium cromoglicate) or oral antihistamines. A cool compress placed over the eyes may also provide relief.
If these measures do not help alleviate symptoms, GPs may prescribe topical antihistamines (nedocromil sodium), NSAIDs (ketorolac) or corticosteroid drops, depending on the severity of the condition.
Bacterial conjunctivitis is usually self-limiting, resolving in five to 10 days, so may not require treatment, but pharmacy options include chloramphenicol drops and ointment. Symptoms of viral conjunctivitis may be alleviated with artificial tears or a topical antihistamine. Also self-limiting, it resolves within seven days.
Blepharitis
Blepharitis is a chronic inflammation of the eyelid margins that can affect the base of the eyelashes (anterior blepharitis) and the meibomian glands (posterior blepharitis). The inflammation is most commonly caused by pathogenic bacteria, which may result from bacterial infection, seborrhoeic dermatitis, meibomian gland dysfunction or a combination of these.
A common condition, blepharitis accounts for 5 per cent of all consultations for eye problems in primary care. Complications include conjunctivitis, dry eye syndrome, and the inability to wear contact lenses. Symptoms can be intermittent, with periods of exacerbation and remission. Eyelids may be burning, itchy and they may stick together, with symptoms worse in the morning. Signs include redness
and crusted lid margins. Both eyes are normally affected.
Treatment
Blepharitis cannot be cured but it can be managed with self-care measures. Good eyelid hygiene is the mainstay of treatment. Initially this should include applying a warm compress to the closed eyelids for 10-15 minutes twice a day, reduced to once a day for a continuous routine.
Additionally, for posterior blepharitis, massage of the closed eyelids in a circular motion can help to express meibomian gland secretions. The eyelid margins can also be cleaned to remove the debris and reduce inflammation with a cotton bud or cloth, and a cleanser. This can either be a product specifically for the purpose, or a solution of dilute baby shampoo (1:10).
Information on the cleaning technique and advice about avoiding eye make-up and not using contact lenses in periods of exacerbation will help people manage this condition.
Key facts
- Almost 14 million people in the UK fail to have regular eye tests
- People are usually unaware they have AMD until they experience problems with their vision
- ‘Primary open angle’ is the commonest type of glaucoma
Dry eye
Dry eye is a multi-factorial condition affecting the tear film, which normally keeps the eye moist and lubricated. It is usually caused by either of two main mechanisms:
• Decreased tear production
• Increased evaporation of tears.
Decreased tear production can be caused by a number of conditions, including blepharitis, allergic conjunctivitis, or may be the result of an adverse drug effect.
Increased evaporation of tears may be caused by environmental factors, such as low humidity, using computer screens or high winds.
Symptoms include dryness, grittiness and soreness, which gets progressively worse throughout the day. There may be watering of the eyes or the eyelids may stick together in the morning if it is due to meibomian gland dysfunction. Complications include conjunctivitis or, rarely, corneal ulceration.

Treatment
Hypromellose is the most commonly used product – it lubricates the eye, but requires frequent application (every 30 minutes) until symptoms improve. Alternatives are available containing polyvinyl alcohol, or carbomers, which have a longer lasting effect. Liposomal sprays are also available, which claim to repair the disrupted tear film (the cause of evaporative dry eye) to alleviate symptoms.
People with severe symptoms can also add a night-time ointment to their regimen. If drops are used frequently throughout the day, preservative-free options may need to be considered (e.g. one containing sodium hyaluronante) to avoid a build-up of preservative (benzalkonium chloride), which can cause irritation.
In addition to providing drops, ointments or sprays, advice is also useful in helping to control this condition. If blepharitis is an issue, explain the measures required to control it. Environmental conditions can also be managed with the use of a humidifier to moisten ambient air and by taking frequent breaks if using computer screens. If medication is causing dry eye, it may need to be changed and the use of contact lenses possibly limited.
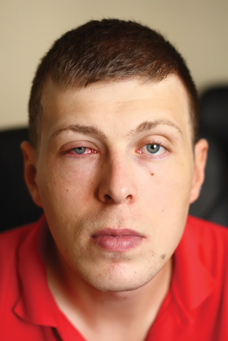
Subconjunctival haemorrhage
Subconjunctival haemorrhage can look alarming, as blood appears on the surface of the eye as a result of a burst blood vessel. Anticoagulant patients are more likely to be affected and it can happen spontaneously or, for example, as a result of coughing or sneezing.
A subconjunctival haemorrhage is usually symptomless and resolves within a few weeks. However, if accompanied by other symptoms, such as pain, loss of vision, or is caused by trauma, then GP referral is important to rule out more serious conditions such as glaucoma or uveitis.
