Clinical

Pain management
In Clinical
Let’s get clinical. Follow the links below to find out more about the latest clinical insight in community pharmacy.Bookmark
Record learning outcomes
In order to put the squeeze on pain, don’t just reach for the OTC analgesics. Your customers will also benefit from any advice you can give them on positive coping strategies.

Â
Learning objectives
After reading this feature you should be able to:
- Play a more prominent role in managing pain
- Identify those patients not using medicines to optimum effect
- Have a deeper understanding of how pain can disrupt people’s lives.
Â
A 29-year-old builder was taken to an A&E department in Leicester after jumping onto a six-inch nail, which went right through his boot behind the steel toecap. As the smallest movement of the nail was painful, he received fentanyl and midazolam. The nail was then pulled out but, when his boot was removed, it was clear that the nail had been between his toes. Despite his obvious distress, there was no tissue damage.1
As this example illustrates, pain is deeply personal. In addition to tissue damage, the experience of pain can be influenced by emotions, psychology, cognition, social factors and expectations. Indeed, expectation in itself can be a potent analgesic.
A surgeon operating near the front line during the Korean War began suffering severe abdominal pain, which he knew indicated acute appendicitis. As the incoming wounded needed help, he asked a nurse to give him a morphine injection.
When he returned to duty following an appendectomy, the doctor was looking through the operating room records and found that, “since he appeared distressedâ€, the nurse had injected saline (probably to avoid mental fogging). The doctor had expected the nurse to follow his instructions and this had invoked the placebo response that overcame the pain of acute appendicitis.2
The complex interplay between tissue damage, psychology and social factors means that some 28m people in the UK endure chronic pain, according to a meta-analysis of 19 studies involving 139,933 adults.3 Overall, between 35 and 51 per cent of adults live with chronic pain.
This discomfort takes numerous forms including chronic widespread pain (experienced by 14.2 per cent of adults), chronic neuropathic pain (8.2-8.9 per cent) and fibromyalgia (5.4 per cent). The prevalence of chronic pain rose with age, from 14.3 per cent in those aged 18-25 years to 62 per cent in those over 75 years of age.3
The meta-analysis also found that between 10.4 and 14.3 per cent of adults experience moderately to severely disabling chronic pain. Similarly, according to the National Pain Audit, 11 per cent of adults and 8 per cent of children suffer severe pain (equivalent to 7.8m people in the UK). Older people, females, those living in poor housing and with certain jobs are all more likely to experience chronic pain.
“Community pharmacists are a central pillar in the management of chronic pain,†says Dr Cathy Stannard, consultant in complex pain and pain transformation programme clinical lead at NHS Gloucestershire CCG. “Pharmacists are well placed to get to know their patients and begin to understand their pain.â€
In addition, community pharmacists can encourage rational analgesic prescribing. “Many painkillers, particularly opioid analgesics, have little direct analgesic effect in chronic pain,†she says, “but patients often use opioids to blunt unpleasant feelings that contribute to their experience of pain. Patients start using opioids to alleviate pain and then keep using them to help get through the day.â€
Effective assessment
Effective assessment is the keystone of pain management and Dr Stannard stresses the importance of focusing on the patient’s experiences and circumstances. Acute pain is short-term and usually follows an injury, such as an operation, fracture or infection. In one study from North-East London, for example, 68 per cent of patients reported pain 48 hours after discharge from day-case surgery and 26 per cent reported severe pain.4
Acute pain is usually self-limiting, resolves once the underlying problem is treated or heals – which generally takes days or weeks – and typically responds well to analgesics, including those available OTC from pharmacies.
Chronic pain is more persistent or recurrent but, rather than set an arbitrary time – such as three months – at which pain becomes chronic, Dr Stannard suggests considering whether the persistence is abnormal for the acute injury. “Experiencing pain a week after a mild groin strain is normal,†she points out.
