Learning update: Cracking patients' skin conditions
In Learning
Follow this topic
Bookmark
Record learning outcomes
While the healthcare system’s focus is on tackling the coronavirus pandemic, patients must continue to deal with long-term medical conditions such as chronic skin disorders – often without the usual backing of their GP or dermatologist. Pharmacy can help fill the gap

Learning objectives
After reading this feature you should be able to:
• Appreciate the incidence, key symptoms and wider psychological impact of common yet chronic dermatological problems
• Advise skin disease sufferers on recommended treatment options z Understand the potential role for pharmacy in early community-based screening for suspicious moles.
Community pharmacists are well positioned to advise on the symptomatic management of chronic skin conditions with both OTC and prescription medications, as well as helping to address acute problems if they arise.
There is also an important role to play in offering self-care advice and providing counselling and support for patients struggling with the mental health impact of long-term skin conditions.
Psoriasis
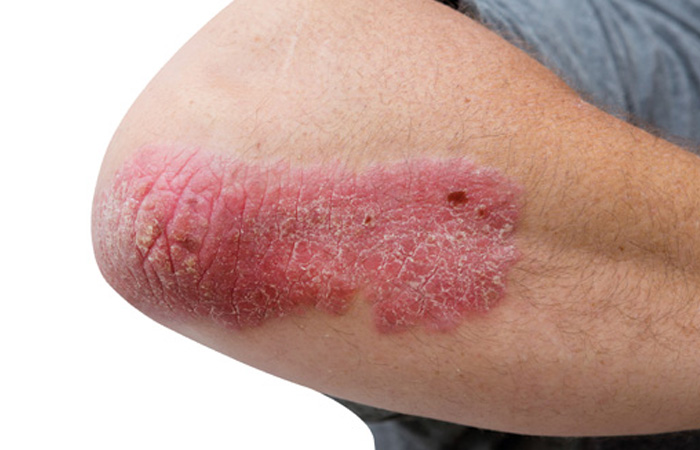
Between 2 and 3 per cent of the UK population suffer from psoriasis, which means approximately 18 million people are affected.1 Psoriasis is caused by an acceleration in the normal process of skin renewal and replacement from several weeks to just a few days. Excess skin cells build up on the skin surface forming raised plaques, which can also be dry, itchy and sore. Plaques appear red on Caucasian skin and darker on darker skin tones, and are often covered in silvery scales. A significant proportion of psoriasis patients (over 10 per cent) will also suffer with concomitant joint disease.2
There are several different types of psoriasis, which typically affect different areas of the body. By far the most common type is plaque psoriasis, which accounts for 80-90 per cent of cases and tends to affect the elbows, knees, scalp and lower back.3 Although it is a chronic condition, psoriasis often follows a waxing and waning disease course with periods of absent/mild symptoms interspersed with more severe flare-ups.
For most patients, treatment for plaque psoriasis follows a stepwise pathway starting with topical products and moving onto phototherapy or stronger systemic therapies if required. Pharmacists can play a key role in optimising outcomes from topical therapy which, for many patients, will be the only treatment required to control their symptoms. Promoting adherence is very important as topical treatments can prove time-consuming to apply and may be smelly, sticky and staining to clothes.
Emollients are the first line of topical therapy and help to reduce itch and scale, while simultaneously boosting the efficacy of other topical treatments. Ideally, emollients should be applied at least three or four times a day and it is important to leave at least half an hour before applying other topical treatments.
Creams or ointments containing corticosteroids of varying strengths are the next rung on the treatment ladder. These should only be applied to small areas or very thick patches of plaque as their overuse can result in skin atrophy. Other topical treatment options include vitamin D analogue creams, deployed either alone or in combination with topical steroids to target mild or moderate psoriasis, and immune-suppressive calcineurin inhibitor creams or ointments that are typically used for difficult-to-treat sensitive areas such as the genitals and skin folds.
While vitamin D analogues are generally well-tolerated, patients should be advised that calcineurin inhibitors can cause initial skin irritation or burning/itching, although this typically resolves within a week. Older topical treatments, such as coal tar and dithranol, are less commonly used today. Patients with more severe or intractable psoriasis that fails to respond to topicals may require phototherapy or systemic treatments such as biologic therapies administered under the care of a dermatologist.
Lifestyle measures that can help to reduce the risk of exacerbations in patients with psoriasis include stopping smoking, sticking to recommended alcohol limits, losing weight, and managing stress and depression/anxiety.
Key facts
• Psoriasis, acne, eczema and dry skin are common dermatological conditions that affect a significant proportion of the UK population
• Topical treatments such as emollients and corticosteroids are the mainstay of treatment for many of these chronic skin conditions
• Long-term dermatological disease can have a significant adverse impact on a sufferer’s quality of life and mental wellbeing.
