Growing pains
In Clinical
Follow this topic
Bookmark
Record learning outcomes
Feeling comfortable in your own skin can be a challenge at any age, but for today’s adolescents, social media is making things a lot more complicated when it comes to their health

Learning objectives
After reading this feature you should:
- Have a good awareness of young people’s health issues
- Understand how to approach customers in this age range
- Be able to advise on treating a number of common ailments in young adults
A recent study exploring behavioural differences between Generation Z (young people born between the mid-1990s and early 2000s) and Baby Boomers (mid-1940s to mid-1960s) found that young people are clearly affected by what they see online.
In the study by research firm Pegasus,1 40 per cent of young people said they felt jealous or unconfident when looking at fitness or beauty images (compared with 10 per cent or less among the older generation). Almost half of the adolescents admitted feeling sad that they don’t look like the images, with 47 per cent saying they felt pressured to lose weight or tone up.
It is little wonder that research by University College London concludes that young people are more likely to feel depressed, self-harm or fail to get a full night’s sleep than they would have 10 years ago.2 In fact, the Association for Young People’s Health reports that some 75 per cent of mental health problems actually start before the age of 24 years (the age when adolescence is said to end).3
Other experts warn that this life stage is also the prime time for other addictive behaviours such as alcoholism, drug use and eating disorders to settle in and have a lifelong impact – 70 per cent of preventable deaths from non-communicable diseases in adults worldwide are thought to result from behaviours established in adolescence.4
Adolescence can also be a particularly critical time for young people with existing conditions, such as type 1 diabetes, epilepsy, juvenile arthritis and asthma, as they begin to make the move from parental supervision to self-management. For its part, Asthma UK is calling for more to be done during this transitional phase, highlighting that two-thirds of 18-to-29 year-olds are still not receiving basic care.5
Eighty-eight per cent of people in this age bracket have uncontrolled asthma, says the charity, and make up the highest proportion of emergency visits (34 per cent). It attributes these high numbers in no small part to the prescription charges that kick in for asthma sufferers at the age of 18 years, leading some to choose between having a ‘preventer’ or ‘reliever’ inhaler, rather than having to pay for both.
Underutilised
Given the long-term repercussions of health issues during adolescence, it is unfortunate that many healthcare professionals feel uncomfortable dipping a toe into these waters – which is often due to confusion about the rules on consent and confidentiality for younger adolescents, or a lack of confidence about initiating a conversation with someone in this age group.
This has led to pharmacy services being vastly underutilised by younger people, says Dr Nicola Gray, a pharmacist who has specialised in young people’s health through research and advocacy work. Community pharmacies represent the most accessible healthcare available, often tending to be where young people live, work or shop, she says, but despite this, the relationship between pharmacy and adolescents is rarely seen as one to be nurtured.
“Instead, young people are viewed as individuals in need of a certain service, such as emergency contraception, substance misuse or STI testing, or even as a potential shoplifter who needs to be followed about – rather than someone who might just want to talk about their health.
“This tends to preclude them being welcomed in the same way as older age groups and invited to engage in conversation. For me, that is a great shame, because young people are thirsty for knowledge and a pharmacy is perfectly placed to fulfill this type of navigator role.”
Dr Gray’s point is supported by the Pegasus research poll, which shows that while at least 50 per cent of Generation Z claim to visit their GP each year, few come away satisfied, with a large proportion feeling that their doctor dismisses them as if they are imagining or exaggerating their symptoms.1 What’s more, the report found that nearly half of Generation Z (46 per cent) say they would struggle to tell their doctor if they were experiencing mental health problems.
Confidentiality and consent
The Royal College of General Practitioners (RCGP) has a resource for reference and training ahead of consultations with children and adolescents.
Confidentiality and Young People6 covers all the regulations governing consent and confidentiality issues. A pdf copy can be downloaded from the RCGP.
Be the change
On the face of it, community pharmacy would seem to be an obvious first place to go for young people – but with almost a third of young people who took part in the Pegasus study believing that pharmacists have not had enough training to discuss health issues, there is clearly work to be done to establish that all-important trust. In order to accomplish this, Dr Gray advocates the three Bs:
- Be welcoming: young people need to feel comfortable in a pharmacy, so everyone in the team must be on board and well trained in how to initiate conversations with adolescent customers and patients
- Be patient: don’t expect the same results as from an adult consultation. Building any meaningful rapport may take several conversations with a younger customer, with information coming in layers until the root of the problem is reached
- Be authentic: adolescents don’t require pharmacists to know their world, so don’t pretend. What they are looking for is a friendly, trustworthy professional.
