Clinical

Sun safety: Blue sky thinking
In Clinical
Let’s get clinical. Follow the links below to find out more about the latest clinical insight in community pharmacy.Bookmark
Record learning outcomes
The sight of the sun shining lifts the spirits but clear advice is needed to ensure customers balance their risks of skin damage with their vitamin D requirements.

Learning objectives
After reading this educational feature you should be able to:
- Advise customers on general sun safety measures
- Explain risk factors for skin cancer and help people decide if they are high risk
- Add value to your service by helping customers select appropriate products to protect their skin.
Â
With more than 14,000 new cases diagnosed each year, malignant melanoma is the UK’s fastest growing cancer. It is, however, a rare condition – non-melanoma skin cancer (NMSC) accounts for nearly 100,000 new cases each year, according to conservative estimates.
Ultraviolet (UV) radiation from the sun is the main potentially avoidable risk factor for skin cancer, linked to an estimated 86 per cent of malignant melanoma cases in the UK.1 It also plays a critical role in NMSC. When considering sun safety, UV protection must be balanced against the need for adequate UVB for vitamin D synthesis.
Most NMSCs and many melanomas can be removed safely if identified early, so regular skin examination is important. This feature uses a scenario-based format to answer common queries and dispel myths about sun safety and skin cancer risk.
Lisa and her friends are planning a three-week sailing trip this summer...
The amount of sun protection required depends partly on a person’s skin type. Darker skin contains more melanin, the pigment that gives skin its colour and is a natural UV protector. Clinicians divide skin into six categories depending on its propensity to tan or burn in the sun (see Figure 1 below). At one end, type 1 skin (northern European type) is pale, very UV-sensitive and always burns; at the other end of the scale, type 6 skin (African type) is dark, UV-resistant and always tans.
Figure 1:Â Skin type classifications
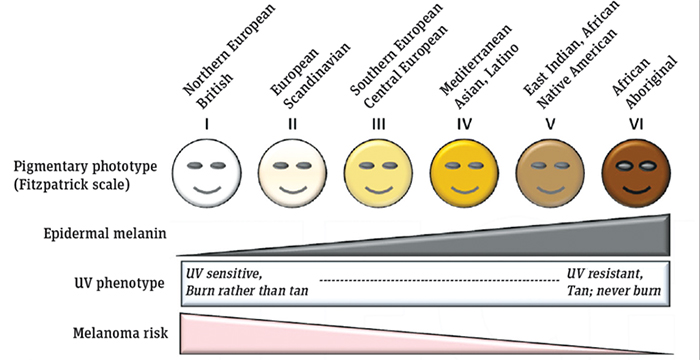
Source: D’Orazio JA, Jarrett S, Marsch A, Lagrew J, Cleary L (2013). Melanoma – Epidemiology, Genetics and Risk Factors, Recent Advances in the Biology, Therapy and Management of Melanoma, Dr Lester Davids (Ed.) ISBN: 978-953-51-0976-1, InTech, DOI: 10.5772/55172. Available here.Â
Sunscreen products contain organic UV filters (chemicals that absorb UV light) and inorganic (mineral) filters, such as titanium dioxide, that reflect UV light. The level of protection given by the product is described by the sun protection factor (SPF). For example, if it takes 20 minutes for someone’s unprotected skin to start to burn (turn red), a SPF15 cream will protect them for 15-times longer (i.e. about five hours). However, to achieve this, it must be applied at a concentration of 2mg/cm2. In practice, this means about 35ml or two tablespoons for the whole body.
The SPF relates only to protection against UVB light, which is primarily responsible for burning. UVA radiation causes skin ageing and also contributes to DNA damage (and therefore to the risk of skin cancer).
It is easy to tell when skin has had too much UVB because it reddens and becomes sore and inflamed. This does not happen with UVA and it is important to choose a sunscreen that provides good UVA protection. Such products are now labelled with a symbol showing the letters UVA in a circle (or are labelled, ‘EU compliant’). This denotes that the UVA protection is at least one-third that of the labelled SPF.
Some manufacturers still use the 1-5 star rating as well – the more stars, the better the UVA protection. For example, if a product has a SPF of 30 and UVA star rating of 3, it will provide UVA protection of about 60 per cent of the SPF value – about 20.
The European Commission has recently simplified the labelling of sunscreens into four protection categories – low (SPF 6-10), medium (SPF 15-25), high (SPF 30-50) and very high (SPF 50+).
Choosing the right product for an individual depends on propensity to burn (e.g. skin type; use of photosensitising medicines) and the risks of skin cancer (skin type; previous history of skin cancer/precancerous lesions; organ transplant recipients; HIV-AIDS). Lisa and her friends should also be reminded that UV radiation penetrates clouds, so it is possible to burn on a cloudy day. In addition, UV radiation is reflected from the sea surface, so they may be getting more UV than they think.
