Reflecting on foot care
In Clinical
Follow this topic
Bookmark
Record learning outcomes
The Covid-19 pandemic has led to a surge in cases of advanced foot disease being reported by hospitals in the UK, triggering renewed calls for people with diabetes not to delay seeking medical attention if they experience any problems with their feet
Learning objectives
After reading this feature you should be able to:
- Appreciate the impact the Covid-19 pandemic has had on the incidence of serious feet and leg complications
- Recognise the danger signs of foot disease among diabetic patients and educate them on good foot/leg health
- Provide advice on the treatment and self-care of common foot and leg problems.
Hesitancy in seeking help has been fuelled by reluctance to enter healthcare settings for fear of catching coronavirus, as well as confusion about which routine diabetes services are still available during the pandemic and how to access them.
According to Diabetes UK, these delays have led to a direct increase in the incidence of people presenting at hospitals with foot problems who need to go straight to surgical admission and major amputation because their condition is so severe.1
Pharmacy teams can help to tackle this burgeoning health emergency by addressing reticence among patients and encouraging them to seek medical attention for foot problems where needed. It is important to reinforce the key message to people with diabetes that they have not been forgotten and that the NHS is open and available to them for help with diabetic foot problems and any other disease-related complication.
“As we continue to navigate the challenges of the pandemic and while vital services remain under immense pressure, we must not forget that serious conditions like diabetes cannot be put on hold,” says Chris Askew, chief executive of Diabetes UK. “Without action, people with diabetes will – unnecessarily – continue to be at increased risk of serious and life-altering complications.”2
Key facts
- More people are presenting at hospital with advanced foot disease due to delays in accessing care
- People with diabetes are at particularly high risk of disease-related foot complications
- Pharmacy can play an important role in helping customers manage everyday foot and leg health issues
Diabetes and foot health
The link between diabetes and foot health problems is well established. High blood glucose levels caused by diabetes can impede blood flow to the feet and also damage nerves, resulting in loss of sensation. As a result, people with diabetes may not be able to feel injury to their feet or sense extremes of temperature.
An estimated 20 per cent of people living with diabetes are at higher risk of developing these diabetic foot care problems which, if not properly identified and treated, can lead to serious sequelae such as foot ulceration and even amputation.2
Pharmacy teams can help raise awareness of the importance of good foot and leg care among patients with diabetes by explaining the causes of diabetic foot disease, emphasising the real risk of developing these problems and highlighting the potentially serious – but preventable – consequences.
Around one in 10 people with diabetes will develop a foot ulcer at some point in their lives and, left untreated, these ulcers are the key drivers of ensuing amputation.2,3 Of the 140 leg, foot and toe amputations performed each week in the UK, the vast majority (80 per cent) result from ulcers that could have been prevented or treated at an earlier stage.2,3
Diabetes UK advocates 10 simple steps to preventing diabetic foot problems:3
- Stop smoking. Smoking impairs circulation in the extremities, which can seriously worsen foot and leg problems in people with diabetes
- Manage blood sugar levels, cholesterol and blood pressure. Keeping blood glucose under control is the single most important weapon in the fight against diabetes complications, including foot problems. Patients should be encouraged to follow the advice of their diabetes care team on glucose monitoring and ensure medications are taken as directed. In this regard, pharmacy teams can play a key role in helping bolster adherence and aiding patients in navigating the complexities of the diabetes treatment pathway
- Check feet daily as, left undetected, diabetic foot problems can quickly escalate. In a person with diabetes, any foot injury which fails to heal – even one as simple as a blister – is a reason to see a GP. Customers should also be advised to look out for changes to their feet such as breaks in the skin, especially if accompanied by discharge, changes in the colour of the skin on the foot or any swelling or redness. If any of these signs are noted, then medical attention should be sought immediately
- Eat a healthy balanced diet and exercise regularly. This can help reduce the risk of diabetic foot problems and is also a key pillar of overall diabetes management
- Cut or file toenails regularly but take care to avoid piercing the skin
- Apply emollient cream to the feet daily to keep the skin on the feet moisturised and healthy (healthy skin provides a more effective barrier to infection) but avoid the area between the toes
- Wear well-fitting shoes that don’t squeeze or rub the feet and avoid going barefoot, especially when outdoors
- See a foot specialist for the treatment of common foot ailments such as corns or hard skin and do not attempt self-care
- Ensure feet are checked over each year as part of the annual diabetes review
- Know who to call and where to seek help if/when a foot problem arises.
Free risk assessment tool with this issue
With medical studies showing that neuro-pathic pre-ulcerative calluses precede 80 per cent of foot ulcerations in patients with diabetes, Dermatonics has produced a risk assessment tool.
The handy card, included as an insert in this issue, highlights six steps starting with making an initial assessment, assessing the level of foot health and additional risk factors to explaining the link between pre-ulcerative callus and ulceration, the risks of diabetic foot disease and treatment.