Weight management
Most children are prone to some puppy fat that is naturally shed as the body goes through the stages of adolescence. However, the pressure to emulate certain images may cause some teenagers to obsess over their weight and embark on fad diets and other unhealthy choices that could lead to eating disorders.
Reinforcing the need for a healthy balance is essential. The British Nutrition Foundation offers a resource for teenagers that covers everything they need to know at this stage of life.

Young people are more likely to feel depressed, self-harm or fail to get a full night’s sleep than they would have 10 years ago
Common health issues during adolescence
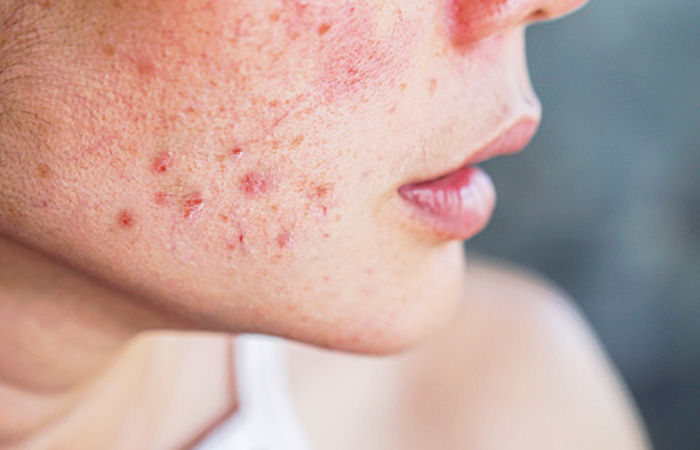
Acne
Acne is common among teenagers and is often sparked by hormonal changes during puberty or menstruation. Advice should include keeping skin clean and washing with gentle, non-comedogenic products, rather than harsh scrubs that may cause irritation.
Numerous OTC treatments are also available for mild forms of acne and contain active ingredients such as benzoyl peroxide or nicotinamide to kill bacteria and make the skin less oily. In severe cases, customers should be referred to their GP, which may result in an antibiotic or topical retinoid cream/gel being prescribed.
Period pain
Abdominal cramping with spasms of varying intensity can occur at various stages of a menstrual cycle, but usually present for 48-72 hours, when bleeding is at its heaviest. This pain can usually be managed with NSAIDs, such as ibuprofen, naproxen or mefenamic acid, but if the pain is severe a GP may also prescribe hormonal contraceptives. Self-help measures include relieving pain with a hot water bottle, self-heating patch or microwave-heated cushion. Regular exercise has been linked to lower levels of menstrual pain.
Dandruff
The exact cause of dandruff is unknown, although it has been linked to an excess of oil (sebum) in the skin. Typically, dandruff starts during the teenage years when increased hormone levels cause more oil production. Dandruff isn’t contagious and in most cases an OTC shampoo will control the problem. If symptoms persist after four to six weeks, a change of product should be recommended. If the problem doesn’t go away, a GP may prescribe a stronger shampoo or topical steroids.
Body odour
Hormonal changes typically make the sweat glands in the armpits, groin, feet and palms much more active, with any skin bacteria often leading to body odour. Good personal hygiene, applying a deodorant (designed to mask any odour) or antiperspirant (which includes chemical ingredients to dry up or prevent sweating) and changing clothes regularly will all help. Recommend clothing made with natural fibres, such as cotton or linen, as this will also absorb sweat better than other materials. Dedicated sprays and powders can also be used on the feet or in shoes. If the problem persists, a GP may decide to prescribe a stronger antiperspirant as a next step.
Shaving
During puberty, hair will begin to develop on both girls and boys. Unless there is an obvious requirement, young men are not advised to shave every day, but to remove patches of hair when necessary. Electric shavers or razors may be used, with the
best time for wet-shaving after a bath.
Recommend splashing the face with warm water and always advise customers to go with the grain, advocating soft, short strokes. Razors/blades should be changed regularly and recommend they have an antiseptic styptic pencil to hand to address those inevitable nicks.
