Clinical

Medical skincare: Picking up the pieces
In Clinical
Let’s get clinical. Follow the links below to find out more about the latest clinical insight in community pharmacy.Bookmark
Record learning outcomes
Through careful questioning and expert advice, pharmacists can help find solutions to a range of common skincare conditions.

Learning objectives
After reading this feature you should be able to:
• Recognise different skin conditions
• Offer advice about each condition and the correct use of treatments
• Know when to refer to a GP.
Community pharmacists have an important role to play in helping support patients with skin problems. In this feature, we explore several scenarios to illustrate some of the ways in which pharmacists can help patients presenting in pharmacy with a range of common skin health conditions.
Allergic skin rash
A 16-year-old girl presents at the pharmacy complaining that an itchy rash has appeared all over her body that morning and wanting to buy some cream to help relieve the itching. On examination, you notice small (1-2cm) flesh-coloured swellings on the skin, surrounded by an area of erythema. She has no other medical problems but mentions that she had eczema as a child, which seemed to have gone away. She is a keen runner and yesterday started taking ibuprofen for a sprained ankle. What is the likely diagnosis and how should she be managed?
Answer
In this case, the most likely diagnosis is acute urticaria or hives. The condition is characterised by pruritic wheals (the small skin-coloured swellings) and erythema. Acute urticaria is common and affects one in six people at some time in their life. It is also more prevalent in patients with atopy (i.e. those with asthma, eczema and hay fever).
Urticaria is an immunologically IgE mediated type-1 hypersensitivity reaction that results in mast cell degranulation and the subsequent release of histamine, but other agents are also thought to be involved. The physiological effects are due to increased capillary leakage of fluid that results in skin swelling and vasodilation, which produces the erythema.
Although acute urticaria is a relatively straightforward diagnosis, finding a possible cause is more difficult. In up to 50 per cent of cases, no specific trigger can be found. Asking your patient about her general health (i.e. considering other medical problems), occupation, hobbies, new pets, recent ingestion of new foods, viral infections or medicines could help to pinpoint the causative agent.
Her recent use of ibuprofen is actually a potential cause. When questioning her, you establish that she has not used ibuprofen before and that it was suggested by her mother, who uses it to treat back pain. Although urticarial reactions to NSAIDs can occur within 15 minutes of ingestion of the drug, a reaction can also take place several hours later. As ibuprofen is the most likely cause, stopping the drug should lead to a resolution of her symptoms over the next 24-48 hours.
If she wants to take something to help relieve the pruritus, oral second-generation antihistamines such as cetirizine or loratadine are appropriate. Topical antihistamines would be unsuitable given the widescale nature of her rash and, having been associated with sensitivity reactions, are best avoided.
Additional acne treatments
Nineteen-year-old Emma, a university student, comes to the pharmacy and collects her prescription for lymecycline 408mg for acne. Emma asks about using a cream to help get rid of her spots because she feels that the tablets aren’t working very well. What advice would you give her?
Answer
Acne is a very common condition affecting up to 80 per cent of people aged between 11 and 30 years, although the peak incidence occurs among those aged between 14-19 years of age. It has been suggested that up to 60 per cent of people with acne seek treatment. Typically, acne predominately affects the face but also occurs on the back and chest. Lesions are described as either non-inflammatory (blackheads and whiteheads) or inflammatory (papules and pustules).
It is important to explain to Emma that acne responds slowly to treatment and to wait for up to eight weeks before assessing the response. Failing to appreciate this timescale is likely to result in poor adherence and cessation of treatment at an early stage.
Studies suggest that patients’ understanding of the causes of acne is poor, leading to practices such as excessive cleansing with commercial washes that contain abrasive or exfoliating agents, which may aggravate acne. Simply washing with soap and lukewarm water twice a day is sufficient. Although the role of diet in acne remains controversial, there is some evidence that consumption of a low glycaemic index diet (i.e. reduced refined carbohydrates such as in crisps and white bread) improves acne.
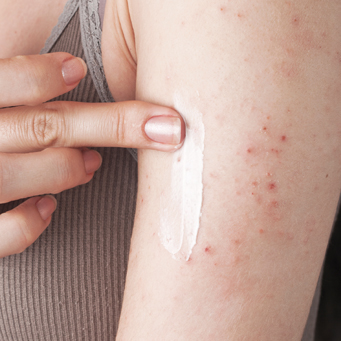
If Emma does want to use an OTC product, one containing benzoyl peroxide would be appropriate. Benzoyl peroxide is effective at reducing both non-inflamed and inflamed lesions, although it can cause skin irritation when first used. Available as a gel/cream and wash, benzoyl peroxide should be applied for short periods of time initially (up to 20 minutes) after washing the skin with soap and water, and then rinsed off. The contact time can be gradually increased as the skin becomes more tolerant.
