Oral health: Could it be cancer?
In Clinical
Follow this topic
Bookmark
Record learning outcomes
Mouth cancer claims far more lives than cervical or testicular cancer, yet worryingly one in five people remain unaware of this deadly disease. How can community pharmacists raise awareness?

Learning objectives
After reading this feature you should be able to:
- Explain the prevalence of mouth cancer and identify the risk factors
- Be aware of the major signs of mouth cancer and advise patients about checking for the disease
- Manage common oral health problems with advice and OTC product recommendation
Awareness of oral cancer is far too low in the UK and this needs to change, says Dr Nigel Carter, chief executive officer of the Oral Health Foundation.
“Most people who develop mouth cancer will be older men with a history of smoking and drinking to excess,” he says, “but more younger people and women than ever before are developing the disease. This is being driven largely by behavioural choices and is where more awareness should be targeted because too many people think they are not at risk.”
According to Cancer Research UK:
- Men are more than twice as likely as women to develop oral cancer (including mouth cancer). One in 75 men and one in 150 women will be diagnosed with the disease
- Incidence rates for the disease are projected to rise by 33 per cent to 20 cases per 100,000 people by 2035
- While often seen as an ‘older man’s disease’, rates of oral cancer (especially tongue and tonsil cancers) are on the increase, particularly in people in their 40s, 50s and 60s
- Oral cancer is the eleventh commonest male cancer overall, but the fourth commonest among men aged 45 to 59 years.
Around one in five people in Britain has never heard of mouth cancer, says Dr Carter, and this is a figure that has hardly changed over the past decade. Worryingly, fewer men say they have heard of mouth cancer compared to women, even though men traditionally are more at risk, he says.
“Cases continue to rise and mouth cancer claims far more lives than some other forms of cancer such as cervical or testicular cancer – yet people remain unaware of the disease.”
Key facts
- Research suggests that smoking causes more than 60 per cent of mouth and throat cancers
- Around nine out of 10 oral cancer cases in the UK are linked to preventable causes like smoking and excessive alcohol consumption
- HPV could soon overtake smoking as the main cause
Risk factors
Oral cancer includes cancers of the mouth, tongue, lips, tonsils and middle part of the throat (oropharynx). Around nine out of 10 oral cancer cases in the UK are linked to preventable causes like smoking and excessive alcohol consumption. Over-exposure to sunlight can also increase the risk of cancer of the lips.
Research suggests that smoking causes more than 60 per cent of mouth and throat cancers in the UK and that giving up reduces the risk of mouth cancer by more than a third. At particular risk are those people who smoke and drink alcohol to excess, as this increases their chances of mouth cancer 30-fold. Even people exposed to passive smoking have an increased risk of the disease, while some traditional ethnic habits of chewing tobacco, betel quid, gutkha and paan also count as high risk factors.
A diet low in fruit and vegetables has been linked to over half of all mouth cancer cases. The latest National Diet and Nutrition Survey revealed that only 27 per cent of adults between 19 and 64 years of age, and 35 per cent of adults aged 65 years and over, meet the 5-a-day target for fruit and vegetables (it has been suggested this should be increased to 10-a-day).

Mouth Cancer Action says foods and supplements that may lower the risk of mouth cancer include fruit and vegetables, vitamin C and calcium supplements, caffeinated coffee and green tea.
The human papillomavirus virus (HPV) has been linked to oral cancer, as well as cancers of the cervix, anus, penis, vulva and vagina. It is transmitted mainly through oral sex. Most people will get HPV at some point in their lives and it generally doesn’t cause any symptoms. (To protect against cervical cancer, all girls can be vaccinated against HPV free on the NHS between the ages of 12 and 18 years. Most girls are usually offered the vaccine when they are in year eight at secondary school.)
The current vaccine, Gardasil, protects against HPV types 6, 11, 16 and 18. Types 16 and 18 are the cause of most cervical cancers in the UK – more than 70 per cent – and are also linked to cancers of the mouth and throat. (HPV types 6 and 11 cause nearly all cases of genital warts.)
Estimates of how many oral cancer cases are caused by HPV vary, but HPV infection is thought to be responsible for most cases in younger people. “As sexual behaviour has evolved over the past couple of decades, with more people having multiple partners, there has been a corresponding increase in cases of mouth cancer,” says Dr Carter.
“HPV is the major cause of cervical cancer and affects the skin that lines the moist areas of the body, such as inside the mouth. Research suggests it could soon overtake smoking as the main cause of mouth cancer in this country. One of the most effective ways pharmacy teams can advise customers about this is to let them know about the relationship between HPV and mouth cancer and raise the issue of HPV vaccination.”