Delivering value
Once the right culture and attitudes are in place, there are a number of ways pharmacies can add value, says Dr Gray.
Talk about medicines
Inviting a young person in for a review of their medications is a great way to build on an existing relationship and support an eventual move from parental supervision to self-management.
That is not to say parents should be excluded. The aim is to build a young person’s confidence, while keeping their support structure in place. Normalising the process will help both parents and child to make the transition. If they don’t have one in place already, help them develop an action plan for any emergencies.
Tailor advice
Make a point of asking questions and look to build up a picture of the young person’s hobbies and activities so that any consultation will be directly relevant for them. For example, with someone who enjoys sport, where it is appropriate suggest smoking cessation products or check their asthma inhaler technique.
Set the scene
Reaching the age of 18 years can seem like falling off a cliff to some young people, with prescription charges kicking in as well. Pharmacists could contact some of their existing younger patients and invite them in for a chat to discuss how the changes will affect them personally. Display signs in the pharmacy to encourage other young people to make contact.
Be visible
Post notices in the pharmacy or other community venues inviting young people to learn more about the adolescent health services on offer. Some GP clinics invite young people in once they reach the age of 13 years so they can learn what is on offer.
Understand the issues
Don’t just pay lip service to any adolescent health problem. Take the time to make sure that everyone in the pharmacy team can appreciate things from a younger person’s perspective. Be conscious of any fears, such as side-effects, weight gain or skin rashes that might affect appearance or relationships, and address them in your conversations.
Step up – and step in
If it is felt a young person is wasting their time on an OTC product when they really need to see a GP, intervene discreetly and speak to them. A good example is when a case of acne is beyond first-line washes and scrubs. It can be tricky to initiate this sort of conversation, but the person will respect the pharmacist more in the long run and is more likely to approach them directly another time.
Mind your language
Don’t dumb down. Treat younger customers as any others. A good approach is to use the correct names for medications and simple everyday language when discussing any symptoms or possible side-effects. GPs who make an effort to engage well with young people have reported that it improves their conversations with all their patients. Think about the things most relevant to them when giving medicines advice – will it affect their concentration at school or their social life, for example?

Embrace technology
Social media often gets a bad press but it can also be a force for good. Be aware of the best forums, apps and websites that can help promote good health. For example, headmeds.org.uk offers young people information on everything they need to know about mental health conditions and corresponding treatments.
Signpost services
Help young customers find appropriate advice and treatment by suggesting what other healthcare services within the community they could access. This can cover a host of things – including GPs and specific support groups, as well as where to go for any missed immunisations, such as the HPV vaccine, which is now available up to the age of 25 years. Consider approaching support groups in person in order to establish a tie-up and to ensure everyone is engaged when it comes to helping young people with their health issues.
Treat your younger customers as you would any others
Implementing You’re Welcome
In the early 2000s, the Government unveiled a set of criteria for youth-friendly services. Known as ‘You’re Welcome’, the framework was aimed at health professionals from multiple disciplines. This is currently being refreshed as part of a project supported by Public Health England, NHS England and the Department of Health and Social Care.
The pilot, which includes a self-assessment toolkit, aims to ensure best practice within adolescent health and is being led by the British Youth Council, Association for Young People’s Health and Youth Focus North West.
‘You’re Welcome’ covers 10 topic areas:
- Accessibility
- Publicity
- Confidentiality and consent
- Environment
- Staff training, skills, attitudes and values
- Joined-up working
- Young people’s involvement in monitoring and evaluation of patient experience
- Health issues for young people
- Sexual and reproductive health services
- Specialist child and adolescent mental health services (CAMHS).
Find out more about ‘You’re Welcome’
References
- Generation Z: The Future of Health & Wellbeing Report – Behavioural Differences Between the Generations/Conducted by 3GEM on behalf of Pegasus in October 2018 and Pegasus study groups in May 2018
- Adolescent health: Teens ‘more depressed and sleeping less’
- Association for Young People’s Health. Young People’s Health Update 2017
- Kuruvilla S, Sadana R, Villar Montesinos E, Beard J et al. A life-course approach to health: synergy with sustainable development goals. World Health Organization Bulletin 2018; 96:42-50
- The Reality of Asthma Care in the UK. Annual Asthma Survey Report 2018. Asthma UK
- Confidentiality and Young People. Royal College of General Practitioners
