In Clinical
Follow this topic
Bookmark
Record learning outcomes
Cases of monkeypox have now been reported in multiple countries that do not have endemic monkeypox virus in animal or human populations, including countries in Europe, North America and Australasia.
These cases have no history of travel to areas where the virus is endemic, suggesting that person-to-person transmission is occurring.
FAQS
Monkeypox is a very rare infectious disease caused by the monkeypox virus. It was first isolated from monkeys in 1958. The first known human case was diagnosed in 1970 in the Democratic Republic of the Congo (DRC). Since then, monkeypox has become endemic in central and western African countries.
NB: rodents, such as rats and squirrels, can also carry the virus. A 2003 outbreak in the US was traced to rodents imported as pets from Ghana.
Some infectious disease experts believe that the disease was held in check when smallpox vaccination was common but since the eradication of smallpox (and discontinuation of routine vaccination) cases of monkeypox have risen.
Monkeypox is a zoonotic virus that is typically transmitted through close contact between an animal and human, often through a bite, scratch, or contact with the rash and with fomites (objects e.g. bedding contaminated with material from monkeypox lesions). Person-to-person transmission is believed to occur through direct contact with lesions, body fluids, respiratory droplets or fomites.
People may be contagious at the early signs of fever and stay infectious through the rash until the skin scabs and heals over.
There are two clades of monkeypox – a Central African clade with a reported mortality rate of 10 per cent and a West African clade with a reported mortality of 1 per cent from epidemiological cluster and outbreak reports from Africa. In the UK, so far, all reported cases have been identified as the West African clade.
The disease in healthy adults is primarily self-limiting and with a relatively low mortality. There is remaining uncertainty over potentially increased severity in children and in individuals who are immunocompromised or pregnant.
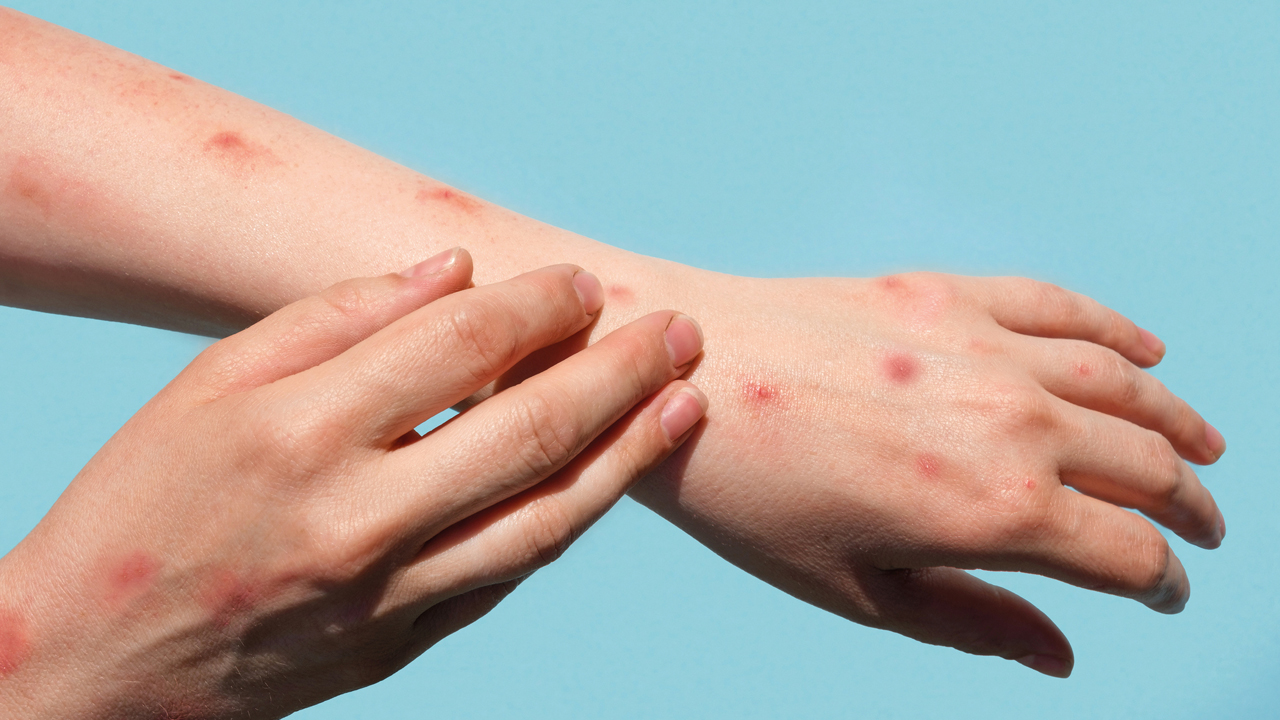
Monkeypox starts with fever, then general body aches, malaise, and muscle aches and swollen lymph nodes. These are followed by the development of a rash. It starts as macules (flat lesions) that progress to form nodules, then blisters and pustules that eventually scab over and heal. On occasions, the rash has been confused with chickenpox. The incubation period is usually seven to 14 days.
Like the smallpox and cowpox viruses, the monkeypox virus is part of the Orthopox virus genus. Monkeypox is not related to chickenpox.
The UK Government has issued guidance (for healthcare professionals) designed to suppress transmission of monkeypox in the community with the ultimate aim of eradicating the disease.
The guidance (Principles for monkeypox control in the UK: 4 nations consensus statement) also emphasises measures to prevent the disease from spreading in hospitals and healthcare settings and to healthcare workers.
Previous vaccination against smallpox provides a degree of cross-protection. Pre- and post-exposure prophylaxis with smallpox vaccine (MVA-BN [Imvanex]) is available and will be used on a risk-assessed basis.
The recommendations and risk categories are set out in guidance from the UKHSA. As the vaccine does not have a marketing authorisation for protection against monkeypox in Europe, its use would be considered ‘off label’.
A recent analysis of seven previous cases of monkeypox in the UK noted that the antiviral tecovirimat might shorten the duration of monkeypox symptoms and reduce the length of time a patient is contagious.
Gay men and men who have sex with men (MSM) may not actually be disproportionately affected – it may just be an unlucky conjunction of circumstances. Sexual health clinics were alerted by the UKHSA and the British Association for Sexual Health and HIV on May 16 to possible community transmission of monkeypox virus among MSM. It followed inquiries into four linked cases who all identified as gay, bisexual or other MSM.