Conference call: British Association of Dermatologists
In Clinical
Follow this topic
Bookmark
Record learning outcomes
The 96th annual meeting of the British Association of Dermatologists took place last month in Birmingham. Dr Christine Clark highlights some of the key pieces of research.
Compelling evidence for topical retinoids in acne
There is compelling evidence for the use of topical retinoids as part of an acne treatment regimen€, Dr Alison Layton, consultant dermatologist, Harrogate & District NHS Foundation Trust, told participants at a satellite symposium sponsored by Galderma.
Retinoids exert a direct effect on the abnormal keratinisation that occurs in sebaceous follicles in acne and thereby prevent the formation of comedones. In addition they have an anti-inflammatory effect, which is advantageous in combatting the inflammatory element of acne.
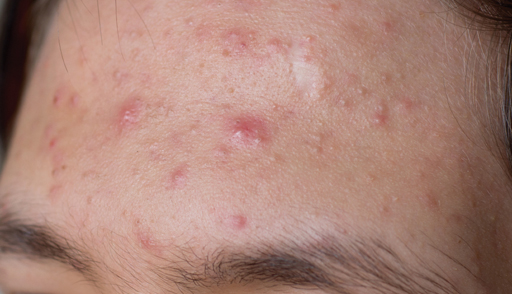 Adapalene (applied topically) has a strong anti-inflammatory action and reduces both inflammatory and non-inflammatory lesions of acne in tandem.
Adapalene (applied topically) has a strong anti-inflammatory action and reduces both inflammatory and non-inflammatory lesions of acne in tandem.
The current evidence-based guidelines from the European Dermatology Forum recommend the use of a topical retinoid together with an oil-free moisturiser for comedonal acne. Over a 12-week period this significantly reduces the number of microcomedos €“ the precursor lesions of acne €“ but they return if treatment is stopped, says Dr Layton.
Many people do not prescribe topical retinoids because of lingering concerns about safety in pregnancy. Although systemic retinoids are definitely teratogenic, a recent systematic review has confirmed that there is no difference in rates of spontaneous abortion or foetal abnormalities between women exposed to topical retinoids during pregnancy and controls (Kaplan 2015).
€If your patient gets pregnant while using topical retinoids, you can reassure her that the foetus will not be harmed as a result of the retinoid,€ Dr Layton said. €We are definitely under-using topical retinoids €“ we are only treating acne half as well as we could do,€ she concluded.
Vitamin D influences MM aggression levels
Many people in the UK are vitamin D deficient, according to current estimates. Vitamin D deficiency is maximal in the spring but people living in the north of the UK can be affected all year round, Professor Julia Newton-Bishop, consultant dermatologist, University of Leeds, told the conference.
Even after an average weekend of sun exposure (six hours in the sun), most people still fail to reach the optimal 60 nanomol/L blood level, according to one study in Yorkshire. €The UK is particularly afflicted with low sunlight levels,€ Professor Newton-Bishop said, adding that we appear to need more sun exposure than the literature suggests.
The situation concerning malignant melanoma (MM) is confusing, she said. People with pale skin and/or family histories of MM have been advised to avoid sun exposure but recent research shows that adequate levels of vitamin D can be important in determining the aggressiveness of melanomas. Lower levels of vitamin D are associated with thicker (worse) tumours and poor survival, said Professor Newton-Bishop.
When MM is diagnosed, vitamin D levels should be checked and supplements offered if levels are low, in accordance with the NICE guideline. Melanoma patients should still avoid intense sun exposure €“ when the UV index is at or above three €“ and definitely avoid getting burned, she says.
Although it should be possible to get just enough sun exposure to make the required vitamin D without getting burned, in practice this is difficult for those with pale skin. Newton-Bishop recommends using a sunscreen and taking vitamin D supplements, the dosage of which should follow Public Health England guidance. Very high doses of vitamin D can have immuno-suppressive effects, she warned.
Daylight PDT suits mild AKs
Daylight photodynamic therapy (PDT) is a very effective treatment for mild actinic keratoses (AKs), according to Dr Sally Ibbotson, a consultant dermatologist from Dundee.
While one patient reported it was €blooming freezing€ and another that he needed two hot water bottles while undergoing treatment, patients in Dundee also reported a €fresher€ and €more youthful€ appearance to their skin, in addition to clearance of their AKs.
PDT is a way of treating AKs, the precursor lesions of squamous cell carcinomas, particularly lesions on the head and face. A photosensitiser (e.g. methylaminolaevulinate [MAL]) is applied, followed by irrad-iation with light to activate the photosensitiser and release reactive oxygen species that kill premalignant cells.
Conventional PDT involves application of MAL, a three-hour wait, and then irradiation using a suitable lamp. About 50 per cent of patients require pain relief after treatment, according to Dr Ibbotson.
The amount of pain can be reduced by giving lower doses of light over a longer period or by using daylight, she explained.
Daylight PDT is suitable for people with diffuse, thin AKs on the face and scalp. A non-reflecting sunscreen (SPF 30) is applied first to prevent sunburn during treatment, then MAL is applied thinly. Within 30 minutes the patient starts a two-hour period of exposure to daylight. This has to be outdoors or in a greenhouse or conservatory.
The treated area can scale and crust after treatment, so it is important to warn patients that their skin will look worse before it looks better.
Daylight PDT can be delivered in the UK between March and October, provided that it is not raining. It just has to be warm enough for the patient to spend two hours outdoors with his/her head uncovered (above 10°C).
Dupilumab described as 'life changing'
Severe eczema can have a devastating effect on people's lives, according to Professor Michael Cork, consultant dermatologist, Sheffield. One boy with eczema recounted how he first attempted suicide at the age of eight because of the misery of living with his skin condition. Another patient had received treatments to the value of £250,000 in one year, but still had severe eczema.
Understanding of the molecular basis of atopic eczema is growing and a large number of new drugs €“ many of them monoclonal antibodies €“ are now being tested against the disease. Dupilumab, designated as a 'breakthrough therapy' by the FDA, blocks signalling through the IL4/IL13 receptor-ligand system, an early step in the inflammatory process that drives eczema.
In a published study of dupilumab in severe eczema, 84 per cent of patients experienced a 50 per cent reduction in disease severity after three months. €My experience is that we saw improvements at six weeks and there was continued improvement over the months that followed, up to six or nine months,€ said Professor Cork. Patient feedback indicated that the treatment was €life changing€. One of the side-effects of dupilumab is conjunctivitis but this can be managed with artificial tears.
Many other potential targets have been identified in the inflammatory cascade that causes eczema and a host of novel drugs are now in development.