Adherence to topical psoriasis treatments
Tom, a 69-year-old regular customer, was recently diagnosed with plaque psoriasis on his elbows and knees. His GP prescribed both betamethasone 0.1% and calcipotriol cream 0.05%. He was told to apply the calcipotriol in the morning and the betamethasone cream before going to bed. Tom has been trying to comply with this regimen but says he gets very tired in the evenings and often forgets to apply his betamethasone cream. Tom, who has been using his creams for the past three weeks, is due to see his GP again next week. He tells you he is concerned that his treatment is not working very well. What advice would you offer him?
Answer
Psoriasis is a chronic, inflammatory skin condition thought to affect up to 3 per cent of the population. Over 90 per cent of patients (like Tom) have plaque psoriasis. The majority of sufferers have mild to moderate disease, which can be managed in primary care.
Guidance issued by NICE in 2012 suggested that first-line topical treatment should be with a potent topical steroid (betamethasone) and a vitamin D analogue (calcipotriol), applied separately, preferably morning and evening. Patients should then be assessed after four weeks. Topical vitamin D analogues can take several weeks before an improvement is seen, whereas most patients using topical steroids can expect see a response after two to four weeks.
As Tom appears to be forgetting to apply his topical steroid, his psoriasis is unlikely to show much of a response after three weeks. Adherence can be either unintentional – when the patient simply forgets or finds the preparation difficult to use – or intentional (where the patient makes a conscious decision not to use prescribed treatment). Irrespective of the origin of the problem, poor adherence can lead to therapeutic failure and unnecessary changes to treatment.
Studies suggest that adherence to topical treatments ranges from 50-60 per cent. One potential strategy to improve adherence is to simplify the dosage regimen. Clearly Tom is experiencing difficulties remembering to use his night-time cream, so a potential solution is to change his prescription to a combination product that contains both a topical steroid and calcipotriol (e.g. Dovobet). In addition, educational advice to enhance Tom’s understanding of the role of treatment (e.g. how to apply the product, when it can be stopped, when to restart) may increase his confidence in managing his psoriasis and lead to improvements in adherence.
Advice on managing an eczema flare
Leanne is a 27-year-old mother whose four-year old son, Nathan, has suffered from eczema since he was eight months old. Her GP has prescribed a bath oil and hydrocortisone cream 1% for his eczema but Nathan doesn’t like the bath oil so Leanne lets him use a commercial bubble bath product instead. Leanne asks for advice because Nathan isn’t sleeping very well and is scratching his skin. Leanne is worried because Nathan’s teacher has mentioned that he doesn’t appear interested in class and has occasionally fallen asleep. What advice would you give to Leanne?
Answer
Atopic eczema is a chronic, itchy skin condition that follows a relapsing-remitting pattern. It is estimated to affect between 15-20 per cent of children and 2 to 10 per cent of adults. The precise cause of eczema is complex, but in simple terms eczema patients have an impaired skin barrier that leads to increased water loss and provides an entry portal for bacteria and allergens that can trigger an eczema flare. Eczema in school children typically affects the inner creases of the elbows and behind the knees, although it is important patients appreciate that the whole of the skin is susceptible to eczema.
Guidance from NICE in 2007 suggested that the cornerstone of eczema management was the use of emollients that form a water impermeable layer over the surface of the skin. This action has a dual function; it reduces water loss through the skin and prevents the entry of potential allergens and irritants. Emollients should be applied liberally (a child would require between 250g and 500g per week) and frequently, even when the skin is clear, as maintenance therapy.
Parental education is crucial for understanding how to manage eczema. Leanne has only been prescribed a bath emollient (which she doesn’t use) and a mild potency steroid cream. Nathan is currently experiencing an eczema flare, characterised by increased skin dryness, itching, redness, swelling and general irritability, leading to a lack of sleep and increased scratching, so he should be referred back to his GP.
The most suitable treatment to manage the flare is a potent topical steroid for a few days and increased emollient use. In addition, since Nathan is experiencing sleep disturbance, it would be prudent to prescribe a sedating antihistamine such as chlorphenamine solution. Suggest to Leanne that she asks her GP for a large quantity of a leave-on emollient and a potent topical steroid to keep in reserve to manage a flare if increased emollient use does not help.
If Nathan wants to use a commercial bubble bath, one solution is for Leanne to pour the emollient bath oil into the bubble-bath bottle.
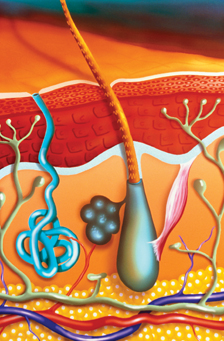
Managing recurrent cold sores
Joanne comes to see you in the pharmacy for advice about a cold sore. She complains that she seems to be getting a lot of them and wonders if there is a cream that would help prevent them. What advice would you give her?
