In Clinical
Follow this topic
Bookmark
Record learning outcomes
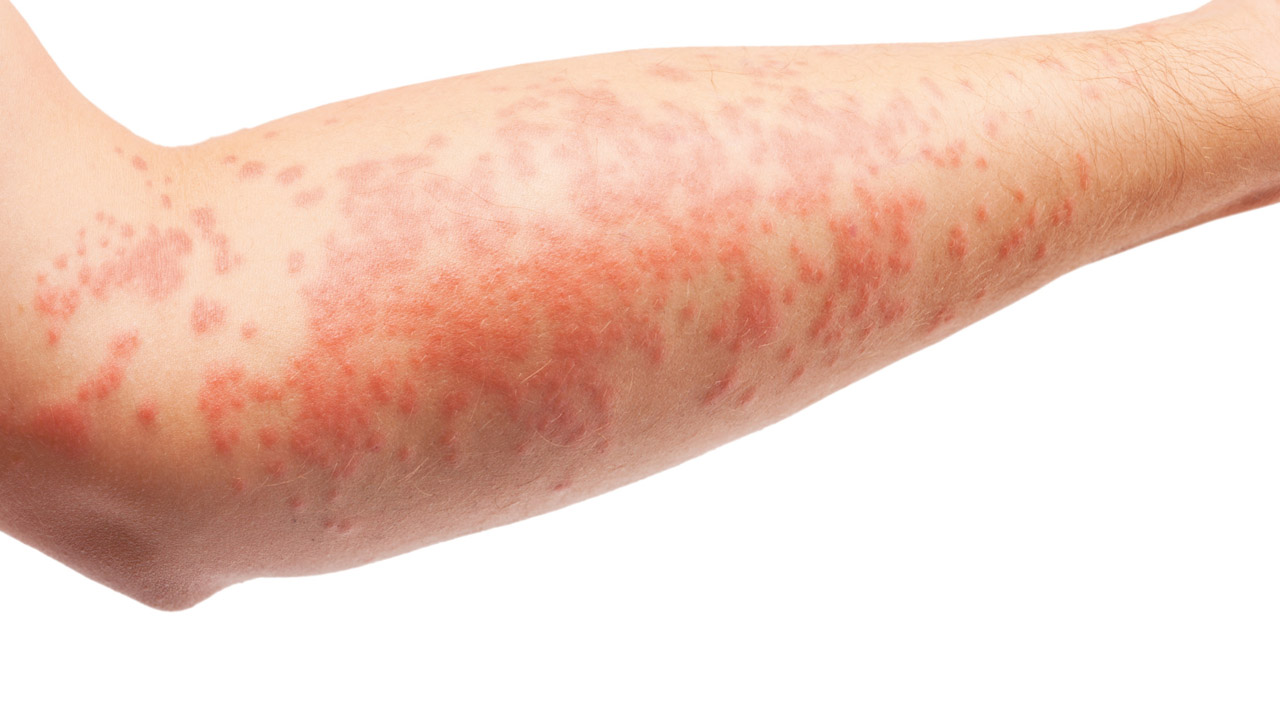
Atopic dermatitis (AD) is one of the most common diseases seen by community pharmacists. Up to 20 per cent of children and 10 per cent of adults in high-income countries have eczema.1
Apart from the often considerable distress caused by visible eczema, AD is linked to numerous comorbidities, such as food allergy, asthma, allergic rhinitis, mental health problems1 and, according to a new study, even venous thromboembolism (VTE).
Several studies highlighted the plethora of mental and physical comorbidities experienced by AD patients. A Dutch study, for example, reported that people with AD were prone to psychiatric comorbidities such as chronic fatigue syndrome, burnout, depression, social phobia, attention deficit hyperactivity disorder, eating disorder, and panic and other anxiety issues.