Increase your footfall
In addition to providing specific advice and support to patients with diabetes, pharmacy teams can also help other customers deal with everyday leg and foot health issues that commonly present in a community pharmacy setting.
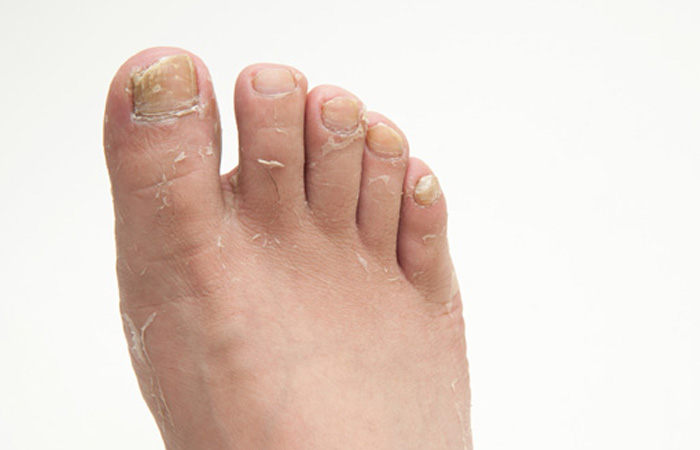
Athlete’s foot
Athlete’s foot typically targets the space between the fourth and fifth toe, causing itchy, red skin that may later become white, inflamed and weepy. Left untreated, the causative tinea pedis fungus can spread to other areas of the foot and the toenails, leading to a fungal nail infection.
Regular application of tea tree oil between the toes can help prevent athlete’s foot from developing, while a range of OTC antifungal foot products are available for those with an active infection.
Athlete’s foot products are available as sprays, creams and solutions that contain either fungistatic agents such as clotrimazole or miconazole or the fungicidal drug terbinafine. Most products require repeated application over a period of a week or more to completely clear the infection, but terbinafine is also available as a single-dose treatment.
Key preventative steps to reduce the risk of future episodes of athlete’s foot and ensuing fungal nail infections include avoiding going barefoot in damp places (particularly communal changing rooms/showers), keeping feet dry and clean, and wearing breathable footwear.
Varicose veins
Varicose veins are swollen, twisted veins in the leg that lie just under the skin’s surface. They result from weakness or damage to the small valves inside the leg veins, which allows blood to flow backwards and collect in the veins, causing them to become swollen and enlarged.
Varicose veins are typified by bulging, lumpy veins on the legs and feet that appear blue or dark purple in colour. Accompanying symptoms can include sensations of aching, throbbing or heaviness in the legs, and dry, itchy skin over the affected vein.
Older age, pregnancy, being overweight, family history and having an occupation that involves long periods of standing are key risk factors for developing varicose veins. Treatment options range from lifestyle measures and compression therapy to medications and ablative/surgical procedures to remove the veins themselves.
Pharmacy staff are well positioned to advise on key self-care measures for varicose veins, which include maintaining a healthy weight, avoiding long periods of standing, elevating legs when seated (above the level of the heart) and keeping physically active. Compression stockings can also be recommended to help relieve symptoms such as pain, swelling and leg heaviness.
Aching legs
Tired and/or aching legs are a common everyday ailment but particularly affect those with jobs that require standing for long periods of time. Other key risk factors include being obese or overweight, pregnancy and – counterintuitively – having a very sedentary lifestyle.
Simple analgesics can be recommended to lessen discomfort associated with aching legs and several creams, balms and serums aimed at relieving feelings of tiredness and heaviness in the legs are also available to buy.
Customers should also be advised to elevate legs when sitting and can consider wearing compression hosiery to boost blood flow to the legs. Losing weight and staying active help reduce episodes of tired and achy lower limbs, although it is important to avoid over-exercise, which can exacerbate the problem.
In some cases, throbbing or painful legs can be an early harbinger of venous hypertension or insufficiency, so customers with prolonged or severe leg pain should be encouraged to consult their GP for further tests. Cramping pain (claudication) that develops in the leg muscles with exercise and resolves with rest is indicative of underlying atherosclerosis, so also warrants further medical investigation.
Deep vein thrombosis
A deep vein thrombosis (DVT) is a blood clot that develops in one of the deep veins in the legs, leading to a partial or complete blockage. The most common site for a DVT to develop is the calf, although the thigh vein can sometimes be affected. Immobility is the key cause of DVT, particularly during or after surgery, because it is movement of the leg muscles that helps to push blood along the veins. However, other important risk factors to be aware of include cancer or heart failure, oral contraceptives and HRT, older age, pregnancy, obesity and dehydration.
The hallmark signs and symptoms of DVT are persistent pain, tenderness and swelling of the calf, which may also look red and feel warm to the touch. Any customer with suspected DVT should be encouraged to seek urgent medical attention as serious complications such as pulmonary embolism can occur if part of the clot breaks off and enters the bloodstream.