“If the person is still in pain a month later, that is abnormal and should trigger further investigation. Pain that is distressing or disabling and which is not associated with obvious injury needs evaluation whether or not it has lasted for three months.â€
Nevertheless, pain’s subjective, multifaceted nature can make assessment difficult. “The severity of acute pain is a good indicator of the extent of the underlying damage,†Dr Stannard comments, “but, in chronic pain, the severity of the pain, anxiety and distress often bears little, if any, relationship to the tissue damage. There are a few obvious exceptions, however, such as the pain associated with sickle cell crises or spinal collapse in osteoporosis.â€
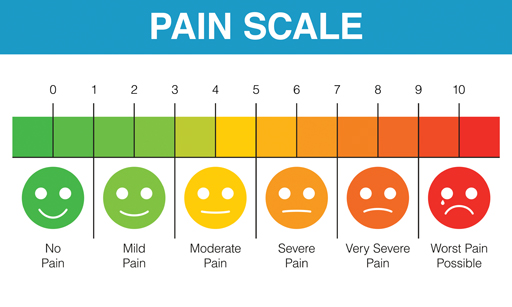
In addition, patients may see their pain differently to healthcare professionals. Patients are often asked to rank their pain on a scale of 0 (no pain) to 10 (the worst they have experienced or can imagine). Often the pain is the worst the patient has experienced, but clinicians have seen far worse.
“To me, a person with a rating of 10 would not be able to function, yet some patients drive to my clinic and say that their pain is 10,†Dr Stannard says. “Nevertheless, if someone says their pain is 9 or 10, then they want you to do something about it. They’re asking for help.â€
Against this background, pharmacists could ask those patients with chronic pain to keep a diary for a couple of weeks as this can offer valuable insights, such as whether a pattern emerges, if there are any triggers and the efficacy of pain medicines.
Dr Stannard suggests asking patients to complete the diary or app at the end of each day. “This offers them the opportunity to reflect on whether it has been a good day and identify any antecedents,†she says.
Â
Tackling inappropriate prescribing
Effective evaluation, such as during a MUR, offers pharmacists an ideal opportunity to tackle inappropriate prescribing and check compliance with analgesics. “People in chronic pain are often awash with medicines, although sometimes these are not very effective,†Dr Stannard says.
“Analgesics generally help only about a quarter of people in chronic pain. Paracetamol and ibuprofen help people self-manage mild acute pain, but are unlikely to help most cases of chronic pain.â€
MURs can, for example, help tackle inappropriate opioid use and educate patients. According to the National Pain Audit, 52 per cent of patients reported difficulty understanding chronic pain. Dr Stannard also notes that patients in chronic pain often don’t understand their treatment. “There is a pressing need to educate patients and prescribers that increasing the dose, for instance, might not be the most appropriate approach,†she remarks.
The analgesic effect of opioids often wears off relatively rapidly and increasing the dose is unlikely to yield much additional benefit in people with chronic pain. “If conventional doses of analgesics do not alleviate the pain, it is probably better to consider alternatives – such as referral to a pain service – than to keep increasing the dose,†Dr Stannard says. “If a pharmacist identifies someone who remains in pain despite taking high-dose opiates, the drugs aren’t working.â€
Pharmacists need to be cognisant of the unmet and often undisclosed emotional needs of people in chronic pain who are taking high-dose opiates, says Dr Stannard. “Many people who have chronic pain that persists despite very high doses of opioids will report that they are living with other difficult burdens, such as domestic violence, a history of sexual or physical abuse, or another emotional trauma.
“For these patients, analgesics are never going to be the answer. Patients need expert and sensitive assessment and support and referral to appropriate services. For all patients with pain, whether acute or chronic, there is a need for support in understanding the role of medicines in pain management, which pharmacists are well placed to offer.â€
Surveys suggest that people in chronic pain often experience considerable delays accessing the help they need. According to the National Pain Audit, 20 per cent of the patients with chronic pain who responded to its survey had reported visiting A&E in the previous six months to find help. They had all seen their GPs, with 66 per cent making more than three visits to healthcare providers.
However, the audit also found marked variation in access to multidisciplinary care (essential for specialist chronic pain services) and waiting times.
The enigma of neuropathic pain
Medications are the mainstay of management for chronic neuropathic pain – despite not being very effective. “In clinical trials that enrol people with a discrete condition, such as pain following shingles, [only] about a third of people with neuropathic pain respond to any given drug,†Dr Stannard says.