Raising awareness
People should check for mouth cancer in the same way that they check for breast or testicular cancer, says Dr Carter. “After all, nobody bats an eyelid about checking for a lump in a breast or testicle and visiting a doctor about it,” he says.
“People need to be aware of the major signs of mouth cancer – red and white patches and ulcers that don’t heal within three weeks – and make sure they are regularly checking themselves.” (See panel on ‘Mouth cancer checks’.)
Early diagnosis transforms a person’s chances of beating the disease – from 50 to 90 per cent – so it is crucial that pharmacy teams know what to look out for. “It is important to encourage customers who have noticed any unusual or persistent changes to their mouth or neck to tell their doctor,” says Carl Alexander, spokesperson for Cancer Research UK.
“The key signs and symptoms include ulcers or sores that won’t heal and last longer than three weeks, an unexplained lump in the neck, a lump on the lips or in the mouth, or a red or redand- white patch in the mouth. If they notice anything unusual or persistent, that is when they should go to the doctor to get it checked out. It is most likely something less serious than cancer but, if it is cancer, an early diagnosis could make a big difference.”
Mouth cancer checks: what to do
The following mouth cancer checks can be recommended to customers and carried out at home. Ask about the following:
- Face: Look at the face and neck in the mirror: do both sides look the same? Look for any lumps, bumps or swellings that are only on one side of the face
- Neck: Feel and press along the sides and front of the neck. Can you feel tenderness or lumps?
- Lips: Pull down the lower lip and look inside for any sores or change in colour. Use your thumb and forefinger to feel the lip for lumps, bumps or changes in texture. Repeat this on the upper lip
- Cheek: Use a finger to pull out the cheek so that the inside is visible in a mirror. Look for red, white or dark patches. Put an index finger inside the cheek and thumb on the outside. Gently squeeze and roll the cheek to check for any lumps, tenderness or ulcers. Repeat on the other cheek
- Roof of the mouth: Tilt back the head and open the mouth wide to see if there are any lumps or if there is a change in colour visible. Run a finger along the roof of the mouth to feel for any lumps or ulcers
- Tongue: Stick out the tongue and look at the surface for any changes in colour and/or texture. Gently pull out the tongue and look at one side first, then the other side. Look for any swelling, change in colour or ulcers. Examine the underside of the tongue by placing the tip of the tongue on the roof of the mouth
- Floor of the mouth: Look at the floor of the mouth for changes in colour that are different to normal. Gently press a finger along the floor of the mouth and underside of the tongue to feel for any lumps, swellings or ulcers. Source: Oral Health Foundation
Pharmacy advice
One in 10 people turn to their pharmacist for advice if they have a mouth ulcer that doesn’t heal within a couple of weeks, says Dr Carter – so pharmacy teams are well-placed to refer customers to their dentist or GP to get any worrying symptoms checked out.
“Rather than advising to use a topical ulcer remedy, which could just mask the symptoms, it is important that pharmacy staff recognise that this could potentially be a sign of mouth cancer,” he says. “Before recommending a topical remedy, it is essential to ask how long a customer has had the ulcer.”
Dr Carter also advises speaking to any customers who could be at a higher-than-normal risk. “This includes people who smoke or drink to excess, or a combination of both,” he says, “as well as people who chew tobacco or other substances. Getting to those who don’t think they are at risk is very important.” With the increase in HPV-related mouth cancer, young, sexually active people should be targeted, he says, particularly young men.
“Young women receive the HPV vaccine as part of a schoolbased programme but young men don’t, which leaves them at risk. Making them aware of this can help to save a life.”
Boys in Australia, Austria, Brazil, Canada, Israel and the United States are offered the vaccine and Italy has decided to do the same. It is unacceptable that boys in the UK are being left behind and exposed to the virus, says Peter Baker, HPV Action campaign director.
Carl Alexander suggests pharmacies stock Cancer Research UK’s free leaflets and display posters prominently within the pharmacy to encourage customers to ask for advice. “The resources cover topics including spotting the signs of cancer, stopping smoking, and how to eat and drink healthily,” he says.
“It is important to make sure that any information is accessible to all groups. Where identified, smokers should be advised that the most effective way to quit is through attending NHS Stop Smoking Services. Pharmacists can also provide products and brief advice to help give up smoking, including on e-cigarette use, encouraging users to follow instructions and making sure they use enough of any NRT.”
Common oral health problems in pharmacy
Toothache
According to National Smile Month statistics, nearly 30 per cent of adults suffer from regular dental pain. Toothache is often caused by decaying teeth and needs to be treated immediately before an abscess can develop. At first the pain may just be triggered by hot or sweet foods, but eventually it may last longer or become constant. Depending on the severity, tooth decay may be treated with a filling or with root canal treatment followed by a filling or crown.