Glaucoma
Glaucoma causes progressive optic nerve damage that can lead to loss of vision. Commonly associated with raised intraocular pressure when drainage of aqueous humour from the eye is restricted, glaucoma is normally bilateral, but it may be worse in one eye.
There are two main types of glaucoma:
• Primary open angle
• Primary angle closure.
Primary open angle is the commonest type of glaucoma. This is where the angle between the iris and the cornea is normal. It is often asymptomatic and may only be detected in routine eye examinations.
Primary angle closure glaucoma is less common. This is when the angle between the iris and the cornea is at least partially closed. It develops over time, but can cause severe sudden symptoms, including:
• Eye pain
• Red eye
• Headache
• Blurred vision
• Impaired vision with halos around lights
• Tenderness around the eyes
• Nausea and vomiting.
Treatment
First-line treatment options include prostaglandin analogues (e.g. latanoprost) or beta blockers (e.g. betaxolol). Second-line treatment options, such as carbonic anhydrase inhibitors (brinzolamide) or sympathomimetics (brimonidine) can be used if first-line treatment is unsuccessful or they can be added to primary treatment. Combination products are also available.
Uveitis
Uveitis, which is inflammation of the iris and ciliary body, is a serious condition that can lead to blindness. Urgent referral is therefore required as uveitis can only be diagnosed after a thorough assessment. It is caused by infection (e.g. herpes simplex or herpes zoster), or non-infectious causes (e.g. trauma or inflammatory bowel disease), or it may be idiopathic. Uveitis is defined based on the location of the inflammation: anterior (front of the eye), intermediate (middle) or posterior (rear).
Symptoms include pain, red eye, sensitivity to light, blurred vision, loss of peripheral vision, floaters, tearing, and sometimes headache. In most cases uveitis is bilateral.
Treatment
Treatment depends on location. For anterior uveitis corticosteroid drops are used while, for intermediate or posterior uveitis, periocular steroid injections or oral steroids can be used. Steroid drops may need to be used very frequently initially (perhaps hourly) to control the inflammation. Frequency can be reduced as the severity improves. Long-term therapy is not required in most cases, but for those with chronic or sight-threatening disease, immunomodulatory drugs (e.g. antimetabolites, calcineurin inhibitors, alkylating agents or biologics) may be required.
Complications include the development of cataracts or glaucoma, so it is important that treatment is started urgently as that has a significant influence on the prognosis. If uveitis occurs secondary to an infection, it should be treated urgently, as it is often more aggressive and may lead to permanent blindness.
AMD
Age-related macular degeneration is a progressive eye condition that affects the central area of the retina (macula), which can result in loss of central vision. Ageing results in an increase in the breakdown of light sensitive cells. As the disease progresses, the reduced number of light sensitive cells affects the vision. There is also a growth of new blood vessels which, unlike normal retinal vessels, easily break and leak blood constituents, resulting in distortion and scarring of the retina.
People are usually unaware they have AMD until they experience problems with their vision. However, it may be detected earlier during a routine eye examination.
Symptoms include:
• Loss of visual acuity and contrast sensitivity
• Size or colour of objects appearing different with each eye
• Abnormal dark adaptation
• Light glare
• A perception of flickering or flashing lights
• Visual hallucinations.
There is no cure for AMD, but there is plenty of advice you can provide which may slow the progression of the disease including stopping smoking and eating a healthy, balanced diet rich in leafy green vegetables and fresh fruit.
In addition, some ophthalmologists recommend dietary supplements for people with intermediate AMD in one or both eyes, or advanced AMD in one eye, to help to prevent or delay the condition from progressing.
The supplements contain vitamins and minerals that are antioxidants (e.g. vitamin C 500mg, vitamin E 400IU, lutein 10mg, zeaxanthin 2mg, zinc 25mg and copper [cupric oxide 2mg]), which may prevent cellular damage in the retina by reacting with free radicals produced in the process of light absorption.
Diet can play a role in triggering the onset and progression of AMD
When to refer eye problems
People should be referred to their GP or local optometrist if they have any of the following symptoms:
• Vision is affected
• Eye pain
• Unilateral red eye
• Photophobia
• Eye injury (trauma or chemical injury)
• Recent eye surgery
• Foreign body in the eye
• Unequal or misshapen pupils, or abnormal pupillary reactions
• Conjunctivitis in a baby during the first 28 days of life.
Also consider referring:
• People with rheumatoid disease
• Contact lens wearers.