“Fewer people respond in clinical practice, maybe a fifth. However, neuropathic pain causes patients considerable distress, is often disabling and, for most people, there are few alternatives to medicines.â€
Analgesics generally help only about a quarter of people who are suffering chronic pain
Dr Stannard is also able to lay a pharmacological myth to rest – namely, opioids work in some people with neuropathic pain. “The low response rate in clinical studies leads clinicians to conclude that opioids are ineffective in neuropathic pain,†she says. “We now know that opioids are no more and no less effective than other drugs. Tramadol, for example, shows broadly similar efficacy in neuropathic pain to amitriptyline and gabapentin.â€
For reasons that remain biologically obscure, some people with neuropathic pain respond to some drugs but not to others. So if a pharmacist identifies during a MUR or NMS review that the neuropathic pain is not responding adequately to treatment, Dr Stannard suggests referring patients for a different drug. “If patients do not respond to amitriptyline, they may respond to gabapentin, and vice versa,†she says.
Key facts
- Effective assessment is the keystone of pain management
- MURs can help tackle inappropriate opioid use and educate patients
- People in chronic pain often experience considerable delays accessing the help they need
Lack of innovation
Around 3400 BC, the Sumerians were among the first people to cultivate the poppy plant. Eventually, every major civilisation in Europe and Asia used it as an analgesic and to treat numerous ailments.5 Opioids remain the most effective analgesics, despite numerous potential targets for novel analgesics being heralded in pharmacological literature and conference presentations.
Recent advances have helped our understanding of the underlying neurobiology but these insights have yet to translate into effective new treatments. “It is all fascinating,†Dr Stannard says, “but these insights are not therapeutically as exciting as they seem: they have not resulted in new effective analgesics in the clinic. Patients are more complex than the animal models employed in analgesic studies. Psychological and emotional factors have a major influence on patients’ pain experiences, for example.â€

Some pain syndromes are proving especially difficult to treat despite considerable research. “We have known about phantom pain, for instance, for nearly four centuries, but we are no better at treating it,†says Dr Stannard. The aetiology of phantom pain is reasonably well understood – the sensory and motor cortex receives nerve signals from around the body but when the brain no longer receives the input, it fills in the sensory gap. This produces the sensation of pain in the missing part of the body.
“Phantom pain can arise from lost limbs or following a mastectomy,†Dr Stannard adds. “It can cause great suffering and psychological distress. Despite understanding how and why phantom pain arises, we have little to offer other than the relatively ineffective drugs for neuropathic pain. Being able to offer people with phantom pain an alternative treatment would be a real step forward.â€
Clearly, we still have much to learn about the causes and treatment of chronic pain. In the meantime, community pharmacists will remain in the vanguard of pain management. “Pharmacists can offer a range of OTC treatments to help people manage pain. They can also offer advice, education, support and appropriate referral,†Dr Stannard says.
“In some cases, however, the most appropriate treatment for chronic pain is to stop drugs. If a GP suggests stopping a drug, the patient might suspect that they are just trying to save money – but patients recognise that pharmacists are the experts about medicines. So, if a pharmacist suggests that the most appropriate approach for chronic pain is to stop taking analgesics, patients will listen. It is a very potent message.â€
Effective interventions
Simple analgesics, heat pads and other products have an important role in the management of short-term pain associated with injury. Simple analgesics may also help while people wait for referral and, used intermittently, allow self-management when episodic discomfort – such as flare-ups of arthritis – makes normal function difficult.
“Taking simple oral analgesics can help people with breakthrough pain regain control,†Dr Cathy Stannard says. “Heat pads and topical treatments can also help. However, there are much more effective interventions for people who experience persistent discomfort, including remaining active.â€
Some people in chronic pain even find walking difficult, says Dr Stannard. “Medications can help as part of a treatment plan to get people active. Pharmacists need to have a conversation with people in chronic pain to look at other ways of managing the discomfort. They need to reassure these people that there probably isn’t anything seriously wrong and that medications alone are unlikely to help long-term.â€
Â
References
1. Anonymous Minerva. British Medical Journal 1995; 310:70-70
2. Wall P. Pain and the placebo response. Ciba Foundation Symposium 1993; 174:187-211; discussion 2-6
3. Fayaz A, Croft P, Langford RM et al. Prevalence of chronic pain in the UK: a systematic review and meta-analysis of population studies. BMJ Open 2016; 6:Doi:10.1136/bmjopen-2015-010364
4. Fahmy N, Siah J, Umo-Etuk J. Patient compliance with postoperative analgesia after day case surgery: a multisite observational study of patients in North East London.
British Journal of Pain 2016; 10:84-89
5. Rosenblum A, et al. Opioids and the treatment of chronic pain: controversies, status and future directions. Experimental and clinical psychopharmacology 2008; 16:405-416
For the latest OTC product news in the pain category, click here.
