Clinical

First aid & wound care: Sounding the alarm
In Clinical
Let’s get clinical. Follow the links below to find out more about the latest clinical insight in community pharmacy.Bookmark
Record learning outcomes
It is important to know when to raise the alarm if leg ulcers aren’t healing as expected.

Learning objectives
After reading this feature you should be able to:
- Recognise the red flag symptoms for leg ulcers
- Explain what complications can occur if treatment isn’t followed
- Know what to do in a medical emergency.
Â
If asked to consider wound care, many working in pharmacy would immediately think of first aid dressings. Yet these account for only a fraction of the NHS spend in the category. Of far greater financial significance for the healthcare system are chronic wounds and, in particular, leg ulcers.
These sores of the lower limb – most commonly located on the inside of the leg, just above the ankle – take many weeks to heal and can be expensive to treat. A German paper published in the International Wound Journal in 2014 put the costs to manage a leg ulcer in excess of the equivalent of £6,000 per patient.
Red flag symptoms
Venous leg ulcers account for around 80 per cent of all leg ulcers, according to the Circulation Foundation. What initially seems to be a relatively minor knock fails to heal in the expected one to two week timeframe, usually because of an underlying problem with the veins in the leg. This may be because of mobility issues – osteoarthritis or obesity, for example, or perhaps a recent fracture or surgery – or varicose veins.
Whatever the root cause, the effect of constant high blood pressure inside the veins slowly but surely damages the capillaries near the skin surface, making it much more fragile than before.
There are often warning signs that an injury is not healing as would normally be expected, says Dr Bav Shergill of the British Association of Dermatologists (BAD). “Brown spots and patches may appear on the skin, and the altered blood flow can turn the skin various shades between red and blue.â€
Other red flag symptoms include swelling of the leg, finding it painful to stand for long periods, and the skin becoming itchy and scaly with firm, tender areas underneath, he adds. Once it has developed, an ulcer has a distinctive appearance, says Dr Shergill.
“The bed of the ulcer may show bumpy, moist and red healing tissue, or may be covered in a yellowish-grey layer. Ulcers often leak fluid, the amount of which can vary.†Leg ulcers are hugely susceptible to bacterial infection, which is usually indicated by an increase in pain, redness and swelling around the sore, a significant quantity of green or unpleasant pus oozing from the site, and a fever.
First aid kits
There are few basic skills that have such an impact as knowing first aid. Being able to help someone who is injured or ill and keep them safe until they can see a medical professional can be the difference between life and death. Even those who are not seriously unwell will feel reassured by knowing they are being attended to by someone with first aid knowledge. Every home should have a first aid kit that as a minimum contains the following:
- Plasters and a roll of dressing strip
- Sterile dressings and dressing pads plus adhesive tape and scissors
- Eye wash and eye pad
- Sterile gloves and wipes
- Hand sanitiser.
Other items that may be useful include an instant ice pack, triangular bandage to be used as a sling and a first aid booklet.
While household items can be pressed into service if need be – clothing can be used to support a suspected broken bone or sprained joint, for example, or a tea towel employed as a makeshift dressing pad to staunch bleeding – having a purpose-built kit on standby can save time and enable the person administering the first aid to be more attentive to the patient instead of having to think about what they can use and then trying to find it.
Â
Other causes
If venous disease is responsible for some 80 per cent of leg ulcers, what causes the remaining 20 per cent? According to the Circulation Foundation, arterial disease accounts for about 15 per cent, with other causes, such as diabetes and rheumatoid arthritis, making up the rest.
