Clinical

Child & teen health: Open wide!
In Clinical
Let’s get clinical. Follow the links below to find out more about the latest clinical insight in community pharmacy.Bookmark
Record learning outcomes
Mary Poppins may have used a spoonful of sugar but nowadays helping the medicine go down is rather more complicated...
 
Â
Learning objectives
After reading this article you should be able to:
- Identify issues that can arise when dealing with medicines for children
- Understand the need for safeguarding policies and procedures
- Deal with common childhood ailments.
Â
When a patient brings in a prescription, it is relatively straightforward – but when the prescription is for a child, it immediately feels more complicated. A multitude of questions arise, such as whether the dose is suitable for the child’s age and weight and whether the drug is licensed for use in children in the first place.
Giving out the dispensed item also requires a bit more thought in terms of what information to provide to the parent or carer, the need to answer any questions they might have about the best way to get medicines into their charges and the thorny issue of whether services that would normally be offered for someone on that particular medicine are applicable to under-18s.
Teenagers bring their own extra brand of awkwardness, with many reluctant to be in the pharmacy in the first place, let alone prepared to listen to any advice supplied with their dispensed medication.
Added complexity
Steve Tomlin, the Royal Pharmaceutical Society’s expert on children’s medicines, agrees that supplying drugs to and for children brings with it an added layer of complexity. Of prime importance is dosing, he says, urging pharmacists and dispensing staff to check the dose against a child’s weight rather than age.
“Many products give age bands for dosing – for example, a 5ml spoonful for three to six-year-olds – but there are enormous variations across this range, so find out how much the child weighs and work it out from there,†he says.
Dosing errors can also result from inadvertent changes in product strength. Many medicines for children are made as specials, so the strengths are not necessarily consistent, he says. “A 5ml spoonful of a 10mg per 5ml liquid may be fine, but accidentally give 5ml of a 100mg in 5ml preparation of the same drug – easily done as the parent or carer may not think to check the label of something they give all the time – and the child has been given a dose ten times what it should be.â€
One way this can be avoided is by dispensing the same product to a patient every time. “Many medicines prescribed for children are unlicensed and while lots of different manufacturers make the same products, they all do it slightly differently, which means that bioavailability can vary.â€
Patients’ needs should be a higher priority than using the specials manufacturer with which a pharmacy has a supply arrangement, he adds.
Another problem he highlights concerns liquids. “Liquids are more expensive than tablets, accurate dosing can be difficult and often they are not very palatable. If a tablet is taken, it is clear how much of a drug has been consumed, but with a liquid, has 5ml been taken or a bit less or a bit more? “Studies have shown that from the age of four years, many children can take tablets, particularly if they are coated, but there can be reluctance on the part of prescribers, parents and children [to use them]. Children change as they grow up, so why shouldn’t their medicines evolve with them?†says Tomlin.
Â
Safeguarding
Safeguarding is the term used to describe the action taken to promote the welfare of children and protect them from harm. It is sometimes used interchangeably with the phrase ‘child protection’ but the latter is a little more specific, referring to the protection of individual children who have been identified as suffering or being likely to suffer significant harm.
Safeguarding and child protection guidance and legislation apply to everyone up to the age of 18 years. All organisations that come into contact with children – from health providers and schools to faith groups and community organisations – should have specific safeguarding policies and procedures in place to keep children safe and ensure they are not placed at unacceptable risk of harm. More information is available via the GPhC.
Â
Which services?
Another worry is which services can be offered. Rosie Taylor, head of service development for the Pharmaceutical Services Negotiating Committee says it often receives queries as to whether medicines use reviews can be conducted with children.
The answer is yes, but the child needs to be able to give informed consent, which means that they must understand what a MUR is, can engage with the process and understand that the information can be shared. It is the same for the new medicine service – there is no age limit. It is up to the pharmacist to use his/her professional judgement and discretion to decide whether it is appropriate.
“There is guidance on consent for anyone who is unclear on this matter, such as that issued by the General Pharmaceutical Council. However, there are two things to bear in mind,†she says. The first is that the service must be carried out with the patient, which is the child and not their parent or carer. The second is that for some services, there will be restrictions on eligibility according to age – for example, a locally commissioned stop smoking or emergency hormonal contraception service, which will be written into the service specification.
One thing everyone working in community pharmacy needs to be aware of is safeguarding, says Rosie Taylor. “For a lot of services, it is a requirement to have completed training on this subject and it is also a quality payment criterion in England. Putting that to one side, it is arguably something that anyone dealing with children on a daily basis needs to know about.†(See Safeguarding box above.)

