Tackling the opioid crisis
In Clinical
Follow this topic
Bookmark
Record learning outcomes
The prescription opioid time bomb has focused clinical attention on chronic pain and inspired a raft of management initiatives across the UK

Learning objectives.
After reading this feature you should be able to:
- Appreciate the seriousness of the opioid crisis
- Play a more prominent role in managing chronic pain
- Help patients tounderstand that medication is not necessarily the only way to tackle pain.
Pain is deeply personal. People born with congenital insensitivity to pain can handle burning coals, stab knives into their arms, and chew off their fingers and toes without experiencing even a minimum of discomfort. Some people born without arms or legs endure phantom pain in a limb that never developed. The rest of us are between these extremes – our perception of pain severity, as well as our emotional, biological and behavioural responses, can vary dramatically for the same pain producing (nociceptive) stimulus.
Acute pain is a biological alarm, warning of injury, so pain often needs to be intense, intrusive and unpleasant – or a person would just ignore the alarm and exacerbate the damage. About 28 million adults in the UK suffer from chronic pain, generally regarded as pain that lasts for more than three months1.
A meta-analysis of 19 studies reported that between 35.0 and 51.3 per cent of adults in the UK live in chronic pain, which takes numerous forms, including chronic widespread pain (experienced by 14.2 per cent of adults), chronic neuropathic pain (8.2-8.9 per cent) and fibromyalgia (5.4 per cent). Chronic pain also seems to become more common as we age, with prevalence rising from 14.3 per cent in people aged 18-25 years to 62.0 per cent in those older than 75 years1.
Despite being common, the NHS doesn’t manage chronic pain particularly well. “The NHS has very limited resources,” says Helen Macdonald, accredited practitioner, supervisor and trainer for the British Association for Behavioural and Cognitive Psychotherapies (BABCP). “Proportionally, however, very few of these resources are directed at pain management considering the number of people who live with persistent pain.”
“Prescribers failing to undertake any meaningful review of analgesic effectiveness following initiation leads to numerous clinical concerns. These include overprescribing of opioids, gabapentinoid abuse and patients self-medicating with large doses of weak opioids,” adds Lee Wilson, consultant pharmacist at Doncaster and Bassetlaw Hospitals NHS Trust. “The key message should be: review with a view to stop ineffective analgesics.”
As a healthcare community, we are looking at how we can reduce ineffective opioid use, says Wilson, who is also chair of the UK Clinical Pharmacy Association pain management group. “Locally, our opioid prescribing levels seem to have reached a peak and are moving, albeit slowly, downwards.”
Several factors have contributed to the decline in opioid use, he says, including changing attitudes across the primary and secondary care interface, interventions from clinical commissioning groups, including letters to GPs for each patient deemed to be on high-dose opioids, and increasing cognisance of the Opioids Aware guidance (see ‘Further sources of information’). However, improving pain management means looking beyond prescription medication.
Developing a service
“Evidence-based pain management services include, as a minimum, medical interventions, physiotherapy and cognitive behavioural therapy,” says Helen Macdonald, who is also a consultant in cognitive behavioural therapy (CBT).
“Ideally, pain management services should benefit from additional specialist input from, for instance, expert patients, occupational therapy, pharmacy and, perhaps, psychiatry. Professionals should collaborate with their patients to promote self-management of pain and use the evidence base to deliver a biopsychosocial approach.”
The Improving Access to Psychological Therapies (IAPT) services, for example, aim to improve psychological wellbeing for people with chronic pain and other long-term health conditions (LTCs). About 40 per cent of people with depression and anxiety disorders have a LTC and about 30 per cent of people with a LTC and 70 per cent of those with medically unexplained symptoms, which can include persistent pain, have mental health co-morbidities2.
“IAPT provides an integrated approach to treating common mental health problems for people who also have a LTC,” says Macdonald. “Treating the mental health aspects helps people to do better physically, improving quality of life and reducing healthcare service use.
“Patients who are empowered in self-management of chronic pain tend to do well independently of whether or not the chronic pain has a known cause. Including mental health as part of this holistic approach and treating appropriately issues such as depression or anxiety disorders also improves outcomes.