Research round-up
- A French study found that 20 per cent of female atopic dermatitis patients always or often experienced AD exacerbations a few days before menstruation
- A UK study has found that AD patients are 17 per cent more likely to develop venous thromboembolism than controls
- A meta-analysis of 557 articles found that AD increased the risk of food sensitivity, challenge-proven food allergy and food allergy about four- to five-fold
Link with mental disorders
Patient with atopic dermatitis were more likely to experience loneliness than those without the condition. Loneliness and increasing AD severity strengthened the association between AD and mental disorders.
Food allergies are also common co-morbidities. While certain foods can exacerbate AD, food sensitivity and food allergy can develop after the skin is exposed to food allergens. Poor skin barrier function, a hallmark of AD, can enhance the skin’s reaction to food allergens.
A meta-analysis of 557 articles found that 48.4 per cent of AD patients had food sensitivity, 40.7 per cent challenge-proven food allergy (CPFA) and 32.7 per cent food allergy. Overall, AD increased the risk of food sensitivity, CPFA and food allergy about four- to five-fold.
Children with AD were more likely than adults with eczema to show food sensitivity (49.8 and 28.6 per cent respectively) and food allergy (31.4 and 24.1 per cent respectively). Looking at the relationship the other way, children and adults with food sensitivity (OR 3.92), CPFA (OR 4.93) and food allergy (OR 4.06) were about four times more likely than controls to have AD. In other words, the conditions are intimately intertwined.
The authors remark that healthcare professionals “should be aware of the strong bidirectional relationship to optimise management and treatment of these patients”. They add that, “whether food avoidance in AD individuals could improve their AD and the most [effective] preventative actions remain unknown”.
The comorbidities of AD are more than psychiatric, atopic and dermatological. A UK study used general practice records to match 150,975 AD patients to 603,770 controls. After adjusting for confounders, AD patients were 17 per cent more likely to develop VTE than controls. It was also associated with a 30 per cent increased risk of deep vein thrombosis. The risk of pulmonary thromboembolism did not differ significantly between AD patients and controls.
VTE risk was higher among people with severe AD (32 per cent increased risk) than moderate AD (12 per cent increased risk), people aged 65 years and older (22 per cent increased risk) and those who are obese (25 per cent increased risk). The results were consistent after excluding people with a history of VTE or other inflammatory conditions; VTE risk did not differ between sexes or in females taking hormone treatment.
“Understanding why AD associates with an increased risk of VTE is vital for future research, and knowledge of this increased VTE risk, as well as the subgroups with the highest risk, are important for dermatologists treating AD,” the authors conclude.
“Atopic dermatitis and food allergy and sensitivity are intimately intertwined”
Asthma update
Asthma sufferers at risk from cost-of-living crisis
Asthma + Lung UK has warned that many of the 5.4 million people in the UK with asthma could be at risk as living costs soar and winter bites.
Around one in five people with asthma surveyed by the charity say that the soaring cost of living has caused life-threatening asthma attacks as they cut back on medicines, heating and food.
The charity, which surveyed more than 3,600 people with lung conditions such as asthma, COPD and bronchiectasis, also found that one in two felt their condition had worsened since the cost-of-living crisis began, with many needing emergency treatment.
Almost one in six respondents (15 per cent) said they were cutting back on using their inhaler to make it last longer, even though using a preventer inhaler every day is the best way to manage asthma and prevent attacks. One in 10 said they had been using medical devices (e.g. nebulisers) that require electricity less often.
Asthma + Lung UK warns that with winter already the deadliest season for people with lung conditions, there could be a tidal wave of hospital admissions as cold weather, an abundance of viruses and people cutting back on medicines, heating, food and electricity puts them at risk.
Uncontrolled severe asthma “a huge burden”
Uncontrolled severe asthma imposes a “huge burden … in terms of mortality, morbidity and healthcare resource consumption compared with other patients with asthma and with the general population”, a new study concludes.
French researchers used medical records to identify 16,588 asthma patients aged at least 12 years. The mean age was 62.0 years and 4.5 per cent had uncontrolled severe asthma. During the two-year follow-up, those with uncontrolled severe asthma were more than twice as likely to die (relative risk 2.35) as general population controls without asthma: 92.0 and 96.6 per cent respectively were alive at two years.