Practicalities
Children’s medicine specialist Steve Tomlin urges pharmacists and their teams not to fall into the trap of thinking that someone further up the chain will have provided all the information a child or their carer needs to know about their treatment.
“You have to understand what is going on, and while nobody expects anyone to be an expert on every drug and every condition that affects children, it makes sense to have a sound grasp of the bread and butter of paediatrics: asthma, epilepsy and medicines for pain and fever.â€
Anika Shah, pharmacy manager at Kings Pharmacy in North London, agrees. “There are some obvious things to do when you get an inhaler prescription, for example, such as checking inhaler technique, but it is also important to think about practicalities. An inhaler that needs to be used four times a day doesn’t necessarily need to go into school, which the parent might assume, and instead can be given before and after school, in the early evening and at bedtime.â€
If medicines do need to go into school or another childcare setting, it is vital that everything is labelled meticulously, even if it is an OTC product, she says. “Staff in many places won’t give medicines to children unless they are labelled and there is also the stress of making sure the item is in the same place as the child when it is needed. Having two of something prescribed is ideal, as it means that, for example, a bottle of antibiotic liquid can be in the fridge at home and another in the fridge at school.â€
Apply common sense, advises Steve Tomlin. “What point is there in putting on the label of a medicine for a child on nasogastric feeds that this item should be taken on an empty stomach? Not only is it unnecessary and unhelpful, it can also be upsetting for all involved.â€
Communication channels
The best prescribing in the world is futile if the patient can’t or doesn’t want to take the medicine in question, says Anika Shah. “Talk to the patient or parent and find out what they are worried about. For a steroid inhaler, they might be put off by reading in the product information that growth can be affected, but this can be addressed by explaining that the risk is tiny and massively outweighed by the benefit of the patient being able to breathe properly.â€
Teenagers can be particularly tricky, she says. “They might be embarrassed to use medicines in front of their friends, so be sensitive as to what is important to them and come up with things that work for them rather than pushing your own thoughts and feelings. Be prepared to go the extra mile. For instance, we don’t have a service that allows us to provide EHC free of charge, so in the past I have contacted a patient’s GP to get a prescription sent over rather than sending them away as it can put them in a difficult situation.â€
Steve Tomlin agrees. “A teenager may have been put on a course of antibiotics but is going to delay starting it because they are going out over the weekend. Unless the antibiotic is metronidazole, there is no need for them to do this. Similarly, they may be deterred from taking something because weight gain is mentioned in the product leaflet. Combating myths and providing explanations, being careful to do so in a way that the patient understands, is a great way that pharmacists and their teams can make a difference and improve adherence. It means that teenagers are more likely to seek help from a pharmacy in the future.â€
Common conditions
Head lice
Head lice are very common in young children because of the frequency with which this age group has head-to-head contact. The main symptom is itching and there may well be nits (empty egg casings) visible. Treatment should only be carried out on individuals who have had at least one live louse on their head, with physical insecticides used first-line. A second application seven days later should kill any lice that have hatched since the first treatment. Wet combing using a metal, fine-toothed comb and plenty of conditioner is also popular, but is time-consuming to do properly and must be repeated every four days for at least two weeks.
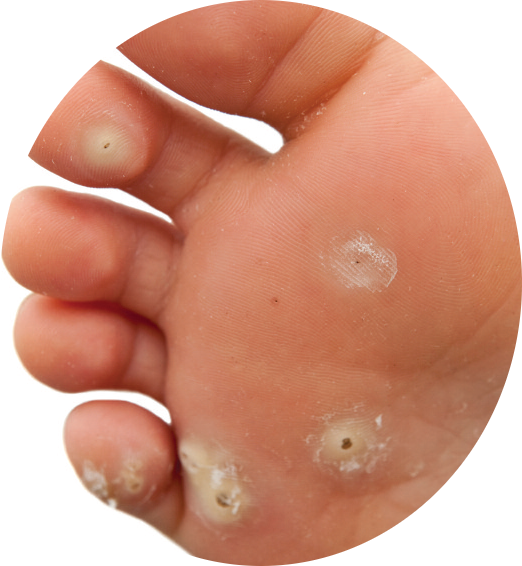 Warts and veruccas
Warts and veruccas
Warts and veruccas are caused by viruses and can be painful if pressed. They will resolve in time, but can be helped along by using products containing salicylic acid or silver nitrate, although perseverance is needed. Freezing treatments may be preferable in some cases, for example, for stubborn warts or if rapid relief is being sought, but can be painful to use. Preventative measures include not walking barefoot in wet areas, wearing flip-flops or verucca socks in communal areas, such as showers and changing rooms, and not sharing towels.