“People tend to do less well when the impact on the individual and those around them is not considered or where a healthcare professional takes a traditional ‘acute medicine’ approach, which may not make best use of the available evidence.
“The structure of services can mean that people with chronic pain, particularly those without a clear diagnosis, end up on a ‘journey’ around various hospital departments before eventually having a psychiatric or psychological assessment,” Macdonald adds.
“The patient may undergo investigations and treatments that aren’t indicated, or which aren’t necessarily helpful, then end up feeling that the hospital is suggesting that the pain ‘is all in the mind’.”
On the other hand, people with a history of mental health problems are more likely to be rapidly offered a psychological approach to help manage chronic pain but, Helen Macdonald notes, this may be at the expense of a robust diagnostic work-up, so clinicians may miss physical causes for chronic pain.
In addition, some doctors may dismiss aches and pains in, for instance, an obese patient as the result of excess weight and miss a more serious disease, such as a cancer – so-called diagnostic overshadowing.
Expanding the multidisciplinary team is one way to help improve pain management. “Advanced physiotherapy practitioners undertake many of our pain management unit assessments,” Lee Wilson says. “They also lead our pain management programmes, which help patients understand, manage and live with their pain, with limited nursing and pharmacy input.”
Specialist pain pharmacists can support their community colleagues by education and developing guidelines covering, for example, neuropathic pain, says Wilson. These guidelines can address local issues.
Doncaster and Bassetlaw, for example, prescribes large amounts of pregabalin. “We think our large local prison population may be a major contributor, but it can’t be the whole story,” he says. One approach being discussed locally is using amitriptyline as the first-line treatment for neuropathic pain, followed by gabapentinoids or referral to the pain management unit.
If we mention prescribing concerns regarding NSAIDs, we’ve nearly wiped out the World Health Organization analgesic ladder
Weak evidence
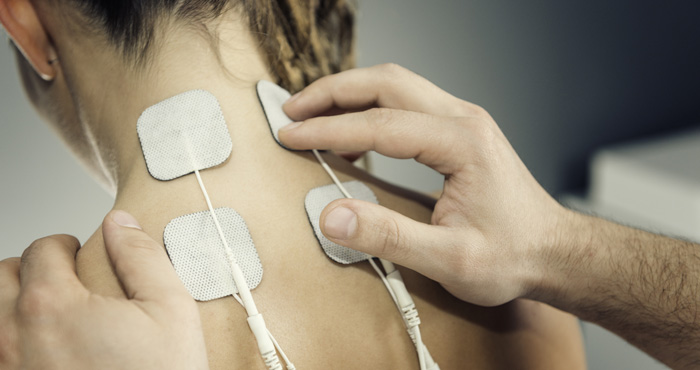
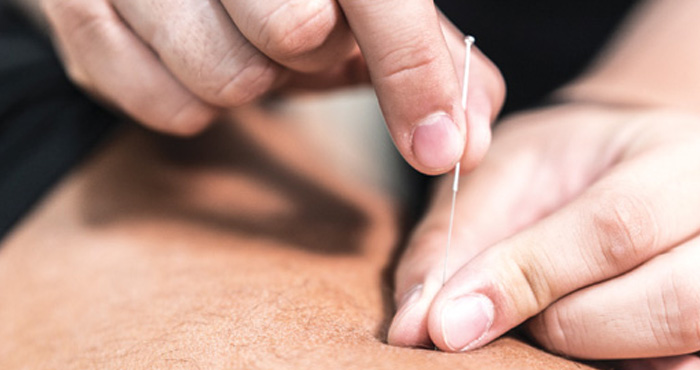
Multidisciplinary team involvement is especially important as a variety of treatments – including physiotherapy, CBT, transcutaneous electrical nerve stimulation (TENS) and acupuncture – may help selected chronic pain patients. For example, a meta-analysis of 31 studies involving 17,922 patients reported that acupuncture roughly halved the intensity of chronic pain caused by back, neck and shoulder problems, osteoarthritis and headache3.