Some cases may be the result of more than one condition simultaneously causing damage. During diagnosis of a leg ulcer, a Doppler test is often carried out to establish whether peripheral arterial disease is at play in order that the correct treatment is provided. See Circulation Foundation: leg ulcers
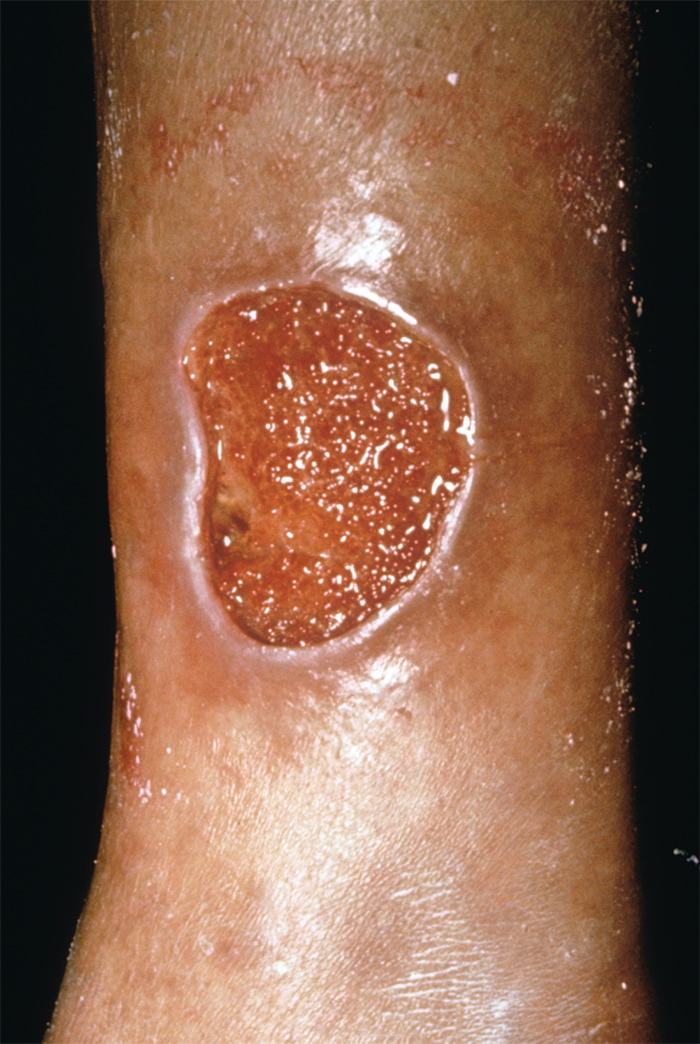 Venous leg ulcers are the most common ulcer type
Venous leg ulcers are the most common ulcer type
Â
Urgent care required
While some first aid situations require relatively minor treatment, it is vital to be able to identify medical emergencies, such as the following:
- Fractures can be difficult to distinguish from sprains and strains, but if there is any doubt at all, the most sensible course of action is to manage the patient as if they have broken a bone. This involves keeping the limb as still as possible, applying an ice pack if feasible, and getting them to hospital for an x-ray. Food and drink should be avoided in case the patient requires surgery and will need to be anaesthetised. Signs that a fracture may have occurred include severe pain, swelling or tenderness around the injured area, and bleeding, which may be under the skin
- Heart attacks are sometimes mistaken for heartburn because the pain is usually located in the chest. However, the patient may describe the pain as “tight†or “crushing†rather than the burning sensation of indigestion, and may complain that it travels into one or both of the arms, the jaw, neck, back or abdomen. An ambulance should be called and the person made comfortable while they wait, taking only any angina medication they may have or a 300mg aspirin tablet chewed slowly if there are no contraindications
- Stroke may be misidentified as drunkenness or a fit, but this only delays treatment, which is more effective the earlier it is delivered. Signs of a stroke can include weakness down one side of the body, which may be seen in the face as well as the body; speech problems, which extend to comprehension of others as well as difficulties speaking themselves; swallowing issues; and dizziness or loss of consciousness
- Shock is a state in which the circulatory system fails to provide enough oxygen to the body’s organs and can result from a huge range of problems, from severe blood loss, burns or vomiting, to anaphylaxis, a bacterial infection or a heart attack. It can appear that the patient has fainted, but on closer examination the pulse and breathing will be rapid and shallow rather than slow. Comfort, warmth and reassurance should be provided while an ambulance is called.
Making it better
The management of uncomplicated venous leg ulcers involves several steps:
- The wound must be cleaned to remove slough and any necrotic, fibrous or excess granulation tissue – usually achieved by irrigation and gentle washing. Occasionally debridement (surgical excision of dead tissue or cellular debris) may be considered necessary
- The wound is then dressed using a low-adherent dressing for the most part, but employing a hydrocolloid, alginate or hydrogel if pain, heavy exudate or sloughing respectively is an issue. Compression therapy is then applied below the knee – two layers if the patient is mobile, or three or four if they are not. This reduces venous reflux and ankle oedema and increases venous blood flow, which in turn improves the circulation and healing
- The patient should be followed up at least weekly for the first couple of weeks in order that dressings can be changed and the healing process evaluated. This also provides a useful opportunity to check on the patient’s compliance with their prescribed compression therapy and their general well-being. Once the ulcer is healing, appointments can be stretched out to fortnightly, then monthly, and finally every three months.
Dr Shergill says pharmacists and their teams have a valuable role to play in supporting patients with venous leg ulcers and their carers, particularly when it comes to providing encouragement and advice on some of the problems commonly experienced.
“Oedema can be reduced by regular exercise and keeping the affected leg raised while inactive. Less mobile people can exercise their leg muscles by moving their foot up and down at the ankle,†he says. Diuretics are not appropriate under such circumstances.
“Dry skin and eczema can occur around the ulcer, so advice on how to keep this area moisturised effectively through the regular use of emollients is useful,†Dr Shergill continues. Paracetamol can be used for pain, plus codeine if necessary, although it is worth highlighting the fact that worsening pain usually indicates a problem that warrants medical attention, such as an infection, diabetic neuropathy or arterial disease.