Athlete’s foot
Athlete’s foot is another problem that is often picked up in damp changing rooms and from swimming room floors, although it is caused by a fungus rather than a virus. It usually starts as soreness and itchiness between the fourth and fifth toes, becoming white, inflamed and weeping before sometimes cracking and peeling. If left untreated, athlete’s foot may spread to other areas of the foot and toenails. It should be managed by washing the feet daily with soap before drying them properly and applying a fungicidal (terbinafine is the only one available OTC) or fungistatic product (e.g. miconazole, tolnaftate or griseofulvin). The former kills the fungus if it is applied once or twice a day for a week, whereas the latter need to be used up to three times a day for two to four weeks for the infection to be cleared to the extent that it should not return.
Ringworm
Ringworm can affect people of all ages but requires skin-to-skin contact so is common in children. The fungal infection starts as small ring or oval-shaped patches on the skin with red, scaly edges, which may multiply and grow. The main symptom is itching. Antifungal treatment is needed (see athlete’s foot).
Fungal nail infections
Fungal nail infections are common in younger people who share communal showers due to sporting pursuits, with toenails more frequently affected than fingernails. A single nail may be affected, or several, with the nail appearing to be thickened or discoloured. As the infection progresses the nail may crumble or come away from the nail bed, causing discomfort. OTC treatments are available (e.g. amorolfine nail lacquer) but check before recommending or selling them as they may not be licensed for under 18s.
Acne
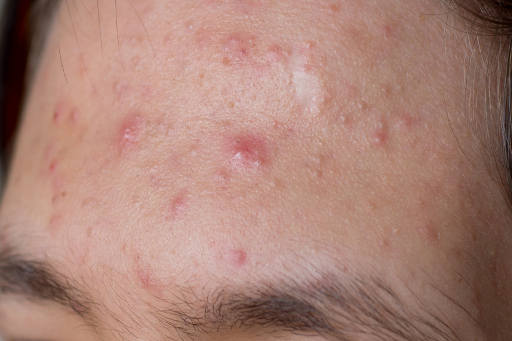 Acne usually starts at puberty and resolves by the mid-20s, but this is little consolation to teenagers who may become incredibly self-conscious and withdrawn as a result of their skin condition. Acne is triggered by the bacterium Propionibacterium acnes and most frequently affects the face, although the neck, back and chest are also commonly involved. There is no cure but symptoms can be managed using topical OTC products containing benzoyl peroxide, nicotinamide or salicylates. Sufferers can help themselves by resisting squeezing and picking spots, washing with a gentle cleaner and tepid water every morning and evening before patting skin dry, and regularly washing hair if it falls across the face.
Acne usually starts at puberty and resolves by the mid-20s, but this is little consolation to teenagers who may become incredibly self-conscious and withdrawn as a result of their skin condition. Acne is triggered by the bacterium Propionibacterium acnes and most frequently affects the face, although the neck, back and chest are also commonly involved. There is no cure but symptoms can be managed using topical OTC products containing benzoyl peroxide, nicotinamide or salicylates. Sufferers can help themselves by resisting squeezing and picking spots, washing with a gentle cleaner and tepid water every morning and evening before patting skin dry, and regularly washing hair if it falls across the face.
Dandruff
Dandruff, again so often associated with teenagers, is commoner in males than females and is caused by a build-up of dead skin cells on the scalp that cause characteristic white lumps and itching. Antifungal shampoos are effective and easy to use, but may need to be used on an ongoing basis to keep the problem at bay. Other measures that can help include avoiding prolonged blowdrying of hair, increasing the intake of vitamin B and essential fatty acids while reducing carbohydrates and sugar, and brushing hair regularly to encourage the shedding of dead skin cells. Encourage patients and parents to find out more about these conditions by referring them to websites such as NHS Choices and social media channels such as that produced by the Department of Health.
Â
Key facts
- It is important to check that the dose prescribed is suitable for the child’s age and weight
- Dosing errors can result from inadvertent changes in product strength
- Combating myths and providing explanations in a way that the patient understands can improve adherence.