In general, systemic reviews and meta-analyses conclude that acupuncture is significantly better than ‘sham acupuncture’ and standard care for some types of chronic pain. Acupuncture’s benefits can last up to six to 12 months and seems to be less likely to cause adverse events than many medical treatments. The most common complications are bruising or bleeding where the needle is inserted and a transient vasovagal response,4 which can cause dizziness, visual disturbances and blackouts.
Performing studies robust enough to convince commissioners can be difficult, however. TENS’s benefits, for example, are biologically plausible. A parent who rubs a sore area alleviates their child’s discomfort in part by activating non-nociceptive nerves that inhibit the nociceptive response in the dorsal horn in the spinal cord. TENS stimulates non-nociceptive fibres to inhibit pain, possibly by modulating levels of adenosine and endogenous opioids in the CNS,5 but showing that TENS is clinically valuable is difficult.
“How can TENS be tested in placebo-controlled trials when the intensity of the signal is supposed to build up to a certain level? ‘Sham TENS’ is often used, but the low voltage is not a conventional placebo,” says Lee Wilson.
Interventions with weak evidence bases are vulnerable to decommissioning, which might leave patients in chronic pain no option but to use analgesics. “Anecdotally, I’ve heard that some patients previously well controlled with acupuncture are now escalating opioids in primary care,” Wilson comments.
“NICE guidance has ‘downgraded’ acupuncture, but the evidence supports using it in certain circumstances,” Helen Macdonald adds. “I think, however, this may be the rationale for CCGs reducing funding.”
On the other hand, analgesics are not supported by especially robust evidence in chronic pain either. For instance, an editorial in the European Journal of Hospital Pharmacy reported that doses of up to 4,000mg paracetamol daily are “ineffective in back pain” and have “little chance of achieving clinically meaningful benefit in osteoarthritis”.
The authors found no evidence from reviews that paracetamol alleviates dysmenorrhoea, neck pain, rheumatoid arthritis or cancer pain. Paracetamol may, however, cause complications, particularly at higher doses, including increased mortality, cardiovascular and gastrointestinal adverse events, acute hepatic failure and abnormal liver function tests6.
Meanwhile, NICE warns of the “long-standing and well-recognised gastrointestinal and renal safety concerns with all NSAIDs”. NICE also highlights the “substantial evidence confirming an increased risk of cardiovascular events with many NSAIDs, including COX-2 inhibitors and some traditional NSAIDs, such as diclofenac and high-dose ibuprofen”7.
“If we mention prescribing concerns regarding NSAIDs, we’ve nearly wiped out the World Health Organization analgesic ladder,” Lee Wilson notes. “Considering the issues regarding lack of evidence for opioids and paracetamol in the long-term, this leaves a large field with a poor evidence base and practitioners with few tools at their disposal. We need more high-quality research across the board.”
“These analgesics have very high ‘face validity’ among the general population, which may make it harder for individuals to accept that they have little benefit – especially as there may be perceived to be few alternatives,” Helen Macdonald adds.
Key facts
- Chronic pain is generally regarded as pain that lasts for more than three months
- Prescribers frequently fail to undertake any meaningful review of analgesic effectiveness
- Improving pain management means looking beyond prescription medication
Psychological approach
In 1976, the American psychiatrist Aaron Beck suggested that events do not directly cause anxiety, depression and other emotional problems. Rather, our interpretation determines whether we develop anxiety, depression or another psychiatric problem. For instance, when we are depressed or anxious, we may interpret a minor difficulty as ‘proof’ things are getting worse. Negative emotions and expectations feed off each other. Beck’s theory forms the foundation of CBT, which is an important element in multidisciplinary chronic pain management.
“CBT addresses unhelpful beliefs and behaviours, which is why it can be particularly helpful for chronic pain. CBT can help people to live well with pain and to enhance quality of life despite the physical discomfort,” says Helen Macdonald. “CBT may treat a concurrent mental health diagnosis, such as depression or post-traumatic stress disorder, or specifically help someone to manage their pain better.”