Community pharmacy teams can also provide advice on compression product care, says Dr Shergill. “Patients should follow the instructions carefully, as washing at the wrong temperature can damage the elastic. Patients also need to make sure compression products are replaced every three to six months because over time they lose their stretch.â€
It is sensible to check if patients are putting on stockings or bandages themselves, he adds, in order to reinforce basic advice such as the importance of not pulling them up too high or turning over the tops.
Managing minor emergencies
Many injuries look nasty when they first occur but will respond to relatively straightforward treatment.
 Nosebleeds look dramatic but rarely indicate anything serious. Whether the blood is flowing from one or both nostrils, the patient should be sat down and told to firmly pinch the soft part of the nose, below the bridge but above the nostrils, while leaning forward in order to avoid blood draining into the throat. An ice pack placed on the bridge of the nose will constrict the blood vessels. If the bleeding is very heavy or persistent or breathing is difficult, medical advice should be sought, as is the case for children under the age of two years, regular nosebleed sufferers and if the nosebleed is part of a larger injury (e.g. a bad fall or car accident)
Nosebleeds look dramatic but rarely indicate anything serious. Whether the blood is flowing from one or both nostrils, the patient should be sat down and told to firmly pinch the soft part of the nose, below the bridge but above the nostrils, while leaning forward in order to avoid blood draining into the throat. An ice pack placed on the bridge of the nose will constrict the blood vessels. If the bleeding is very heavy or persistent or breathing is difficult, medical advice should be sought, as is the case for children under the age of two years, regular nosebleed sufferers and if the nosebleed is part of a larger injury (e.g. a bad fall or car accident)- Burns and scalds should be cooled using cold running water until pain subsides or for a minimum of 10 minutes. Any clothing or jewellery should be removed carefully unless it is stuck to the skin. The area should then be covered using plastic film and the limb raised if there is swelling. Materials that may shed fibres, creams, lotions and sprays should not be used. Further treatment is necessary for large or deep burns, all chemical and electrical burns, and any burns that blister. The elderly and infants should also be seen, as should anyone with a weakened immune system or a long term-condition such as diabetes
- Bleeding that is minor requires nothing more than thorough cleaning and covering with a sterile dressing. The main risk associated with heavy bleeding is shock as a result of blood loss, so staunching the flow is the usual priority. Pressure must be applied to the wound – if there is an object embedded in the wound, padding should first be built up around it in order to avoid forcing the item in further – and then maintained until the bleeding has stopped. The limb should also be raised unless there is suspicion of a fracture. Serious bleeding should always be checked by a medical professional.
Sticking to the regimen
When it comes to the management of venous leg ulcers, adherence is a must. As well an infection, possible complications include immobility due to pain, time off work, distress, loss of independence and social isolation, as well as serious conditions such as osteomyelitis and septicaemia.
If there appears to be an infection, the ulcer should be swabbed in order to inform appropriate antibiotic use. Compression therapy should be delayed until the infection has resolved as it is not only painful for the patient, but impractical given that daily inspections of the wound are likely to take place. For very large or persistent ulcers, surgery may be necessary. An operation may also be performed to treat varicose veins if this is thought to be the underlying cause.
“Support is needed even after the ulcer has healed as the individual may need encouragement to adopt a lifestyle that reduces the risk of recurrence. Patients should be advised to cut down – or preferably stop – smoking and to take up a healthy, balanced diet,†says Dr Shergill. Losing weight if obese can also help, he says.
It is also essential to emphasise the importance of wearing the appropriate grade and type of compression stockings – as recommended by NICE – ideally for a minimum of five years. Class 3 products are generally advocated, but Class 2 may be worn if the person is unable to tolerate such high levels of compression. Lifelong wearing is sometimes necessary; for example by anyone suffering from recurrent venous leg ulcers.
Patients should be followed up every six to 12 months with the aim of identifying risk factors that increase the risk of ulceration (e.g. poor skin care, a deterioration in leg oedema, the development of varicose veins and trauma to the legs). Attending a leg club can help patients feel in control of their condition and care. Details are available at The Lindsay Leg Club.
Â
Find out more
- A free first aid guide can be downloaded from the St John Ambulance website. A free app is also available, providing advice on a range of emergency scenarios including hypoglycaemic episodes, choking, allergic reactions, and cardiopulmonary resuscitation. First aid courses can be booked here
- The British Red Cross has online training in video form, which explains first aid skills for situations as disparate as poisoning, hypothermia and meningitis. Courses can be booked hereÂ
- St Andrew’s, Scotland’s leading first aid charity, runs courses at a number of centres, which are bookable here. The website also features a calculator to help employers assess whether they have sufficient first aid cover and supplies for the workplace(s) they are responsible for. See St Andrew's First Aid: workplace requirements calculator