Treatment options include anticoagulants and compression stockings. To reduce the future risk of DVT, patients – particularly those with risk factors – should be encouraged to keep active and hydrated and avoid long periods of immobility.
Blisters
Blisters develop when the skin becomes damaged and act as the body’s own self-generated protective cushion against further injury. Blisters on the feet are typically caused by friction from poorly-fitting shoes and appear as small pockets of clear fluid under a layer of skin.
The key step in dealing with blisters is to cover and protect the affected area to avoid further damage and allow healing. Numerous blister plasters and dressings are available in a range of sizes and shapes. Hydrocolloid dressings have the additional advantage of creating an optimised moist wound healing environment that reduces pain and accelerates healing.
Blisters which show signs of infection, such as redness or warmth in the surrounding skin or exudation of pus, may require antibiotics due to the risk of skin or blood infections, and customers should be referred to their GP accordingly.
To prevent blisters from developing in the first place, it is important to wear comfortable, well-fitting shoes, ‘break in’ new footwear before use and wear thick socks during exercise.
Corns and calluses
Corns are caused by pressure or rubbing from overly tight shoes that leads to small cone-shaped areas of thickened skin. Hard corns are layers of thick, dead skin that build up on the toe surface. They contain a packed centre with the tip pointing inwards, pressing on nerve ends in the foot and causing pain. In contrast, soft corns are white and rubbery in texture and appear between the toes themselves.
Calluses are areas of hard dry skin caused by pressure or friction on the bony parts of the feet, so typically affect the ball of the foot, the outside of the big toe and side of the heels. They cause a generalised burning sensation rather than the localised pain of corns.
Salicylic acid, usually applied as a medicated plaster or cap, is the cornerstone of treatment for both corns and calluses, and works by removing the excess layers of hard skin. Corn/callus removal pens are also available containing trichloroacetic acid (TCA), which is applied to the affected area as a gel.
Cushioning products can also be recommended to help relieve pressure, ease pain and stop the problem from recurring. Regular use of foot files, pumice stones and moisturising creams can help to prevent future build-up of hard skin.
Bunions
Bunions are caused by a slow dislocation of the big toe joint.4 Bunions can be hereditary so hard to prevent but key self-care steps for sufferers include avoiding high heels or pointed-toe shoes, which can exacerbate the problem. Bunion pain can be relieved with non-medicated bunion pads and plasters, while bunion protectors are available to purchase OTC to help to protect the affected area and absorb friction on the bunion.
Surgery is the only definitive cure for bunions but, to help correct the underlying deviation and relieve pain, customers can also try flexible bunion correctors, which are worn inside the shoe and act to push the toe back into alignment.
Chilblains
Chilblains are small, red and itchy patches of swollen skin that appear on the toes and feet after exposure to the cold. They are thought to arise due to an abnormal reaction to cold temperatures, likely due to poor circulation. Chilblains typically heal on their own within a week or so but it is important to keep the affected area warm and away from direct heat.
Simple oral analgesics such as paracetamol or ibuprofen can help manage any pain, while soothing creams like calamine may provide relief from symptoms such as itching or burning.
Warts and verrucae
Both warts and verrucae are caused by infection with the human papilloma virus (HPV), which triggers excess keratin production in the top layer of the skin. In other words, a verruca is simply a wart that occurs on the sole of the foot, appearing as a flat, round lump peppered with one or more black spots.
Treatment options include topical liquid or gel formulations of acids such as salicylic acid or TCA (available as creams, plasters, sprays and pens) or ‘freeze’ treatments that contain gases which work by rapidly freezing the core of the verruca. Both acid foot products and freezing sprays offer 70-75 per cent success in treating verrucae but may take time to work and often need to be repeated.
Customers can be reassured that, even without treatment, all verrucae will eventually heal with time – however this can be a protracted process lasting up to two years and hinges on the strength of the immune system (healing may take longer in immunocompromised individuals). To avoid spreading a verruca (or catching one in future), advise customers to wear flip-flops in communal showers, not to share foot products or shoes/socks and cover the affected area when swimming.
The dreaded sweaty feet...
The feet contain more sweat glands per inch than any other part of the body – over a quarter of a million – so sweaty feet and associated odour are a common issue.5
Maintaining a rigorous foot hygiene regimen is essential for combatting sweaty feet. Feet should be washed daily in warm water, dried thoroughly and talcum powder applied after cleansing to help absorb sweat and dry out/freshen them.
Customers should opt for well-fitting shoes made of breathable materials (e.g. leather) and moisture-absorbing socks made of natural fibres such as cotton or wool. If odour is a problem, antibacterial emollient washes can be used as part of the daily foot hygiene routine.
Pharmacy teams can also recommend odour-neutralising foot antiperspirants containing aluminium chloride and/or medicated, deodourising insoles.