CBT for chronic pain often includes shifting the focus from trying to reduce nociception to dealing with pain’s impact on the person and those around them, says Macdonald. “This will promote a holistic approach that hopefully helps the person with pain feel more empowered to deal with their symptoms,” she says.
Community pharmacists can help prevent the start of opioid escalation
“Pain is more likely to become chronic when someone is very distressed by their symptoms and believes that they are unable to manage the pain, or that passive treatments or someone else treating them, rather than self-management, is going to work best.”
CBT for chronic pain tends to cover activity management and relaxation, coping strategies (such as problem-solving, motivation and dealing with low mood and anxiety), overcoming avoidance, getting better sleep, working with significant others and carers, and overcoming setbacks.
“Considerable research suggests that people who learn to live a valued life, and accept that they will live with pain, do better than those who ‘fight’ and try to find a ‘cure’ for their chronic pain,” says Macdonald. “Reaching a place of acceptance supports self-management of chronic pain.”
CBT can also help the person engage and stay motivated during physiotherapy, such as by overcoming the patient’s fear and avoidance of certain types of movement. “CBT can be very useful to help people manage activity and rest, without becoming de-conditioned, and without ‘overdoing it’,” Macdonald says.
Unfortunately, many people can’t access the help they need. “We need to investigate waiting times to see a CBT practitioner specifically for chronic pain,” she points out. “I suspect, however, that the wait is likely to be longer for CBT for pain management than for other indications, and even longer in Wales, Scotland and Northern Ireland where access to psychological therapies generally is even worse.”
Opioid scripts
Between 1998 and 2016, the number of opioid prescriptions increased by 34 per cent from 568 to 761 per 1,000 of the population in England. Based on total oral morphine equivalency, however, prescribing more than doubled (127 per cent increase) from 190,000mg to 431,000mg per 1,000 of the population.
The volume of high-dose (120mg or greater morphine equivalency) long-acting opioid prescriptions increased almost six-fold (581 per cent increase) from three to 23 per 1,000 of the population during this time. Based on total oral morphine equivalency, prescribing rose five-fold (457 per cent increase) from 17,800mg to 99,300mg per 1,000 of the population. Prescriptions declined from 2016 to 2017, largely due to less morphine use.
Bridging the gap
While patients wait for specialist support, community pharmacists can advise patients about pacing and rehabilitation, echoing messages that they may have received during a pain management programme, Lee Wilson suggests.
In addition, pharmacists can signpost patients to local services and highlight potential opioid abuse to GPs. “Suggesting that people get a referral to the local integrated IAPT service is probably the most useful signpost for patients in chronic pain,” Helen Macdonald suggests.
Pharmacists can also advise patients to learn relaxation techniques, she adds. The relaxation response may alleviate chronic pain by reducing sympathetic activity, muscular tension and awareness of pain, while increasing the release of endogenous opioids4. Community pharmacists should watch for and refer people with depression, anxiety or both, which often accompany chronic pain, she says.
Until NHS services for chronic pain improve, community pharmacists will remain in the vanguard of pain management – not necessarily by reaching for an OTC analgesic, but by helping each patient access the support that meets their needs.
“Community pharmacists can help prevent the start of the opioid escalation, which often begins with co-codamol 8/500, which is paracetamol with the added bonus of constipation,” Lee Wilson remarks. “It may be surprising to hear this from a pharmacist, but the management of persistent or chronic pain is moving away from medications.”
Further sources of information for patients and pharmacists
- BABCP
- Reading Well initiative for people with long-term conditions (including chronic pain)
- Live Well With Pain
- Opioids Aware guidance
- The Pain Toolkit
References
- BMJ Open 2016; 6:DOI: 10.1136/bmjopen-2015-010364
- Available at NHS England
- Archives of Internal Medicine 2012; 172:1444-1453
- BMJ 2017; 357:j1284
- Evidence-Based Complementary and Alternative Medicine 2015; 2015:8
- European Journal of Hospital Pharmacy 2016; 23:187-188
- Available at NICE
- The Lancet Psychiatry 2019; 6:140-150