People commonly use about half the amount of sunscreen that is required. Some experts advise using two applications – one before going out in the sun and another afterwards. Sunscreen should be reapplied after two hours to maintain adequate protection – earlier after swimming or towelling. No sunscreen product offers 100 per cent protection, so the terms ‘sunblock’ and ‘100 per cent protection’ have now been banned. Sunscreens should always be used in conjunction with other common sense UV protection measures – often summarised as the five S’s of sun safety:
- Slip on a T-shirt
- Slop on SPF30+ broad spectrum (UVA and UVB) sunscreen
- Slap on a broad-brimmed hat
- Slide on sunglasses
- Shade from the sun whenever possible.
Young man planning a cycling holiday in Devon and Cornwall...
Even in the UK, sun safety is an important consideration. One way to gauge how much protection is needed is to check the UV index that indicates how much UV radiation is reaching a geographical area. The value ranges from one to 11+; when the index is 3 or more, there is enough UV to damage skin and therefore sunscreens are required.
The Met Office website publishes daily UV forecasts, while the British Association of Dermatologists (BAD) has a free app that allows users to check the UV index on a given day anywhere in the world (see Met Office: UV and sun health.)
A couple are taking their two young children for a summer holiday in Majorca...
The skin of very young children is delicate and burns easily. Blistering sunburn in childhood can double the risk of melanoma in later life. In addition to using a high-factor (at least SPF30) broad-spectrum sunscreen, parents should be advised to protect children’s skin from the sun by using long-sleeved T-shirts and sunsuits/swimsuits that cover the neck and shoulders. A widebrimmed hat and wrap-around sunglasses should also be used. Whenever possible children should play in the shade, especially around midday when solar radiation is most intense.
If a child’s skin (or anybody’s skin) starts to burn, it is important to act quickly. Cover the skin or get under shade and cool the skin by taking a tepid shower or using a wet flannel. Drinking plenty of water will help with the cooling process and help to avoid dehydration.
Good quality moisturising after-sun products can be helpful to soothe the skin and relieve feelings of tightness and/or itching. They should be smoothed on lightly and not rubbed as the skin might already be sore and tender. Topical antihistamines and local anaesthetics should not be used because of the risk of hypersensitivity reactions.
Routine sun protection for children is also important in the UK. Sun Safe Schools is an accreditation scheme run by the charity Skcin, which is designed to prevent skin cancer through education. “We advocate the provision of sunscreen dispensers in primary school classrooms and sun awareness aids because that starts good habits early,†says Marie Tudor, business development manager for Skcin (see Sun Safe Schools).
New online test to predict risk
A new online tool (the Qskin risk calculator) has been devised to predict the risk for people aged 40 years and over of developing non-melanoma skin cancer (NMSC) – basal cell carcinomas (BCCs) and squamous cell carcinomas (SCCs) – over the next three years.
Although BCCs and SCCs are common cancers, until now there has been no reliable way of predicting an individual’s risk of developing them.
Researchers at the Berghofer Medical Research Institute in Queensland, Australia, analysed data from 39,000 people aged 40-70 years to identify the most important risk factors. The test computes a risk level from the responses to 10 questions about risk factors for skin cancer, including age, gender, smoking status, skin colour, tanning ability, freckling tendency, and other aspects of a person’s medical history. It is hoped that the test will help to identify those at high risk so that they can be monitored appropriately.
The test is not a substitute for visiting a doctor or skin cancer clinic and it does not estimate the risk of developing a melanoma. If it indicates that someone has a high risk of skin cancer, they should consult their doctor. The test can be accessed here.
Rina keeps most of her skin covered for cultural reasons and is now moving to Aberdeen...
Rina is at risk of developing vitamin D deficiency. Vitamin D is synthesised in the skin through the action of UVB.
It is essential not only for healthy bones but also for heart, muscle and skin function. Vitamin D is available from certain foods including fish, milk, egg yolks and fortified cereals but exposure to sunlight is the most efficient way to boost levels. It is estimated that about 15 minutes of sunlight a day on unprotected skin (e.g. arms and face) is enough to meet the body’s vitamin D requirements. However, in the UK, from mid-October until the beginning of April, there is insufficient UVB for skin synthesis.2
Rina is at risk of vitamin D deficiency (defined as less than 25nmol/litre) because her skin is covered most of the time and because she is moving to live in a northerly region where sunlight is less intense. She should be advised to take a daily vitamin D supplement of 10 micrograms. Other groups of people who may be at risk of vitamin D deficiency include infants and children under five years of age, pregnant and breast-feeding women, people with dark skin and people over the age of 65 years.
A woman with pale skin and a lot of moles...
Having many moles is a risk factor for melanoma, but most moles are normal. A mole that is changing or growing can be a sign of melanoma development. Everyone should learn to examine their skin for signs of skin cancer and seek medical advice if changes are found. The ABCDE mole checklist is a useful reminder of what to look for:
- A: Asymmetry
- B: Border – irregular of jagged edges
- C: Colour – uneven, black, brown, bluish
- D: Diameter – wider than 6mm
- E: Enlargement – growing or raised.
At-risk individuals should have an annual check by a doctor.

Â
Tracy has eczema and is looking for a suitable sunscreen...
People with eczema are usually careful to avoid products that could contain irritants that trigger a bout of eczema. A number of sunscreen products are now available that have been formulated specifically for sensitive or atopic skin.