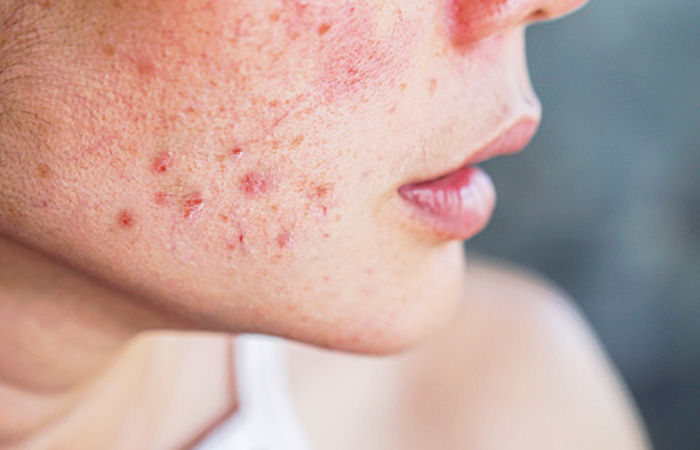
Acne
Acne is an almost unavoidable scourge of adolescence and young adulthood, affecting around 95 per cent of 11-30-year-olds to some extent.3 To tackle this widespread skin complaint, a range of topical OTC acne products are available containing different active ingredients.
Benzoyl peroxide features in a number of creams and works by removing acne-causing bacteria and dead cells from the skin. Common side-effects include skin dryness, redness and peeling. If this occurs, customers should pause treatment for a few days before restarting or switch to a lower strength product. An oil-free moisturiser can be recommended alongside benzoyl peroxide to combat skin dryness.
Salicylic acid, found in products from face washes to cleansers, helps to promote skin shedding and unblock pores. It is most effective against non-inflammatory acne.
Nicotinamide is an anti-inflammatory agent applied to the skin twice daily, usually as a gel.
Unlike benzoyl peroxide, it will not bleach clothes or bedding.
Other spot-targeting face washes are also available containing mild antiseptic or antimicrobial ingre- dients that can reduce the effects of the P. acnes bacteria. Customers should be advised that it can take up to three months to see results from acne treatments, which must be used regularly to achieve best results. Once the skin has cleared, treatment should be continued to keep spots at bay over the longer-term.
It is important to encourage sufferers to resist the temptation to pick or squeeze spots as this can lead to permanent scarring. Any customer with acne that fails to respond to an adequate course of OTC intervention, is characterised by severe spots or scarring, or is causing significant psychological distress, should be referred to their GP.
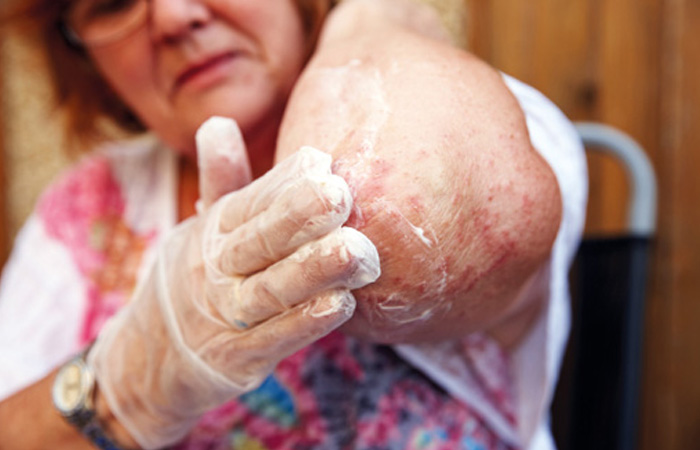
Eczema and dry skin
Eczema is a common dry skin condition mainly seen in the early years of life, with as many as one in five children affected.4 Mild eczema is characterised by patches of dry, itchy, scaly, red skin, while more severe cases can lead to weeping, crusting and bleeding. Eczematous skin fails to produce sufficient amounts of fats and oils and is unable to retain enough moisture to maintain the skin’s plump protective barrier. Emollients replace this essential moisture and are therefore the linchpin of treatment for eczema.
On the question of which emollient is best, the National Eczema Society advises that: “Eczema is a very individual condition and different emollients tend to suit different people. The best emollient is the one you like, because then you will use it more often. Always test new products on a small area of unaffected skin for 48 hours in case you have a reaction.