Answer
Cold sores (oral herpes labialis) are due to infection with herpes simplex virus type 1 (HSV-1). Cold sores affect between 20-40 per cent of young adults although by early adulthood the prevalence can be as high as 85 per cent. Cold sores initially develop as erythematous areas that swell into papules and then vesicles on the edge of the lower lip. These vesicles subsequently burst and collapse into ulcers over the next one to three days. The ulcers crust over and the skin returns to normal within two weeks.
The primary infection with HSV-1 can occur in childhood and is often asymptomatic. Between six and 24 hours before the development of a cold sore, up to 60 per cent of people experience warning or prodromal symptoms such as pain, burning and/or tingling and itching at the site where the cold sore subsequently appears.
After the initial infection, the HSV-1 virus becomes dormant and resides in the sensory ganglia or nerve endings. Between 20 and 40 per cent of young adults who test positive for the HSV-1 virus develop recurrent cold sores, with most individuals experiencing around two infections a year – although up to 10 per cent of patients have a minimum of six episodes per year. The reasons for recurrence include exposure to UV radiation, stress, illness and premenstrual tension.
Unfortunately, there is little that can be done to help Joanne. There are no treatments that can remove the virus permanently, although patients who experience recurrent infections should try and minimise exposure to potential trigger factors. If UV exposure is a potential trigger, then lip balms with a SPF of 15 might help. A recent Cochrane review that considered the effectiveness of preventative measures found that while use of oral antiviral agents, such as acyclovir, did reduce the incidence of recurrence, this effect was small.
There was also no evidence that topical antivirals prevented recurrence and while some studies suggested that the use of a lip balm with a sun protectant reduced the recurrence rate in response to artificial light, it did not prevent infections due to sunlight.
Managing hair loss in a young man
Andy is a 29-year-old local who asks to speak to you in private. He mentions that he seems to be losing his hair and is rather embarrassed about it. Andy describes how it first started a few weeks ago and occurred at the front of his head but now seems to be happening on both sides. He describes how his father had the same problem and that while only 62 he is now practically bald. Andy is concerned that he might go bald sooner, given that he seems to be losing a lot of hair. He has no other medical problems apart from asthma for which he uses a salbutamol inhaler occasionally. What advice would you give to Andy?
Answer
Based on his description of the problem, Andy is most likely suffering from androgenic alopecia (hair loss) or male-pattern baldness. The condition is common and increases with age, affecting around 80 per cent of men aged over 70 years. Although signs can first appear in the teenage years, roughly half of those with the condition will be affected by the age of 50. The cause is unknown but believed to be androgen-dependent with a genetic basis. Over time, there is a gradual reduction in the size of hair follicles, and terminal hair (i.e. normal hair) is replaced by thinner and less pigmented vellus hair.
There is no cure for androgenic alopecia. Andy needs to decide whether or not to use treatment. The only OTC treatment available is minoxidil as a 2% or 5% application. If Andy decides to use treatment, it would be advisable to start with the 2% solution and then increase to 5%. According to NICE Clinical Knowledge Summaries, minoxidil is not very effective but works best if used at an early stage. It does not affect the hair loss process but appears to thicken and increase the density of remaining hair. In clinical studies, after 12 months of use, 25-50 per cent of men reported at least moderate hair regrowth. Treatment needs to be indefinite to be effective.
A second option would be referral to a GP, as finasteride 1mg (Propecia) is available on private prescription, although there is no convincing evidence that finasteride is more effective than minoxidil.
Skincare category advice
To support self-care for skin conditions and encourage customers to seek advice, a well-positioned, well-stocked medicated skincare category in pharmacy is a must.
Jesse Mu, brand manager of Dermalex, offers the following advice: “Pharmacists will benefit from stocking a wide range of skincare products that support both mainstream concerns, such as dry skin, and specialist conditions, such as rosacea. Consider the demographics of your shoppers as you select the best solutions to appeal to your community needs, and merchandise similar treatments and brands together to encourage a ‘one-stop shop’ experience for consumers.”
Jesse also advises pharmacists to discuss patients’ symptoms, concerns and satisfaction levels with current treatments before making product recommendations, as well as considering the benefits of dual action products and products that are “gentle on the skin, suitable for long-term use and those that can be used in combination with other treatments”.
In addition, she stresses the need to offer holistic support to patients and to ensure that pharmacy teams are able to signpost customers to useful online resources, such as NHS Choices, the Eczema Society or rosaceauncovered.co.uk – the latter a new website developed for Dermalex, which provides information on the triggers of rosacea along with expert tips and guidance on managing the condition.