“It is important to try and understand what is causing the toothache,” says Dr Nigel Carter, chief executive officer of the Oral Health Foundation. “Far more often than not, toothache is something that only a dentist will be able to help treat. Suggesting a sensitive toothpaste, a high fluoride toothpaste, interdental cleaning and an oral health routine that involves brushing at least twice a day for two minutes can help alleviate any problems before they can get seen by a dentist.”
Mouth ulcers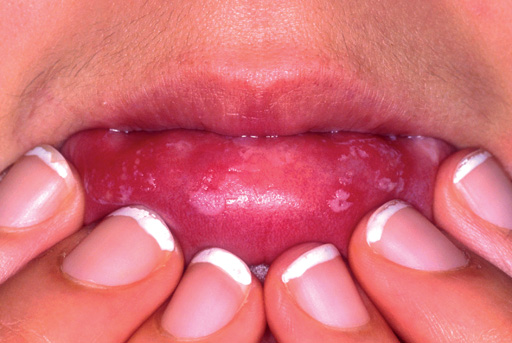
Causes of mouth ulcers include sharp teeth, brushing, poorly fitting dentures or biting the cheek or tongue. Recurrent mouth ulcers can be a sign of stress or anxiety or may be associated with some chronic medical conditions, such as inflammatory bowel disease. Most mouth ulcers disappear after one or two weeks and don’t need specific treatment but they can be very sore (especially when eating) – so customers may seek lozenges, mouthwashes, sprays and gels that help to ease the pain and encourage healing.
If ulcers appear for longer than three weeks, customers should be referred, says Dr Carter, as this could be a sign of mouth cancer. “If your customer has a number of mouth ulcers that keep coming back, this is called recurrent aphthous stomatitis,” he adds. “This is a common problem in otherwise healthy children and young people. The cause is not known, but it is not infectious and unlikely to be inherited.”
Sensitive teeth
Sensitive teeth affect up to three in 10 people in the UK. Sensitivity can occur at any time and varies in intensity and duration. Some people may experience an occasional twinge, while others may have severe discomfort for several hours or on a regular basis. Sensitivity can be aggravated by hot, cold, sweet or acidic food and drink, or even cold air. It may be due to an underlying dental problem, such as over-vigorous brushing, acid erosion or gum recession, and is also associated with tooth grinding.
If customers have sensitive teeth, they should switch to a softer toothbrush and use fluoride toothpaste that is formulated specifically to combat sensitivity. These products can take a while to work but if the sensitivity continues after a few weeks, or is severe, customers should see their dentist.
Bad breath
If customers have bad breath, they should keep a diary of everything they eat and drink, and any medicines they are taking. “All bad breath is caused by bacteria in the mouth,” says Dr Carter. “This has a large number of causes – everything from food stuck between the teeth, smoking and diet right through to underlying medical conditions such as diabetes and, most commonly, gum disease.”
Some mouthwashes can help to prevent and/or treat any gum disease, but these need to be used with a regular brushing and flossing regimen. “Over-the-counter products, such as mouthwash, can help to alleviate bad breath,” says Dr Carter, “but if it continues for a prolonged period of time and patients find they are just ‘covering it up’, they should be referred to a dentist to discover the underlying cause.”
Bleeding gums
Gums can bleed from time to time after overvigorous brushing or flossing but if a customer has gums that bleed regularly, after no obvious trauma, they should be referred to a dentist. Bleeding gums are one of the first signs of gum disease (gingivitis), which can lead to periodontitis, a major cause of tooth loss in adults. Gingivitis is generally caused by a buildup of plaque on teeth, close to the gum line. It is easily prevented with a regular oral care routine.
“A quick check in the mirror when brushing your teeth can reveal any early signs of gum disease, such as redness, bleeding or receding gums,” says Superdrug pharmacist Kathryn Granleese. “Customers should aim to brush their teeth just before they go to bed and on one other occasion each day for two minutes, as well as flossing regularly. Encourage them to attend regular dental appointments as, in most cases, a dentist or dental hygienist will be able to treat gum disease with a teeth clean.”
Cold sores
Cold sores are caused by the herpes simplex virus, which lays dormant in the body after an initial infection. A new outbreak may be triggered by an illness, stress, feeling ‘run down’, sunlight or hormonal changes in women. These small painful blisters appear around the lips and mouth. They usually begin with a tingling, burning or itching sensation on the skin before small fluid-filled blisters appear, usually on the edge of the lower lip. Cold sores are highly contagious, passing from person to person through close contact such as kissing, but usually scab over and disappear within seven to 10 days.
Most pharmacy customers can use OTC cold sore products to ease any pain and speed up the healing time. These products work best if they are used as soon as the initial tingling sensation occurs. If customers have any underlying health problems, or get recurrent cold sores, they should see their GP.