“You may need to use different types of emollient on different parts of the body to obtain the best hydration and to restore the skin’s barrier function to normal. You may also like to alternate between a lighter emollient during the day and during the warmer months, and a greasier one at night and when the weather is colder.”4
For maximum efficacy, emollients should be used by patients at least twice daily – more often if the eczema is flaring – at a total dose of at least 500g per week (250g for children). Leave-on emollients or emollient soap substitutes should be used to wash with and emollients applied gently after bathing in the direction of hair growth. Pharmacists and their teams should counsel patients to apply emollient to all areas of the skin, not just those affected by eczema, and continue to use emollients even if the condition of the skin appears to improve.
Topical steroids are another first-line treatment option for eczema that tend to be used in short bursts to bring flare-ups under control. Paste bandages and wet wraps can provide additional relief for patients who find scratching a particular problem. Sedating antihistamines can also be recommended to aid sleeping, although they do not work against the itch symptoms of eczema and are not recommended for long-term use.
Important self-care advice for eczema sufferers includes reducing scratching where possible and avoiding potential triggers such as perfumed soap products, wool and synthetic materials, and household irritants like washing powder, dust and pets. Patients with severe eczema should be advised to see their GP to discuss prescription treatment options such as oral steroids or immunosuppressants, phototherapy and biologics.
As with eczema, emollients form the cornerstone of treatment for any customer complaining of a dry skin condition. Dry skin in differing forms and severity affects between 15-20 per cent of the population at some point in their lives. A range of emollient creams, lotions and shower/bath products are available OTC.
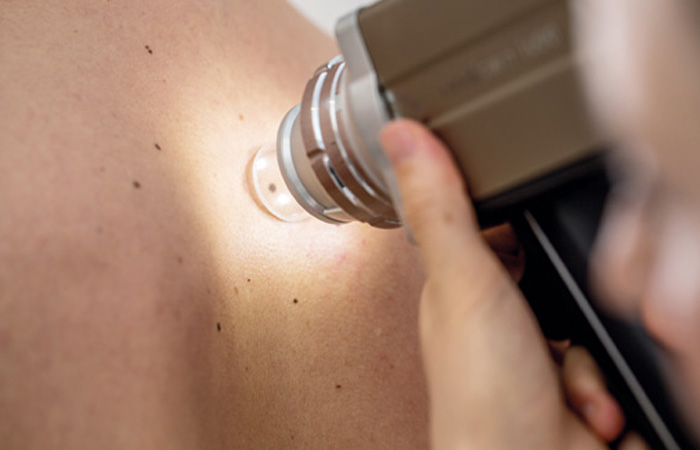
Mole screening — an important opportunity for pharmacy
With Covid-19 dominating the healthcare agenda, mole checking has been just one of the many routine health check-ups to fall by the wayside in recent months.
Although not within their traditional remit, evidence suggests that community pharmacists could have an important role to play in the early detection of suspicious moles and improved diagnosis of malignant melanoma.
A recent study on the use of mole scanning in the community pharmacy setting published in the Journal of Pharmacy showed this to be an effective method for triaging patients.7,8 In the study, almost 10,000 moles were scanned across 50 pharmacies as part of the Boots Mole Scanning Service. This service is provided by ScreenCancer UK and employs a powerful imaging tool to capture detailed pictures of the skin across different layers, which are then sent for analysis by a dermatology specialist.
Of the moles scanned in this study, the vast majority (88 per cent) required no action but 0.7 per cent referred for further follow-up ultimately led to a confirmed diagnosis of malignant melanoma. This equates to 69 cancerous moles that would otherwise have gone undetected without pharmacy screening. Early detection and treatment of malignant melanoma are known to be crucial in preventing mortality.
“During the Covid-19 pandemic, many people might have delayed seeking their GP’s advice, which makes services like this even more important,” says Marc Donovan, Boots chief pharmacist. “This service offers customers increased accessibility and convenience, particularly when early detection and intervention is critical.”
David Wright, professor of pharmacy practice at the University of East Anglia and co-author of the paper, agrees. “This evaluation shows again the contribution that community pharmacy can make to the health of the nation. Mole screening services of this nature enable potentially serious conditions to be detected much earlier and relieves pressure on GPs by providing an alternative screening route.”
Patient perspectives
Chronic skin conditions like eczema and psoriasis can have a negative impact on numerous aspects of a patient’s life, affecting not only physical health but also mental wellbeing, quality of life and long- term opportunities.
The overwhelming majority of skin disease patients (98 per cent) feel their condition affects their emotional and psychological wellbeing, according to recent survey data collated by the All Party Parliamentary Group on Skin (APPGS).5 Carried out in 2020, the survey collected evidence from over 500 patients, 100 clinicians and 16 organisations operating in the field of dermatology. It found that the psychological impact of skin disorders was debilitating and seen across all aspects of patients’ lives including self-esteem, sleep and intimate relationships.