“Sunscreens are like emollients – there is no ‘one-size-fits-all’ product,†says Julie van Onselen, independent dermatology nurse specialist. “If you have eczema, it is a good idea to buy two or three small (travel-size) packs and try them before going on holiday to find what suits your skin.â€
Another common question is how to use emollients and sunscreens together. “We recommend applying the emollient first, as usual, and then applying the sunscreen about 30 minutes later when the emollient has been absorbed,†she says.
- The National Eczema Society has a useful factsheet on sunscreens and recommends the use of mineral (titanium dioxide) sunscreens (see National Eczema Society: factsheets to download).
Different types of skin cancer
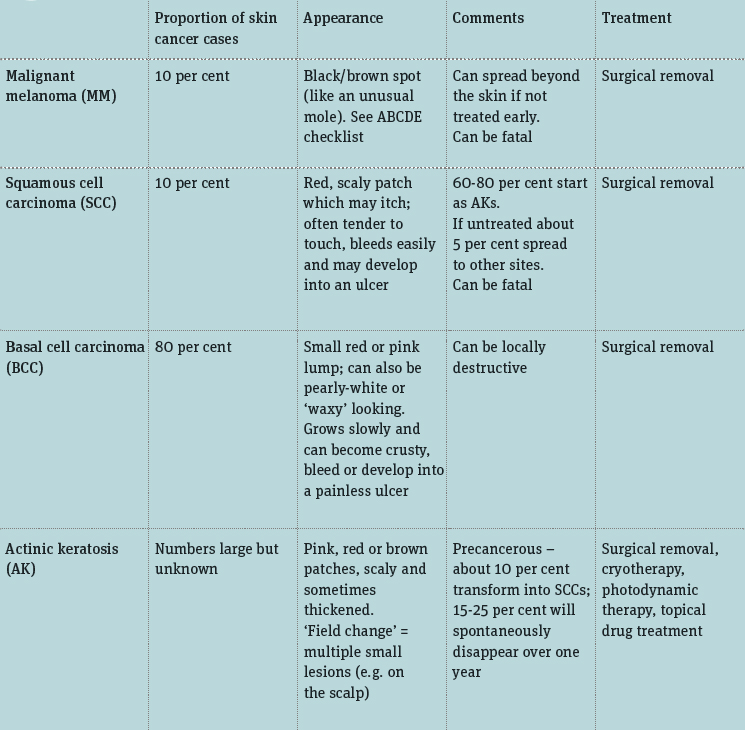
Non-melanoma skin cancers (NMSCs) is a group that includes squamous cell carcinomas (SCCs), basal cell carcinomas (BCCs) and the pre-cancerous actinic keratoses (AKs)
Â
Brian, 52, has undergone a kidney transplant and is planning to spend more time on his allotment...
People who have undergone organ transplants are routinely immunosuppressed and at high risk of developing skin cancer. They are 250-times more likely to develop an actinic keratosis (a pre-malignant lesion) than immunocompetent individuals3 and have a 100-fold higher risk of developing invasive squamous cell carcinomas (SCCs).
“Not all people with transplants are aware of the risks of skin cancer,†says Fiona Loud, policy director of the British Kidney Patient Association. “They need to be reminded and educated about avoiding UV exposure. Another problem is lack of clarity about which products to use. Transplant patients should be advised to apply a factor 50+ sunscreen to all exposed skin every day, summer and winter.â€
Transplant patients should also be having twice-yearly skin examinations by a dermatologist and it is important that these are not missed, she adds.
Brian should be advised to keep his skin covered when outdoors and to use a sunscreen (SPF50+) on exposed skin. He should discuss with his GP the possibility of having a prescription for a sunscreen.
A young woman likes to have regular sunbed sessions “to keep a healthy tanâ€...
The UV radiation from some sunbeds can be more than 10-times stronger than the mid-day Mediterranean sun. One use of a sunbed in someone with type 1 or 2 skin colouring under the age of 35 years increases the lifetime risk of melanoma by 75 per cent, says Dr George Moncrieff, GP and chair of the Dermatology Council for England. Sunbed use is believed to be a contributory factor in the recent increase in the incidence of melanoma in women in their 20s.
Sunbeds provide short, intense exposure to UVA radiation that induces DNA damage and causes premature ageing of the skin. A tan from a sunbed provides little protection against sunburn from sunlight but it causes irreversible damage that is not obvious in the early stages. It is safer to use a fake tan.
Use of sunbeds by under-18s is illegal in the UK. “We remain concerned that this is difficult to enforce. We know of cases of 16-year-olds paying for sunbed sessions with their pocket money,†says Marie Tudor of Skcin.
References
Â
Further reading and links
- Actinic keratoses and skin cancer. Pharmacy Magazine CPD Module 231. January 2015
- Sunlight exposure: risks and benefits. NICE guideline. February 2016.
- The Karen Clifford Skin Cancer Charity provides detailed and authoritative information about skin cancer and sun protection.Â
- The British Association of Dermatologists provides a number of information leaflets on vitamin D and skin cancer.
- The National Eczema Society produces a range of factsheets on sun and eczema.