Mortality was 18.0-fold higher among patients with uncontrolled severe asthma aged 50 to 60 years old and 4.1-fold higher in those aged 60 to 70 years old than the general population. Emergency department visits and hospitalisations were significantly higher in patients with uncontrolled severe asthma (64.7 per cent) than the general population (34.9 per cent) and asthma (55.2 per cent) controls.
Average healthcare costs of uncontrolled severe asthma during the two years were almost four times higher than the general population and double that in asthma controls. (BMJ Open 2022; 12:e060160)
Ineffective treatments
Over the years, numerous studies have highlighted that many AD patients do not receive the most effective available treatments. For example, a survey interviewed 2,005 people with AD from eight countries including the UK. Ninety-two per cent had mild-to-moderate AD (less than 10 per cent of body surface area affected).
Fifty-six per cent of people with AD experienced moderate-to-severe itching in the past week. Indeed, itch was the most common reason AD patients sought advice (61 per cent), followed by skin appearance and visible rash (57 per cent), pain (30 per cent) and difficulties with daily and social activities, such as school, work and relationships (23 per cent).
Perhaps not surprisingly, people with mild-to-moderate AD were less likely to have seen a healthcare professional because of their AD in the past year than those with severe AD (67 and 82 per cent respectively). Patients with mild-to-moderate AD were also less likely to report that their healthcare professional involved them always or usually in decisions about treatment than those with severe AD (73 and 86 per cent).
As expected, most participants with mild-to-moderate AD used topical treatments (45-56 per cent). Patients with severe AD were more likely to use systemic treatments, including oral treatments (46-54 per cent), injectables (43 per cent) and phototherapy (37 per cent). Participants with mild-to-moderate AD reported lower treatment satisfaction, regardless of interventions, than people with severe AD.
In particular, fewer than half of people with mild-to-moderate AD were satisfied with the ability of topical treatments to alleviate itch. “The findings of this survey emphasise a need for improvements in treatments for patients with mild-to-moderate AD, with a specific need for effective anti-pruritic therapies,” the authors conclude.
These and other studies presented during the EADV congress highlight how AD can cause considerable distress and that the comorbidities are more than just atopic and dermatological. Community pharmacists should offer effective treatments and refer when appropriate to help people with AD get the help they need.
It may be one of the most common diseases pharmacists encounter, but there is still much to learn. We’ve only scratched the surface.
Reference
1. The Lancet 2020; 396:345-360
Do hormonal fluctuations have an effect?
Research presented during the EADV congress reported that hormonal fluctuations affect the location, extent and appearance of AD.
A French study found that 20 per cent of female AD patients always or often experienced exacerbations a few days before menstruation. Another 31 per cent occasionally reported pre-menstrual eczema exacerbations. Forty per cent reported exacerbations a few days after menstruation.
A similar proportion (41 per cent) felt that hormonal variations affected their eczema. Of those experiencing hormonal fluctuations in eczema, 61 per cent reported a change in the extent of AD, 39 per cent a change in appearance and 23 per cent a change in lesion location.
Overall, 10.3 per cent of women with eczema said that AD left them afraid of pregnancy. Of these, 55 per cent said that their eczema affected their desire to have children and 42 per cent had delayed pregnancy because of their AD.
Another study followed 87 pre-menopausal women from Italy with moderate-to-severe AD for three months. The Eczema Area and Severity Index (EASI) score worsened by a mean of 17.7 per cent in the pre-menstrual period. In addition, itch worsened by a mean of 35.3 per cent and quality of life scores deteriorated by 26.3 per cent pre-menstrually.
Pre-menstrual dysphoric disorder or moderate-to-severe PMS did not seem to influence pre-menstrual AD exacerbations. “These aspects deserve attention for more comprehensive patient management in everyday practice and in patients recruited in trials evaluating new treatment options,” the authors concluded.