In total, 87 per cent of people with skin disorders reported a negative impact on their social life or leisure/sporting activities and 69 per cent said their condition had a negative effect on work or education. Perhaps most alarmingly, one in every 20 patients with dermatological problems also described having suicidal thoughts.
“This timely report comes out during a period of unprecedented psychological distress for many people living with a skin condition,” says Sir Edward Leigh MP, APPGS chair.
“The Covid-19 pandemic has exacerbated anxiety and stress amongst those already known to experience significant appearance-related distress... It is clear, from the powerful and moving testimony we received from skin patients, that many others experience similar episodes of discrimination, rejection and negative reactions. This can be alienating and deeply distressing.”
Eczema Unmasked, a report produced jointly by the National Eczema Society (NES) and Leo Pharma, confirms the heavy psychological burden carried by people with chronic skin conditions.6 Almost three-quarters of adults (74 per cent) in this report said eczema negatively impacted their mental health and two-thirds (66 per cent) of patients confessed to feelings of loneliness or social isolation because of their skin condition.
As in the APPGS survey, the impact of skin conditions on physical functioning, sleep and work opportunities was clear. Nearly half of adult responders said eczema had negatively affected their ability to do paid work and jeopardised their professional career.6 Social stigma was another key issue revealed by the report, with 85 per cent of respondents reporting embarrassment as result of their eczema and four in five admitting to feeling jealous of people with more ‘typical’ skin.
Perhaps most pertinent for pharmacy was the finding that patients with chronic dermatological disorders can find it challenging to access care and treatment, with the absence of psychological support proving particularly stark.
The overwhelming majority of skin disease patients feel their condition affects their emotional and psychological wellbeing
Does severe atopic eczema increase mortality?
Severe atopic eczema seems to increase overall mortality, according to a UK study.
Researchers used primary care records to match 526,736 patients with atopic eczema with 2,567,872 controls. Overall, all-cause mortality was 4 per cent higher in people with atopic eczema compared with controls, a statistically significant difference. Deaths due to infections (14 per cent), digestive diseases (11 per cent) and genitourinary causes (8 per cent) showed “somewhat stronger associations”. The absolute risk of death was 1,496 and 1,435 per 100,000 people per year in those with and without atopic eczema respectively.
Mortality rose as eczema severity and activity increased. Patients with severe atopic eczema were at a 62 per cent increased risk of mortality compared with controls. The risk of death from infections (hazard ratio [HR] 2.85), respiratory diseases (HR 2.20) and genitourinary causes (HR 2.10) all more than doubled. The association between mortality and eczema was also stronger in people with the most active disease.
Dysfunction of the skin barrier and immune system may account for the link with infections. Adjusting for systemic immunosuppressants did not change the relationship, suggesting these drugs were not responsible. Lower physical activity and reduced sleep quality may contribute to the increased cardiovascular mortality.
Possible mechanisms for the increased mortality related to urogenital disease in people with severe atopic eczema include metabolic syndrome and cardiovascular disease, use of nephrotoxic drugs or chronic inflammation. Increased mortality due to respiratory disease may relate to misclassification of asthma, adverse effects of drugs or smoking. Further studies are needed to clarify the mechanisms.
“Recent evidence has led to a paradigm shift in how atopic eczema is perceived, from focusing on skin symptoms and associated allergic diseases, to understanding that the disease may be associated with a range of important medical outcomes,” says lead author Sinéad Langan, professor of clinical epidemiology at the London School of Hygiene & Tropical Medicine.
“Although the absolute risk of death from severe eczema is low, our findings suggest that those with severe or more active forms of the disease do face a higher risk of dying from associated health issues.”
References
- Psoriasis Association. About Psoriasis: Psoriasis & Treatments
- NICE. Psoriasis: assessment and management. Clinical guideline [CG153]. Updated September 2017
- NHS
- National Eczema Society
- British Association of Dermatologists (BAD). Parliamentary report reveals worrying lack of mental health support for skin disease patients. Press release: Sept 22 2020. Available at: Parliamentary report reveals worrying lack of mental health support for skin disease patients – BAD Patient Hub
- Leo Pharma and National Eczema Society (NES). Eczema Unmasked. October 2020. Eczema Unmasked Report.pdf
- Kirkdale C et al. Accessing Mole-Scanning through Community Pharmacy: A Pilot Service in Collaboration with Dermatology Specialists. Journal of Pharmacy 2020; 8(4): 231
- Boots. Boots UK Supports the NHS with Convenient Mole Scanning Service. Press release: Dec 16 2020. Boots UK – Boots UK Supports the NHS with Convenient Mole Scanning Service.
